All published articles of this journal are available on ScienceDirect.
Preliminary Clinical Evaluation of Short Fiber-Reinforced Composite Resin in Posterior Teeth: 12-Months Report
Abstract
This preliminary clinical trial evaluated 12 month clinical performance of novel filling composite resin system which combines short fiber-reinforced composite resin and conventional particulate filler composite resin in high stress bearing applications. A total of 37 class I and II restorations (compound and complex type) were placed in 6 premolars and 31 molars. The restorations were reviewed clinically at 6 months (baseline) and 12 months using modified USPHS codes change criteria for marginal adaptation, post-operative sensitivity, pulpal pain and secondary caries criteria. Photographs and x-rays were obtained for restorative analysis. Results of 12 months evaluation showed 5 restorations having little marginal leakage (B score) and 1 patient had minor pulpal symptom and post-operative sensitivity (B score). No secondary caries or bulk fracture was detected. The majority of restorations exhibited A scores of the evaluated criteria. After 12 months, restorations combining base of short fiber reinforced composite resin as substructure and surface layer of hybrid composite resin displayed promising performance in high load bearing areas.
INTRODUCTION
Dental restorative filling composite resins have been introduced to dental community in 1960´s [1]. Since then after many significant material improvements restorative composite still suffers lack of mechanical properties and problems related to polymerization shrinkage. Clinical studies have shown that direct fillings fail predominantly because of occlusal wear or secondary caries [2-5]. However, fracture of restorative composite is reported also as a common reason for replacement [3,5]. Due the failures of this kind, it is still controversial, whether restorative composites should be used in large high-stress bearing applications such as in direct posterior restorations [4,5]. The relatively high brittleness and low fracture toughness of current composites still hinder their use in these large stress-bearing restorations [6-8].
Studies have been undertaken to evaluate and improve restorative composite resin against wear and lower the polymerization shrinkage. Attempts have been made to change type of filler or filler size and their silanization, by changing the polymerization kinetics of resins and to influence to degreeof monomer conversion [9-12]. Reinforcing the resin with glass fibers [13,14], with fiber-reinforced composite (FRC) substructure [15,16], whiskers [17], particulate ceramic fillers (dense and porous) [18] and optimization of filler content [9] are among the methods that have been studied. Some other aspect relating to indirect laboratory made composites have been investigated by using post-curing to enhance composite strength and toughness [19].
Recently, short fiber reinforced composite was introduced as a dental restorative composite resin [20-23]. The composite resin is intended to be used in high stress bearing areas especially in molars. The results of the laboratory mechanical tests revealed substantial improvements in the load bearing capacity, the flexural strength and fracture toughness of dental composite resin reinforced with short E-glass fiber fillers in comparison with conventional particulate filler restorative composite resin [20-23]. The short fiber composite resin has also revealed control of the polymerization shrinkage stress by fiber orientation and, thus, marginal microleakage was reduced compared with conventional particulate filler restorative composite resins [22].
Based on the published and our unpublished results of the physical properties of short fiber reinforced composite, it is suggested that short fiber composite resin could be used to fulfill the requirements for the ideal posterior restorations. The short fiber composite is intended to be used as bulk substructure material which will be covered by a layer of particulate filler composite. It is difficult to predict clinical long-term performance from only laboratory experiments. Thus, the aim was to conduct a pilot clinical trial investigating the performance of materials combination of bulk short fiber reinforced composite substructure and surface particulate filler composite in high stress bearing applications.
MATERIALS AND METHODS
Patients’ Selection and Restorative Procedure
The methods used in this investigation have been widely reported [24,25] and was approved by the Joint Commission on Ethics of the Turku University and the Turku University Hospital (20.6.2006). For this study, the case reports of 35 adult patients were selected according to pre-determined inclusion criteria among the registers of private practice dental offices in Finland from January 2009 to May 2011. All teeth were in occlusion and had at least one proximal contact with an adjacent tooth. Patients with extremely poor oral hygiene, heavy bruxism habits or periodontal problems were excluded.
Restorative procedures were carried out by many dentists. Before the start of the study, the operative procedure was thoroughly discussed with the dentists. 31 (84%) of restorations were placed in molars and 6 (16%) in premolar. The majority of the restorations were of a complex type with more than 2 surfaces included. Reason for restorations in 31% of patients was the presence of caries, in 29% of patients the replacement of old restorations and 40% of patients restorations after endodontic treatments (Table 1). Concerning the method of isolation, the use of rubber dam or simply cotton rolls and aspiration, was determined according to a predetermine scheme of randomization.
