All published articles of this journal are available on ScienceDirect.
Two-year Follow-up of Avulsed Teeth Submittted to Laser Therapies: A Case Report
Abstract
Background:
Replanted teeth can lead to critical biological conditions involving ankylosis and external root resorption. To prevent these occurrences, antimicrobial Photodynamic Therapy (aPDT) and Photobiomodulation Therapy (PBMT) can be used during the postoperative phase.
Case Report:
The present report described the clinical case of a patient, an adult male with the avulsion of teeth #11 and #21. Teeth were stored under dry conditions and replanted 18h after trauma. The pulp was removed before replantation and aPDT was performed using a low power laser (660 nm,100 mW, 9 J) in direct irradiation of the root canal. A passive flexible splint was fixed in place from tooth #13 to #23 for 4 weeks. The PBMT was applied three times a week, for the first 2 months, using the same laser device but with an infrared wavelength (808 nm, 100 mW, 3J). Clinical and radiographic examination supported the assessment of inflammatory/infectious resorption.
Conclusion:
The combination of laser therapy with endodontic procedures for treating traumatized teeth ensured successful clinical and radiographic outcomes at a 2-year follow-up examination.
1. INTRODUCTION
The rate of traumatic dental injuries is high in children and young adults, justified by the fact that this group is more susceptible to accidents generated by factors such as sports and routine causes (falls from their height, school games and physical education classes) [1]. Traumatic avulsion of teeth involves severe aggression to the gingiva, periodontal ligament, and pulp. In most cases, injuries occur in permanent teeth (0.5 to 3%), commonly in children and young adults, since a rather elastic alveolar bone offers low stability to extrusive forces [2]. One of the main complications secondary to the replantation of avulsed teeth is ankylosis, which may manifest through external root resorption [3]. A retrospective study with cases of avulsed teeth verified that 8% of external root resorption was present in 70% of cases, superficial resorption was observed in 10%, reabsorption by substitution in 10% and ankylosis in 10%. Relative to complications affecting the pulp, pulp necrosis was found after 4 weeks of follow-up, and internal root resorption, after one year [4]. Both antimicrobial Photodynamic Therapy (aPDT) and Photobiomodulation Therapy (PBMT) using low power laser can be used during the postoperative phase to reduce the local bacterial load and accelerate the healing process (by affecting cellular metabolic processes), respectively [5, 6] to prevent these occurrences. Photobiomodulation Therapy (PBMT) is based on applying light emitting diodes from LASERS or LEDS to promote pain control, modulation of inflammation, and tissue repair. The primary target of PBMT is cytochrome c oxidase - a photoreceptor in the mitochondrial respiratory chain. This chromophore induces the development of ATP (adenosine triphosphate) attending to cell response, which in turn will advance crucial cell activities to tissue repair (metabolic activity, proliferation, migration, and differentiation) [7]. Antimicrobial photodynamic therapy (aPDT) consists of a technique in which the low-power laser is also used; however, in this case, the aim is to reduce the bacterial load. The technique associates the application of a photosensitizer (PS) in the damaged region for a period of time (called irradiation time) with the subsequent use of light with a wavelength similar to that of the PS. In the presence of oxygen, the PS contributes immense quantities of reactive oxygen species (ROS), killing microorganisms [8]. According to a systematic review [9] published in the Cochrane Library, few randomized clinical trials still demonstrate the effectiveness of the treatment protocol applied in cases of dental trauma. To date, there are no clinical reports of the effect of photobiomodulation therapy using low-power lasers and aPDT on traumatized teeth. The present report aimed to describe a clinical case in which both PBMT and aPDT were used as ancillary treatments, contributing to the preservation of teeth in a clinical case with delayed tooth replantation.
2. CASE REPORT
2.1. Clinical and Radiographic Examinations
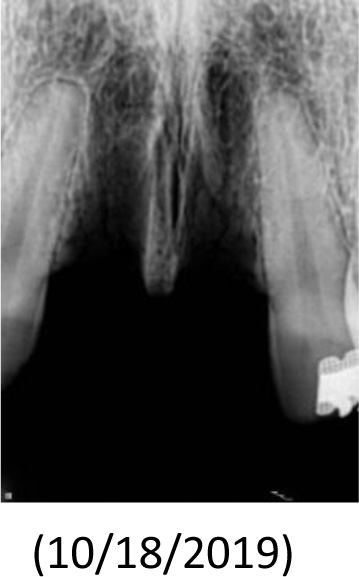
The patient, a 25-year-old man, was referred to the Dental Trauma Clinic of the School of Dentistry of the University of São Paulo (USP) 18h after suffering facial trauma caused by a motorcycle accident. The patient had no history of systemic disease and did not use any medication before the clinical appointment. Clinical and radiographic exams revealed several traumatic dentoalveolar conditions in teeth #11 and #21, as shown in Fig. (1). No other oral injury was identified in the clinical diagnosis. The avulsed teeth exhibited necrotic periodontal ligament cells due to the continued storage in dry conditions.
