All published articles of this journal are available on ScienceDirect.
Aging Protocols and Their Effects on Bond Strength of Total-Etch and Self-Etch Adhesive Systems to Dentin
Abstract
Objective:
This study investigated whether different aging protocols have effects on the bond strength of total-etch and self-etch adhesive systems to dentin substrate.
Methods:
Molars were sectioned exposing the dentin, which was submitted to restorative procedures using two-step total-etch (ASB, Adper SingleBond2), two-step self-etch (CLF, Clearfil SEBond), or one-step self-etch (OPT, Optibond All-in-One) system and resin composite. The obtained blocks were sectioned to result in sticks to be submitted to bond strength and failure mode tests after 24h storage in distilled water (DW), or 180-day aging protocols in DW, artificial saliva (AS), citric acid (CA), or thermal cycling (TC). The types of failures were classified as adhesive, cohesive in dentin, cohesive in composite resin, and mixed. Data were analyzed using ANOVA followed by Tukey’s test (α=5%). The failure modes were descriptive under the relative frequencies form.
Results:
It was observed that ASB presented the higher bond strength(p<0.05), while CLF and OPT did not demonstrate differences between them(p>0.05) after 24h. The bond strength obtained with ASB significantly overcame that of OPT when stored in DW or AS for 180 days (p<0.001). In these storing mediums, ASB did not differ from CLF(p>0.05), while in CA or TC the values of CLF were significantly lower (p<0.001). In TC aging, the values presented by OPT did not differ from ASB(p>0.05), both of which had higher values than CLF(p<0.05). The predominant failure mode was adhesive.
Conclusion:
For the two-step total-etch and two-step self-etch adhesives, the influence of aging in AS and TC was equivalent to that of storage in DW. The most deleterious effects occurred in CA, a situation in which self-etch adhesives displayed worse performance than the conventional type.
1. INTRODUCTION
One of the greatest challenges in dentistry has been to promote an efficient and durable bond between dentin substrate and adhesive restorative materials. This bond that is established in a micro-mechanical way substantiates itself on the process of demineralization of the hard dental tissues and on the infiltration in the micropores formed by resinous monomers, constituting hybridization [1]. The hybridization process may be affected by various aspects, among which the type of adhesive system used is highlighted [2].
Two-step total-etch adhesives represent simplified systems that require pretreatment with phosphoric acid at 37% [3]. In these products, the hydrophilic components of the primer and the hydrophobic components of the adhesive are chemically balanced and gathered in one vial [3]. The self-etch adhesive systems, which dismiss the prior application of phosphoric acid, represent an alternative to the conventional adhesive systems. The self-etch adhesive systems can be commercially presented in two steps, in which the conditioning agent and the primer are combined in one vial and the adhesive is applied separately; or in one step, in which acid, primer, and adhesive are combined in one application [4].
In order to compare the performance of different adhesive systems, in vitro protocols have been used, where, in the majority, the bond strength (BS) to the dentin substrate is tested right after preparing the restoration in resin composite [2, 5]. However, these studies provide limited data because it is important to investigate the bond over a long period of time [6-8], particularly because the dentin/adhesive/resin interface suffers degradation by physical, mechanical, and chemical processes in the oral cavity [9].
From a physical point of view, hydrothermal tests, which cause hydrolysis of components on the adhesive interface [10], have been largely used to proportionate degradation or aging. It has already been shown that the BS can be reduced by approximately 40% with thermal cycling (TC) [5, 11], but on the other hand, studies did not observe a significant effect of TC [12, 13].
When storing samples in distilled water (DW), the literature generally uses the times of 24 h or six months and points out that the BS may reduce, especially after six months of storage [13, 14]. However, there are reports that the BS values of the dentin/adhesive/resin interface are not affected by the time stored in DW [14, 15]. Other studies utilizing artificial saliva (AS) as immersion storage have demonstrated differences in the BS when comparing the storage times of 24 h and six months [15, 16]. In addition to the effects of DW and AS, acids such as citric acid (CA) may affect the BS of the adhesive systems to dentin in an erosive manner [9].
Considering that in vitro studies represent a valuable model to understand the performance of adhesive systems in a controlled manner [17], and it is important to submit the dentin/adhesive/resin interface to degradation processes so that there is greater proximity to the clinical reality, this study assessed whether different aging protocols have effects on the BS of total-etch and self-etch adhesive systems to dentin substrate, and their respective failure modes. The null hypothesis tested was that BS of total-etch and self-etch adhesive systems were not influenced by different storage solutions.