Characteristics of Patients and Restorations
| 12 Months | |
|---|---|
|
|
|
| Mean age± SD | 42 ±15 |
|
|
|
| Females | 14 |
|
|
|
| Males | 21 |
|
|
|
| Restorations | 37 |
|
|
|
| Premolars | 6 |
|
|
|
| Molars | 31 |
|
|
|
| Mean number of surface per restoration | 2.9 ±1.2 |
| New restorations | 10 |
| Replacement of old restorations | 27 |
Three different adhesive systems were used randomly. Single-step self etch primer and bond (Vivapen, IvoclarVivadent, Schaan, Liechtenstein) and two-steps self etch primer and bond (Clearfil SE bond, Kuraray, Tokyo, Japan) and three-steps etching, primer and bond (Scotchbond multi-purpose adhesive, 3M ESPE, USA). Bonding agents were placed according to manufacturer's instructions. Flow composite resin was applied on the bottom of 84% of cavities prior placing the short fiber reinforced composite (Xenious, StickTeck Ltd, Turku, Finland). The short fiber composite resin was placed and light-cured according to an incremental technique. All restorations were fully covered with a one layer (1-2 mm) of hybrid composite resins [(Estelite, Tokuyama, Japan), (Clearfil Majesty Posterior,Kuraray, Japan), (Z250 and Z100 3MESPE, USA), (Synergy, Coltène/Whaledent, Altstätten, Switzerland)] then occlusion was carefully adjusted with articulating paper. Finishing and polishing procedures were carried at same visit after occlusal adjustment.
Evaluation
The restorations were evaluated after 6 months (baseline) and 12 months by same operator. Each restoration was evaluated according to slightly modified USPHS criteria for the following characteristics: marginal adaptation, post-operative sensitivity, pulpal pain and secondary caries [24, 25] (Table 2). Photograph and X-ray records of restorations were used (Fig. 1-5).
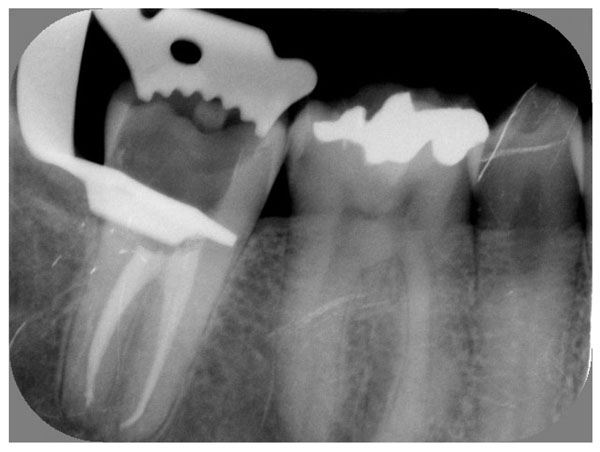
Lower right second molar has been root canal treated. Gutta percha up to 3mm is removed from the canal orifices.

Placement of bulk short fiber composite according to an incremental technique
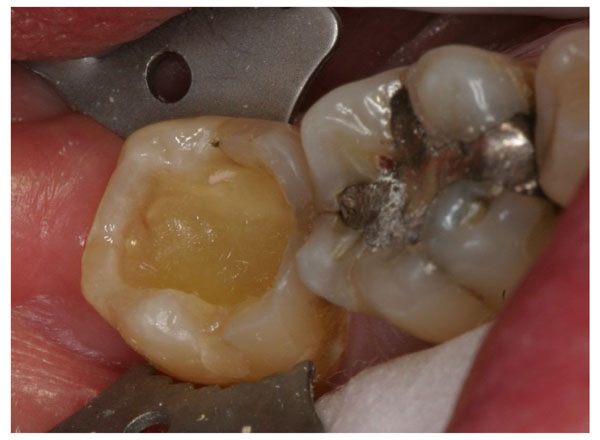
Dentin and enamel surfaces are bonded and bulk short fiber composite substructure applied and light cured in three layers.
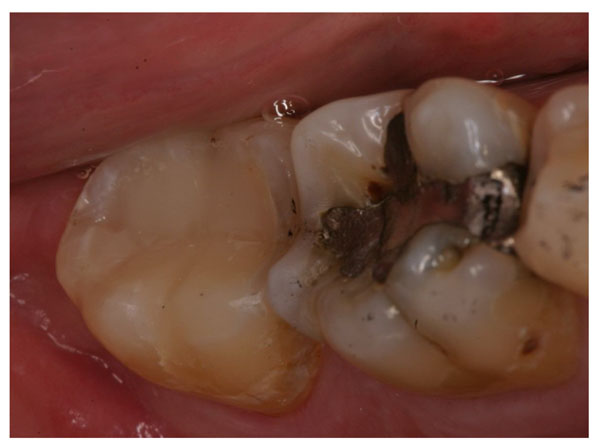
The cavity is filled with restorative composites and the restoration is finished and adjusted in occlusion.