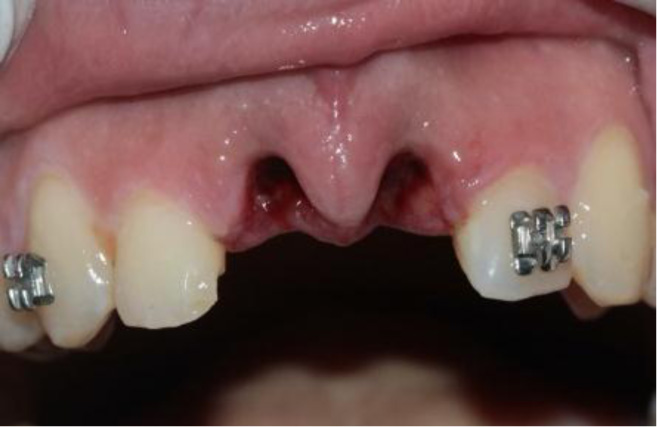
2.2. Tooth Cleaning, Intervention, and Preparation
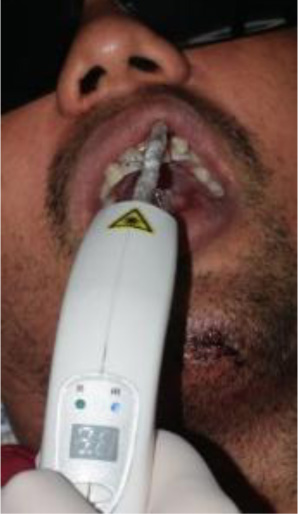
The avulsed teeth were submitted to root planing with an ultrasonic point to remove the necrotic periodontal tissue. Root canals were irrigated with 3 mL of 2.5% NaOCl solution. After cleaning the root canals, antimicrobial Photodynamic Therapy (aPDT) was performed by irrigation with 0.005% methylene blue solution that was retained in the root canal for 5 minutes before using the laser light. Subsequently, the flexible optical fiber was inserted into the root canal. Guided irradiation was performed with a low-power laser (Therapy XT® DMC, Brazil) emitting at 660 nm, using the following parameters: 100 mW, 9 J energy, 90 s, 0,028cm2 of spot size, and continuous emission (Table 1). A 600 μm light diffuser tip was connected to the laser and was inserted up to 1 mm from the tooth apex to ensure that light reached the major portion of the root canal. After laser irradiation, the root canals were irrigated with 3 mL of 17% EDTA followed by 3 mL of 2.5% NaOCl to remove the residual methylene blue solution. Finally, paper points were used to dry the root canal surfaces. In conclusion, the root canals were filled with calcium hydroxide and restored with a glass ionomer cement. The aPDT, PBMT, medication, and temporary restoration were changed monthly for 8 months (Fig. 2).