2. MATERIALS AND METHODS
2.1. Experimental Design
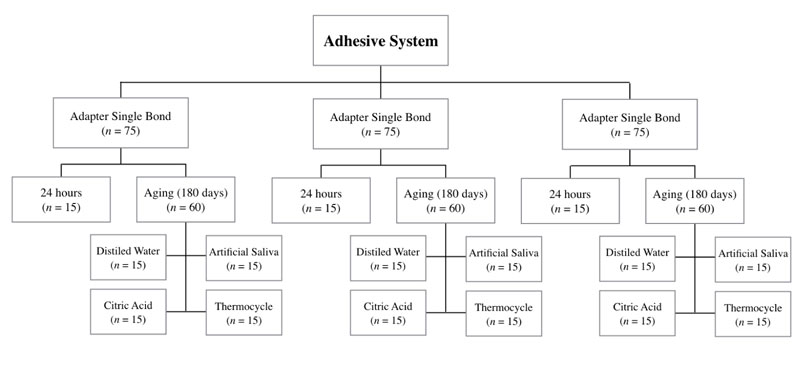
The experimental design is detailed in Fig. (1). This study was designed using two study factors: (1) adhesive system: two-step total-etch (ASB; Adper Single Bond 2, 3M/ESPE, St. Paul, Minnesota, USA), two-step self-etch (CLF; Clearfil SE Bond, Kuraray Noritake, Okayama, Okayama, Japan), or one-step self-etch (OPT; OptiBond All-in-One, Kerr, Orange, California, USA); (2) 24 h of immersion in DW or 180-day aging protocol using DW, AS, CA (erosive challenge), and TC. Healthy third molars (n = 180) were used to obtain specimens of dentin to be submitted to restorative techniques with resin composite using ASB, CLF, or OPT, according to the manufacturer’s instructions.
As inclusion criteria, the teeth must not have any wear, fracture or restoration. The sample size was determined to yield statistically significant results and was estimated based on the previous study [5]. Forty-eight teeth for each experimental group were required to have a power of 80% and significance α = 5%. The sample size was increased to become sixty teeth (n = 60) with a dropout rate of 20%. Each block of dentin/adhesive/resin was submitted to serial cuts to obtain sticks, which were stored in DW for 24 h or submitted to 180-day aging protocols (DW, AS, CA, or TC). As response variables, the microtensile BS in megapascal (MPa) and failure mode were measured.
2.2. Selection and Preparation of the Teeth
After approval by the Local Research Ethics Committee of Faculty Dentistry Sao Leopoldo Mandic (protocol #1.110.952) and after written informed donor patients’ consent, 180 healthy, recently extracted human third molars were obtained. The teeth were cleaned with a periodontal curette (Duflex, SS White, Lakewood, New Jersey, USA) and maintained in a 0.1% thymol solution [18]. For the selection process, the teeth were previously examined under a stereomicroscope with 40x magnification (Quimis, Q7766P, Diadema, São Paulo, Brazil), excluding teeth carious lesions, cracks, or hypoplasia.
Sectioned teeth were randomly separated and sectioned on the middle-third of the coronary portion, at the height of the amelo-dentin junction of the central sulcus, perpendicular to its long axis, using a precision cutting machine (Isomet 1000, Buehler Ltd., Lake Bluff, Illinois, USA) assembled with a diamond disc (Diamond Wafering Blades, Erios, Ipiranga, São Paulo, Brazil) at low speed, underwater refrigeration, performing cuts on the occlusal and root portions. This procedure enabled the acquisition of smooth and flat occlusal dentin specimens, with medium depth in all the teeth.
2.3. Adhesive System Application and Restorative Technique
The dentin specimens were submitted to restorative techniques using one of the three adhesive systems tested: ASB (n = 60), CLF (n = 60) or OPT (n = 60).
For the two-step etch adhesive system, the etching was conducted with 37% phosphoric acid (Condac 37, FGM, Joinville, Santa Catarina, Brazil) for 15s on dentin, with rinsing carried out for 60s. Then, the drying process was conducted with absorbent papers to remove excess water, leaving a slightly moist surface to prevent the collagen fibers from collapsing. Subsequently, two-step total-etch ASB (3M/ESPE, St. Paul, Minnesota, USA) was applied for 30 s to allow the water and solvent to evaporate, a gentle air blast was conducted, and light-curing was performed for 20 s (Optilux 501; Demetron, Danbury, Connecticut, USA).