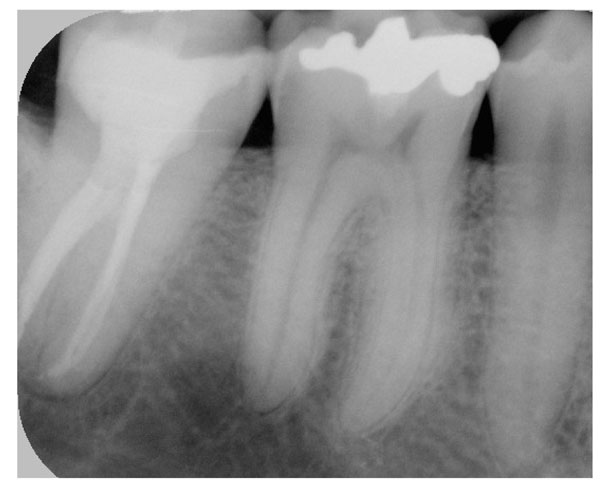
An X-ray showing the finished restoration with materials combination of bulk short fiber composite substructure and surface layer of particulate filler composite.
Modified USPHS Criteria Used
| Criteria | Code | Definition |
|---|---|---|
|
|
||
| marginal adaptation | A | Restoration closely adapted to the tooth, No explorer catch at margins, or there was a catch in one direction |
| B | Explorer catch. No visible evidence of a crevice into which explorer could penetrate. No dentin or base visible | |
| C | Explorer penetrates into a crevice that is of a depth that expose dentin or base | |
|
|
||
| post operative sensitivity | A | None |
| B | Mild but bearable | |
| C | Uncomfortable, but no replacement is necessary | |
| D | Painful. Replacement of restoration is necessary | |
|
|
||
| pulpal symptoms | A | No symptoms |
| B | Minor symptoms | |
| C | Major symptoms | |
| D | Extensive symptoms | |
|
|
||
| secondary caries | A | Absent |
| B | Present | |
RESULTS AND DISCUSSION
Results of 12 months evaluation showed 5 restorations having little marginal leakage (B score) and 1 patient had minor pulpal symptom and post-operative sensitivity (B score). No secondary caries or bulk fracture have been detected. The majority of restorations exhibited A scores of the evaluated criteria.
These results of short-term pilot clinical reports were according to the expectations, since several in vitro studies have already shown a satisfactory performance of using same materials combination in different high stress bearing applications [20-23,26-28].
The function of bulk short fiber composite substructure is based on supporting the surface particulate filler composite layer and working as crack stopper layer. Reinforcing effect of the fiber fillers is based on stress transfer from polymer matrix to fibers but also behavior of individual fiber as a crack stopper. Random fiber orientation had a significant role in mechanical properties. Clinical study reported by Van Dijken have shown that restorative composite with microfibers suffer extensive wear [29], which can be partly explained because of the used fiber length was well below of critical fiber length. In order a fiber to act as an effective reinforcement for polymers, stress transfer from the polymer matrix to the fibers is essential [30,31]. This is achieved, if the fibers have a length equal or greater than the critical fiber length [30]. It has been measured using fiber fragmentation test that the critical fiber lengths of E-glass with bis-GMA polymer matrix vary between 0.5 and 1.6 mm [32]. Deteriorated or initially poor adhesion between the fibers and polymer matrix increase the critical fiber length. In this case, the mechanical friction of fibers to polymer matrix at the interface can compensate the poor adhesion [33]. Based on this, the short fiber composite resins used in this study have fiber fillers equal or greater to critical fiber length.
To receive support from the short fiber composite substructure for the surface particulate composite, the structural rigidity of the short fiber composite substructure should be higher than that of surface particulate composite resin.
In this, the fiber orientation likely has a significant role. On the other hand, if the function of the short fiber composite substructure is based on the mechanism of a crack stopper, the distance from the surface of the stress initiation point to the fibers is of importance. Therefore, the volume fraction or thickness of short fiber composite could contribute to the crack propagation and load-bearing capacity. Previous study by authors, showed when short random fiber-reinforced composite (FRC) was used as substructure for particulate filler composite, the load-bearing capacity of the materials combination increased linearly as thickness layer of FRC increased [16]. From this point of view, in this clinical report, short fiber composite-substructure was covered with only one layer of hybrid particulate filler composite in order to prevent fiber exposure. Although, bacterial adhesion (Streptococcus mutans) did not demonstrate difference to short fiber composite resin than to other restorative materials [34].
Stress applied to the teeth and restorations is generally repetitive or cyclic rather than being isolated and impact in nature. Regarding to this, materials combination of short fiber composite and particulate filler composite showed higher fatigue limit than that obtained with plain particulate filler composite [15].
Most of dentists participated in this multi-centered clinical trial used flowable composite as liner on cavity floors. Despite the popularity of the use of flowable composite on the bottom of cavity, there is only few clinical studies have investigated the effectiveness of this technique and compared with traditional direct placement of composite resin and these studies reported no significant differences between the techniques [35,36].
Finally, it is necessary to emphasize that the time frame and cases for this clinical trial were not of such duration and number to indicate the long-term suitability of the tested materials combination, but it may provide an indication regarding their future performance in high stress bearing applications.
CONCLUSIONS
Within limitations of this pilot clinical report, the results showed good clinical performance of a novel materials combination of bulk short fiber composite substructure and surface layer of particulate filler composite in high stress bearing areas after 1 year.
CONFLICT OF INTEREST
None declared.
ACKNOWLEDGEMENT
None declared