| Wavelength (nm) | Power (mW) | Energy Per Point (J) | Time (Sec) |
Energy Density ( J/cm2 ) |
Power Density (mW/cm2 ) | Spot Size (cm2) | The Frequency of Treatment |
| 660 | 100 | 9 | 90 | 3214.29 | 35714.29 | 0.028 | Once per month during 8 months |
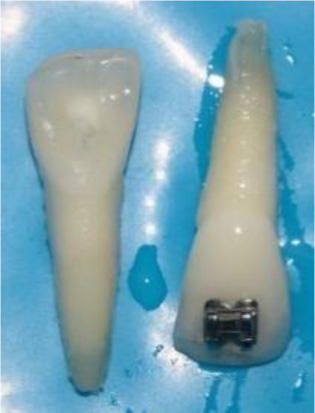
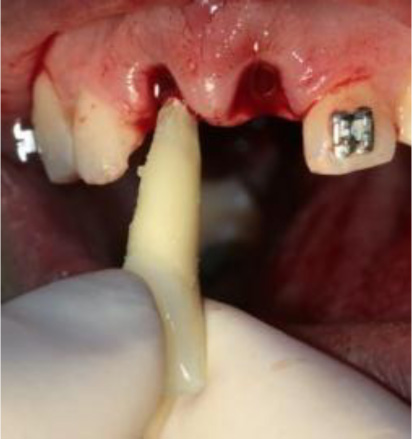
2.3. Teeth Replantation and Splint (intra-orally)
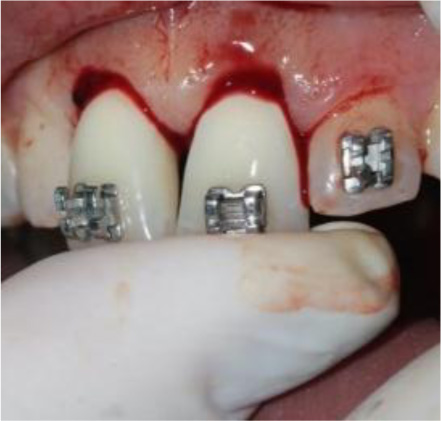
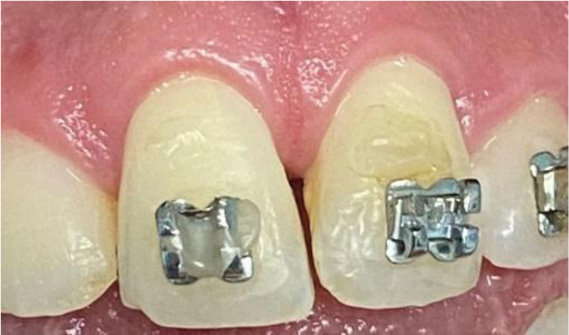
After root canal treatment and replanting of the teeth, local anesthesia was used to rinse and remove the contaminated coagulum from the sockets. Functional splinting with orthodontic 0.016 archwire and composite resin was fixed from tooth #13 to tooth #23 (Figs. 3-5). The splint was removed 1 month later.
2.4. Photobiomodulation Therapy (PBMT)
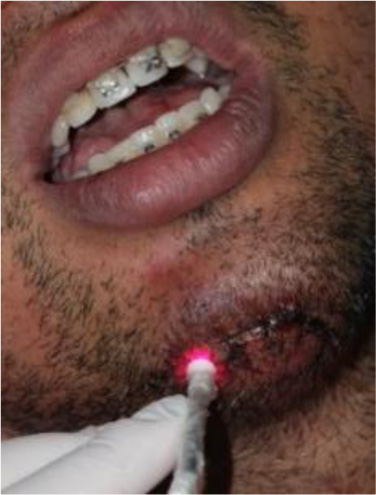
The PBMT was done constantly applying the same laser device but with an infrared wavelength (808 nm) with the following parameters: 100 mW, 0,028 cm2, 30 s, 3 J per point, and 33.33J/cm2 (Table 2). PBMT was performed in contact mode with the target tissue and punctually, consisting of 3 points of application: one in the middle third of the vestibular surface of the dental crown, one at the buccal bone plate (correlating to the nearest location of the dental apex) and one at the palatal bone plate (correlating to the nearest gingival margin) (Figs. 6 and 7). The irradiations were performed for 5 days in the first week (daily application), 3 days in the second week (time interval of 48h), 2 days in the third week (time interval of 48 h) and 1 day in the fourth week. After the first month, the irradiations were applied monthly, and so was the aPDT (Fig. 8).

2.5. Root Canal Filling
After 8 months of laser therapy, the root canals were filled with gutta-percha cones and a bioceramic sealer. The teeth were restored with composite resin, and occlusal adjustments were made. (Figs. 9-14).
| Wavelength (nm) | Power (mW) | Energy Per Point (J) | Time (Sec) |
Energy Density ( J/cm2 ) |
Power Density (mW/cm2 ) | Spot Size (cm2) | The Frequency of Treatment |
| 808 | 100 | 3 (3 points) | 30 per point | 33.33 | 1111.11 | 0.09 | 1. Five days in the first week 2. Three days in the second week 3. Two days in the third week 4. One day in the fourth week 5. After the first month, the irradiations were applied monthly (7 times) |
3. DISCUSSION
The treatment of an avulsed tooth depends on the extent and time when the tooth was dislodged from its socket. A tooth with a completely developed root can be reimplanted in its socket immediately if any contaminants or debris on its surface has been removed. Root resorption can be prevented in 90% of cases if the avulsed tooth is replanted within 30 minutes after avulsion, followed by root canal therapy within 3 to 4 weeks after reimplantation [10, 11]. For avulsed teeth, the recommendation is to perform root canal therapy within an adequate time interval. Traumatic dental injuries to the tooth can result in local pulp necrosis, alveolar damage, traumatic occlusion, and tooth resorption. When a tooth has been exposed to an extra-oral dehydration time of longer than 60 minutes, the periodontal ligament is not expected to survive. Before replantation of this tooth, its pretreatment will make it more resistant to resorption/strengthen it and enable it to withstand resorption. If the tooth remains dry for longer than 60 min, without considering the preservation of the periodontal ligament, endodontic therapy can be performed intraorally [10].