For the two-step self-etch adhesive system CLF (Kuraray Noritake, Okayama, Okayama, Japan), the self-etch primer was applied actively for 30s, followed by gentle air blasts. Following that, the adhesive was applied in even layers and light-cured for 20s (Optilux 501; Demetron, Danbury, Connecticut, USA). For the one-step self-etch adhesive system OPT (Kerr, Orange, California, USA), the system was applied actively for 15s. Then, it was dried with gentle air blasts, followed by a second layer of the system, also accompanied by gentle air blasts and finally light-cured for 20 s (Optilux 501; Demetron, Danbury, Connecticut, USA).
The composite resin (Filtek Z250, 3M, St. Paul, Minnesota, USA) was inserted in 2-mm increments and light-cured for 20 s (Optilux 501; Demetron, Danbury, Connecticut, USA). At the end of the last layer, the light-curing was applied for 60 s. In this manner, a 6 mm composite block was manufactured. The blocks were then stored in distilled water at 37 °C for 24 h [19]. The irradiance of approximately 600 mW/cm2 of the curing light Optilux 501 was measured with the use of a radiometer (Hilux Ledmax, Dentaurum J.P.KG, Pforzheim, Germany).
2.4. Sticks Acquisition
The blocks restored were individually fixed in acrylic support with sticky wax. This set was fixed to the precision cutting machine (Isomet 1000, Buehler Ltd., Lake Bluff, Illinois, USA), and with the aid of a diamond disc (Diamond Wafering Blades, Erios, Ipiranga, São Paulo, Brazil), serial cuts were performed in the mesiodistal and buccolingual directions, maintaining the spacing of 1 mm between the sections. The blocks were then removed from the acrylic support so that the sections constituted of resin composite attached to dentin shaped like a parallelepiped (sticks) could be selected. For each specimen, 6 to 8 sticks were obtained.
2.5. Aging Protocols
Half of specimens of each adhesive system were stored in DW at 37 °C for 24 h and then submitted to the microtensile BS test. The other half of specimens of each adhesive system were submitted to 180-day agin protocols using DW (n = 15), AS (n = 15), CA (n = 15), or TC (n = 15).
For the aging in DW, the medium was exchanged every two days for a period of 180 days [12]. The saliva was also substituted every two days for a period of 180 days [19]. For the aging by storage in CA the sticks were stored in a 0.3% citric acid solution with 2.3 pH for 60 min each day, simulating ten erosive challenges per day, until the exposure time corresponding to the 180-days period was completed. Considering that each erosive episode lasts 90 s and assuming they occur ten times during the day, then there would be 900 s of contact with the acid solution per day [20]. Therefore, to represent 180 days of exposure to the medium, 162,000 s would be needed, which amounts to 45 h, which was simulated by 1 h per day for 45 days.
For the aging protocol utilizing TC (Biopdi, São Carlos, São Paulo, Brazil), the sticks were submitted to 1,000 hydrothermal cycles in distilled water at 5 °C and 55 °C; each bath lasted for 30s, a protocol that simulated a period of 180 days [21].
2.6. Microtensile BS Test
The sticks were fixed with a cyanoacrylate-based adhesive to the grips of a device for microtensile testing that was connected to a universal testing machine (EZ Test; EZS, Shimadzu, Chiyoda-ku, Tokyo, Japan). The tractioning was conducted at 0.5 mm/min speed until the rupture of the stick [22]. The BS values were recorded in Newtons (N). Once the area of the dentin/adhesive/resin interface (mm2) had been measured with a digital caliper, the BS, in Megapascal (MPa), was obtained.
2.7. Failure Mode
A single operator by means of visual inspection under a stereoscopic magnifying glass (EK3ST, Eikonal Equip) assessed the failure mode at the interface (Ópticos e Analíticos, São Paulo, São Paulo, Brazil), with a 40x augmentation. The types of failures were classified as adhesive, cohesive in dentin, cohesive in composite resin, and mixed [13].
2.8. Statistical Analysis
All statistical analyses were conducted on the SPSS 23 program (SPSS Inc., Chicago, Illinois, USA), adopting the 5% significance level. After adherence to normality and homoscedasticity checks, to compare the BS provided by the different adhesive systems after 24 h, the BS values were assessed by one-way ANOVA. To investigate the effect of the adhesive systems and of the laboratory protocol that represents 180 days of aging, as well as its interaction, the BS data were submitted to a two-way ANOVA. The failure modes were descriptive under the relative frequencies form.
3. RESULTS
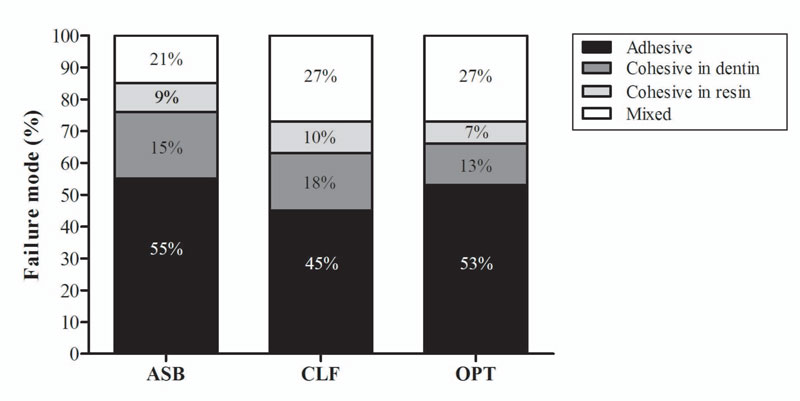
Table 1 presents the BS values of the different adhesive systems after 24 h of storage in DW. It was observed that the two-step total-etch ASB presented the higher bond strength (p < 0.05), while the two-step self-etch CLF and the one-step self-etch OPT did not demonstrate differences between them (p > 0.05). For all adhesive systems tested, the predominant failure mode was adhesive, followed by mixed, cohesive in dentin, and, lastly, cohesive in resin composite (Fig. 2).
The BS values of the different adhesive systems after 180-day aging protocols are presented in Table 2. It was verified that the BS obtained with the two-step total-etch ASB significantly overcame the BS observed with one-step self-etch OPT when stored in DW or AS (p < 0.001). In these storing mediums, the two-step self-etch ASB did not differ from the two-step total-etch CLF (p > 0.05), a result that was not maintained when the aging was simulated with TC and erosive challenges. In these situations, the CLF system presented BS values that were significantly lower than those observed for ASB (p < 0.001). The same situation was found for the one-step self-etch OPT in the CA challenge (p < 0.05). In TC aging, the BS presented by OPT did not differ from ASB (p > 0.05), both of which had higher values than CLF (p < 0.05).
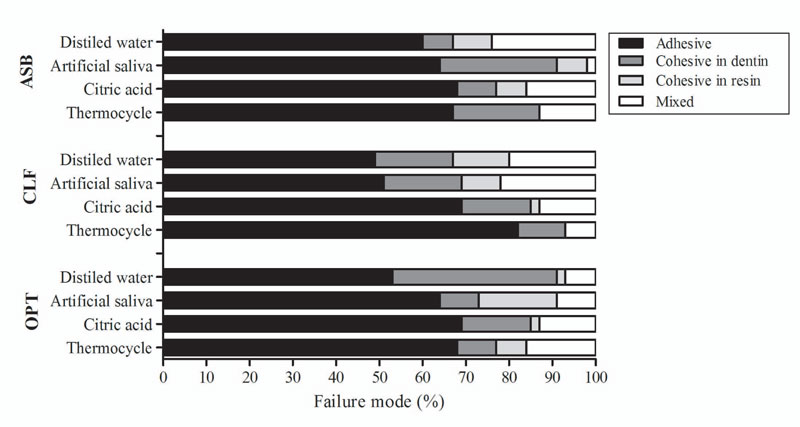
After aging, the adhesive failure continued to be the most prevalent for all the adhesive systems and aging protocols (Fig. 3). The least frequent type of failure encountered was cohesive in resin. It can also be noted that there was an alternation between mixed and cohesive in dentin fractures.