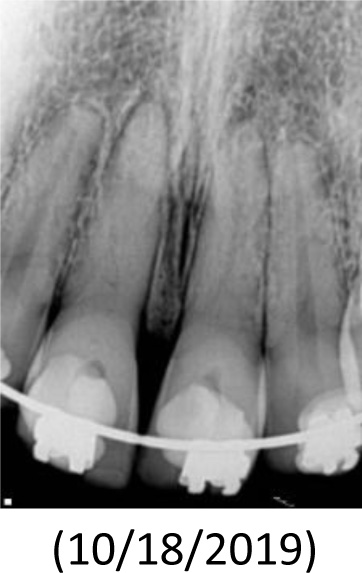
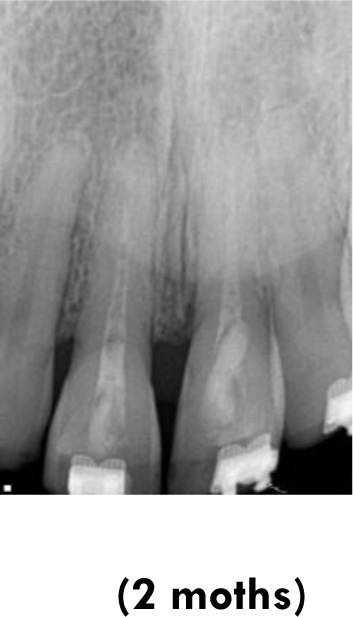
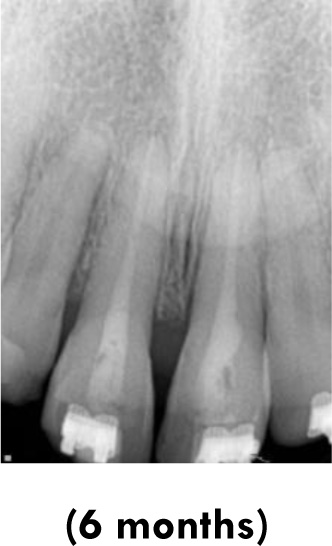

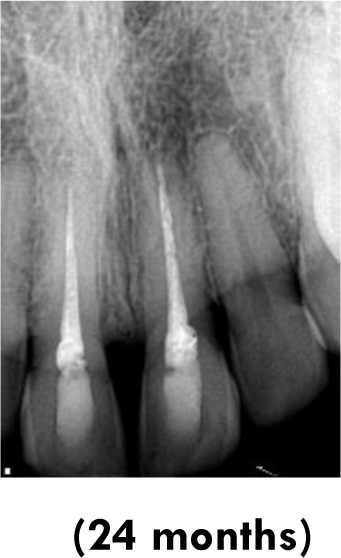
In the present case report, considering the time of approximately 18 hours spent outside the oral cavity, without storage in any solution and any pretreatment, the prognosis predicted was poor. Moreover, one study [11] detected that the danger of premature resorption was increased in teeth that suffered further damage or root contamination or that were stored in dry conditions for longer than 1hour. They reported that the drying time was the most difficult clinical factor associated with the development of post-replantation root resorption. Therefore, therapies that would assist tissue repair and antimicrobial action were considered important.