| Adhesive System | Bond Strength |
|---|---|
| Adper Single Bond 2 | 21.05 ± 14.47 (A) |
| Clearfil SE Bond | 14.92 ± 7.13 (B) |
| Optibond All-in-One | 12.84 ± 6.89 (B) |
| Aging Protocol | Adhesive System | ||
|---|---|---|---|
| Adper Single Bond 2 | Clearfil SE Bond | Optibond All-in-One | |
| Distilled Water | 18.45 ± 5.40 (Aa) | 14.98 ± 4.71 (ABa) | 12.21 ± 8.00 (Bb) |
| Artificial Saliva | 18.92 ± 7.24 (Aa) | 16.73 ± 7.35 (ABa) | 14.38 ± 6.71 (Bab) |
| Citric Acid | 13.75 ± 5.28 (Ab) | 7.09 ± 2.79 (Bb) | 7.10 ± 2.78 (Bc) |
| Thermal Cycle | 19.74 ± 7.73 (Aa) | 6.65 ± 1.69 (Bb) | 16.56 ± 4.32 (Aa) |
4. DISCUSSION
Considering the variety of adhesive systems commercially available and knowing that the comprehension of their performance is relevant to guide the choice among total-etch and self-etch systems, many in vitro studies have been conducted to compare the performance of these materials. One of the widely studied properties is the microtensile BS, which is measured in the majority of the experiments 24 h after preparing the restoration [18-21]. However, in the oral cavity, the tooth-restoration interface is subject to the occurrence of biodegradation processes over time, and it becomes necessary to investigate the behavior of various types of adhesive systems under conditions that challenge its integrity in order to simulate what occurs clinically. Thus, this study assessed whether different aging protocols have effects on the BS of total-etch and self-etch adhesive systems to dentin substrate, and their respective failure modes.
In the literature, there are no clear guidelines about shear force limits, but in fact adhesives should allow good bonding performance in order to sustain masticatory forces (5-10 MPa). On the other hand, adhesion forces should not be too strong in order to avoid enamel and dentin loss in case of injury (40-50 MPa). Therefore, the ideal biomaterial should have bonding forces included in the interval of 5-50 MPa, even if these limits are mostly theoretical [23].
After 24 h, the BS values obtained for the two-step total-etch adhesive system were greater when compared to those observed with the self-etch systems, which did not differ between each other. In fact, Isolan et al. [24] with the same assessment time (24 h), by comparing the BS between total-etch and self-etch adhesive systems on various substrates (enamel, dentin, composite resin, and porcelain), showed that the total-etch system presented greater BS values. This result may be attributed to the strong acids used in the total-etch adhesives to promote dentin demineralization, contributing to a deeper impregnation of the adhesive system in dentin, forming a thicker hybrid layer. Other than that, these adhesive systems create a superficial layer, that is also thicker and supports greater tensions, differently from the self-etch systems, whose layers are thinner. In the present study, the total-etch system used (i.e., ASB) contains water and ethanol as solvents, which have an important effect on the substrate bond quality because they promote an elevated wettability of the acid-prepared dentin [25].
By simulating the aging for 180 days, it could be observed that, for the majority of the experimental conditions, there was a decrease in the BS values with regard to the 24 h immersion time, suggesting that the storage in DW, AS, CA, and TC represent methods to promote dentin/adhesive/resin interface degradation. This finding corroborates with the study of Deng et al [5]. who, by researching the effect of four aging protocols on the dentin/adhesive/resin interface degradation, employing total-etch and self-etch systems, observed a decrease in BS of almost 50% and a significant increase in interface degradation for both systems studied.
This degradation observed over time for the total-etch system can be justified by the fact that the conditioned dentin layer may not be totally impregnated by the adhesive system. The solvents contained in the adhesives have the role of promoting the elimination of the water present between the collagenous fibers, promoting the infiltration of hydrophobic resinous monomers to form the hybrid layer. Nonetheless, there may not be sufficient substitution of all the water removed by the monomers, contributing, therefore, to the weakening of the adhesive system [26].
In this study, the two-step self-etch system did not present significant differences with regard to the total-etch system when stored in DW or AS. On the other hand, when there was TC or when the storage was in CA, the self-etch adhesive systems did not match the two-step total-etch system. A possible explanation for these findings can be the fact that the two-step total-etch adhesive systems form a more hydrophobic layer at the top of the dentin-bond interface, making it less susceptible to water sorption, other than promoting only a partial dissolution of hydroxyapatite, which is an important protective mineral against the collagen fiber degradation [27]. Furthermore, only the storage in DW and AS do not seem to promote very significant aggression on the bond interface, at least within the period of 180 days.
When the aging process was simulated by TC and by immersion in CA, it was observed that the two-step self-etch adhesive system provided BS values that were significantly lower than those observed with the total-etch adhesive system. However, by evaluating the BS obtained with total-etch and self-etch adhesive systems submitted to TC, it was found that the total-etch and two-step self-etch systems did not present BS differences after 24 h storage, but in the period of 180 days, one of the total-etch systems suffered a reduction in its BS, being that the greater values were obtained with the two-step self-etch adhesive system [28, 29]. This finding may have occurred due to the fact that the bond exhibited more resistance toward the temperature variation cycle, generating fewer gaps in the interface for the entrance and exit of fluids. Differently, in the present study, the total-etch adhesive system may have exhibited more resistance toward the temperature variation during TC, possibly because of the formation of a thicker hybrid layer and of a superficial layer of the bond that resisted the tensions generated through the aging method [16].
TC seems to execute a greater impact on the bond interface because it promotes temperature alterations, as well as due to the differences in the coefficients of thermal expansion between the adhesive and dentin, enabling gap formation at the interface, which would entail a greater diffusion of water, leading to the plastification of the bonding agent [21]. All of these adhesive systems utilized a hydrophilic monomer (HEMA-2-hydroxyethyl methacrylate) that absorbs water during TC; in addition, a relative quantity of water remains trapped in the interface, causing soaking and plastification of the polymers, which results in a reduction of the mechanical properties of the adhesive system [16].
The storage in CA produces an erosive effect on the bond interface, causing a gradual dissolution of the bond interface from the edges to the center. There may also be degradation of the collagenous fibers that were not impregnated by the adhesive system due to the incomplete penetration in demineralized dentin, causing instability to the hybrid layer over time [30]. In this study, it was observed that for the two-step self-etch adhesive system, TC and the CA solution resulted in an equivalent reduction to the bond strength, an aspect that was not observed when the one-step self-etch adhesive system was used because the CA solution was the one that caused the lowest BS values for the samples in which this adhesive system was applied. In this regard, it is believed that the erosive challenge represents a protocol that harshly defies the bond interface.
The present report evaluated failure type (adhesive/cohesive/mixed) as the evaluation of this variable is widely used in dental science to evaluate adhesive behavior [31]. It was observed that for all the adhesive systems tested, the most predominant failure mode was adhesive. These results can be justified by the microtensile BS test utilized in the research, which is more efficient in reduced test areas (< 2.0 mm2), generally showing the adhesive failure mode as being the most prevalent [32].
The findings from this research indicate DW as a viable storage medium because the BS values obtained with it did not differ from those associated with the use of AS. Additionally, when utilizing DW, lower cost and easy access are benefits. Although TC is a method in which there is an association of hydrolytic actions and temperature, at least for the adhesive systems evaluated and in the conditions in which this study was conducted, the BS was not inferior to what was reached in DW and AS. However, the fact that TC accelerates the aging process, which occurs only after the 180-day wait, can be established as an advantage. By aging the interface with TC, nonetheless, it is necessary to employ equipment, an aspect that is not demanded when erosive challenges are conducted, which do not require equipment and exhibit proportionate, depending on the adhesive system, damages equal to or even superior to the ones caused by TC.
Considering the limitations of this study, previous authors pointed out that the presence of interfacial porosity could influence strength values [33]. Thus, further studies are necessary to evaluate this variable.
Different uppercase letters indicate statistically significant differences between adhesive systems in the same aging protocol. Different lowercase letters indicate statistically significant differences between aging protocols in the same adhesive system (two-way ANOVA followed by Tukey’s test, p < 0.05).
CONCLUSION
It was concluded that for the two-step total-etch and the two-step self-etch adhesive systems, the storage in AS and TC resulted in effects that matched the effects of DW. The greatest impact on the BS occurred in the CA solution, a situation in which the self-etching adhesive systems revealed inferior bonding performance when compared to the total-etch system.
CLINICAL SIGNIFICANCE
It is important to submit the dentin/adhesive/resin interface to degradation processes so that there is greater proximity to the clinical reality. Therefore, this study used aging protocols simulating clinical reality and elucidated its influence on the bond strength of commonly used adhesive systems to dentin substrate.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
The data that support the findings of this study are with the corresponding author and can be made available upon reasonable request.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