According to the International Association of Dental Traumatology (IADT), reimplantation of avulsed permanent teeth with an open apex with an extra-oral time longer than 60 min is not indicated [12]. Trope [13] alleged that when relevant added damage cannot be avoided and root replacement by bone will occur, procedures are performed to delay the root replacement by the bone to retain the tooth in the mouth for as long as possible. In this situation, therefore, adequate treatment was performed. Initially, the root canal was carefully disinfected, and then the canal was filled with calcium hydroxide to avert inflammatory external root resorption [14]. Longitudinal case reports and clinical studies have verified that in cases of avulsed teeth, using calcium hydroxide has resulted in extraordinarily high estimated success rates [15]. On the contrary, long-term calcium hydroxide treatment may have some harmful effects. This treatment requires several clinical visits that prolong treatment over a long period of time, making patient collaboration a critical factor. Without the patient's collaboration, the probable loss of teeth could be inevitable [16]. According to a recent systematic review, aPDT can be used as an adjunct in treating infectious diseases. Using photosensitizers such as methylene blue, combined with irradiation with a diode laser (630 and 650 nm) has shown significant results for treating infectious diseases and in bactericidal scenarios [17]. The benefits of PBMT have been shown in many areas of health sciences, including enhanced tissue repair, modulation of the inflammatory process, and pain control, resulting in achievements that suggest an appreciable capacity for its use intraorally [18]. The antimicrobial photodynamic therapy (aPDT) was administered because it was a non-invasive therapy, in which the association of an adequate light source with low energy, oxygen, and a photosensitizer (PS) was capable of producing reactive oxygen species (ROS) and leading to a reduction in the local microbial load. These PSs have chemical and physicochemical analogs and a salient cationic load allowing permeation into the outer membrane of gram-negative bacteria, indicating a high degree of selectivity for destroying microorganisms [19]. The effect of irradiating the lesion stained with the PS is the production of ROS along with singlet oxygen (SO). SO is highly cytotoxic, leading to microorganism cell destruction and death. Studies have suggested the potential use of aPDT to improve disinfection during nonsurgical treatment [20]. Therefore, in the present case, the authors considered the aPDT in the extraoral step of the treatment before tooth reimplantation to reduce the bacterial load.
The primary target of PBMT is cytochrome c oxidase - a photoreceptor in the mitochondrial respiratory chain [7]. As a photoreceptor, these chromophores prompt the growth of cellular energy (higher production of ATP), leading to cell response, which improves cell proliferation, metabolic activity, differentiation, and migration. It is also notorious that PBMT has biomodulator action on osteoclasts, fibroblasts, and keratinocytes and improves tissue repair and angiogenesis [21, 22]. PBMT also increases collagen production and other proteins in the extracellular matrix [23]. Trindade et al. (2006) studied the effect of PBMT on treating teeth with apical periodontitis and showed reduced rates for neutrophils/eosinophils in the group receiving root canal therapy and laser when compared with the group receiving root canal treatment alone [24]. Therefore, PBMT can advance tissue repair by fine-tuning the inflammatory process [25]. Another research analyzed the effects of PBMT and dental pulp-capping materials on the procreation of L-929 fibroblasts. The authors demonstrated that in all culture mediums of fibroblasts alone, fibroblasts and calcium hydroxide, fibroblasts and resin, the laser caused a higher quantity of increase in fibroblast when compared with the group in which samples were not submitted to irradiation [26]. The absence of agreement about the delivery of a standardized protocol for PBM therapy is partly due to the scarcity of precisely described materials and methods, which are crucial for reproducing individual studies [27]. To obtain higher levels of certain outcomes, complete acknowledgment of these aspects is important. Moreover, extensive knowledge of laser parameters, tissue volume, and target depth is required to deliver an adequate dose within the current guidelines [28]. A study conducted by Bahman et al. (2020) investigated the process of apexogenesis of immature permanent dog teeth when performed with calcium hydroxide and Photobiomodulation therapy (PBMT) [29]. The authors reported that the association of calcium hydroxide with PBMT could have good effects on the process of apexogenesis. Their study demonstrated that PBMT was shown to have more effects on the process of dentinogenesis in a period of 2 weeks, and this effect was notably different from the 7th day onwards. In these conditions, both aPDT and PBMT were effective for distinct clinical applications in endodontics. For the first time, the two above-mentioned treatments were shown to improve healing, modulate inflammation, control pain, and reduce the bacterial load when treating traumatized teeth. Nevertheless, controlled and randomized clinical studies addressing the use of low-power lasers on traumatized teeth are needed to contribute to the clinical use of the technique.
CONCLUSION
The use of therapy focused on disinfection, combined with aPDT and PBMT for treating severe avulsion, ensured successful outcomes in the clinical and radiographic 2-year follow-up examinations, showing how promising these techniques are in the context of dental trauma.
LIST OF ABBREVIATIONS
| PBMT | = Photobiomodulation Therapy |
| PS | = Photosensitizer |
| ROS | = Reactive Oxygen Species |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals were used that are the basis of this study.
CONSENT FOR PUBLICATION
A term of free and informed consent was obtained from the patient.
STANDARDS OF REPORTING
CARE guidelines were followed.
AVAILABILITY OF DATA AND MATERIALS
Not applicable.
FUNDING
This study was funded by FAPESP 2018/21696-7.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
The author would like ti acknowlege the supplement from FAPESP-SÃO PAULO- BRAZIL.


