All published articles of this journal are available on ScienceDirect.
Medical Ethics Knowledge and Attitude Among Dental Students from Two Universities in The Middle East
Abstract
Background:
Dentists are obligated to provide patients with ethical and harmless treatment.
Objective:
This study aimed to assess the knowledge, attitude and practices of medical ethics among dental students in two dental faculties in the Middle East.
Methods:
A cross-sectional study using a validated online self-administrated questionnaire was completed by dental students who started clinical training at Mansoura University, Egypt, and from Umm Al-Qura University (UQU), Saudi Arabia. Descriptive statistics and chi-square tests were used for the statistical analysis.
Results:
Participants were 649 dental students. About 77% of Mansoura’s students were aware of the Hippocratic Oath compared to 89.6% of UQU students (p=0.000). No significant difference was found between the two faculties in the presence of ethical topics in their curriculum and the mode of teaching. About 67% of respondents reported obtaining written consent from UQU patients compared to only 10.5% of Mansoura’s patients. Nearly 86.3% and 63.3% of dental students at Mansoura and UQU, respectively, believed that they knew the best, irrespective of the patients’ opinion. In case of any wrongdoing during treatment, 88.7% of Mansoura’s and 93.9% of UQU students agreed to inform the patients. Regarding patient autonomy, only 51.2% and 65.3% of dental students at Mansoura and UQU, respectively, respected the patient’s wishes during treatment., The majority of students from both faculties had less knowledge regarding services and duties related to the ethical committee.
Conclusion:
Gaps in knowledge, attitude and practices of medical ethics were found among dental students of the two faculties, especially among Mansoura’s students. Attention should be paid to improving the present situation.
1. INTRODUCTION
Ethics can be defined as the values that include honorable behavior and judgment in the way of stating and appraising principles by which issues of deeds can be solved [1]. It is also known as the science of human personality and behavior; commitments must be maintained based on what is morally correct and immoral, and respectable interpersonal relations should be sustained [2]. Attention should be given equally to ethical and bioethical knowledge and attitude, where ethics relate to assessing personal behavior, while bioethics is more related to the sense of public health responsibilities and decision-making parameters [2].
Dentists and dental students are obligated to provide patients with legal treatment without commencing any medical errors to ensure that dentists’ knowledge and training in bioethics regarding patients' “rights and needs” are mandatory in many institutions. Research about ethics can help dentists be armed with the required knowledge to resolve any ethical dilemma. It is essential to follow formal guidelines and codes of ethics, which can be applied while treating patients. Such guidelines help workers in the dental profession in determining high standards of moral obligations when practicing clinical dentistry as well as conducting scientific research [3].
A study surveyed physicians in Saudi Arabia reported that the majority (77.5%) requested a clear guideline to support their judgment while deciding on a patient-related ethical matter [4]. A retrospective study regarding patients' complaints related to dental treatment indicated that more than 50% of the patients thought that their opinion was considered not important to the dentist, and eventually, the operator decided the course of treatment for them [5]. Another study examined dental lawsuit's causes and found that of the 32 dental complaints filed in one year, 20 cases had clinical issues, and 12 were nonclinical. Only one case had signed informed consent [6].
An increasing number of reported ethical issues related to the treatment and behavior of medical and dental personnel have been recorded in recent years [7]. Dental students are the future dentists; they need to be accountable for their patients' well-being. The curriculum is prepared to increase awareness of ethics and professionalism among dental students. However, it is crucial to identify the perception of ethics, attitude, and behavior among these students before graduation and practicing. Our study will shed light on the current status of future dentists if they are ethically prepared to start their profession based on the need for modifications in dental curriculums.
2. MATERIALS AND METHODS
2.1. Study Design and Study Population
This cross-sectional study was designed to evaluate and compare the attitude of dental students from two different universities in the Middle East. Students were recruited from the Dental Faculties of Mansoura University, Egypt and Umm Al-Qura University (UQU), Saudi Arabia. Students who started clinical training were selected using a convenience sampling technique from the last three academic years. A total of 649 students participated (600 students from Mansoura University, Faculty of Dentistry) and (49 from UQU, Faculty of Dentistry). Of the total sample, 46.7% were males, and 53.3% were females. Regarding the sample size and the response rate, the total number of students attending the clinics was 1639, with a confidence interval of 95%, marginal error of 5%, and population proportion of 50%. The calculated sample size was 323 participants and more. Ethical approval was obtained from the Institutional Review Board of Mansoura University, Faculty of Dentistry (#A03051020).
2.2. Data Collection
Data was collected using an online self-administered questionnaire containing 28 close-ended questions, divided into three parts. Part one included questions covering students’ knowledge about ethical principles, codes of ethics training, ethical courses and patient’s rights. Part two was about students’ attitudes regarding the source of ethical knowledge and consultation in case ethical problems occurred. The students were asked whether they were aware of the presence of an ethics committee in their institution and about the role of this committee. The last part of the questionnaire was about the everyday ethical issues that students might face. They were asked if they agreed or disagreed with certain statements concerning ethical conduct, autonomy, confidentiality, informing patients about wrongdoing, informed consent, and the influence of religious beliefs on the treatment.
2.3. Data Validity
The questionnaire was obtained from a previous study [3]. The questionnaire was piloted first on 30 students (15 students from each dental school), and then the questionnaire was modified according to the students’ feedback. The validity of the questionnaire was tested twice on the same students at the one-week interval; the kappa test was 95%.
2.4. Statistical Analysis
Descriptive statistical analysis was used to calculate frequencies and percentages. Categorical data were studied using Chi-square. Statistical analysis was performed using the Statistical Package for the Social Sciences (Version 20, SPSS Inc., Chicago, IL, USA). A value of P <0.05 was considered statistically significant
3. RESULTS
This cross-sectional study compared dental students who started clinical training (3rd, 4th, and 5th-year students) at the Faculty of Dentistry, Mansoura University and (4th, 5th, and 6th-year students) at the Faculty of Dentistry UQU. Of the 1470 dental students at Mansoura University attending the clinics, only 600 completed the survey (40.8%). On the other hand, 49 dental students out of 169 (29%) participated from UQU. The demographic characteristics of the participants from both faculties are displayed in Table 1.
| - | Mansoura University | Umm Al-Qura University (UQU) |
|---|---|---|
| N (%) | N (%) | |
| Gender | ||
| Females | 432 (57%) | 28 (57.1%) |
| Males | 168 (43%) | 21(42.9%) |
| Academic Year | ||
| 1st clinical year | 237 (39.5%) | 17 (34.7%) |
| 2nd clinical year | 211(35.2%) | 17 (34.7%) |
| Final year | 152(25.3%) | 15 (30.6%) |
| Total Number | ||
| 600 (92.5%) | 49 (7.5%) | |
Students’ knowledge of the basic concepts of ethics is reported in Table 2. Knowledge about the Hippocratic Oath and Helsinki Declaration was reported by more than 75% of the participants. However, a statistically significant difference was found between the two faculties (p=0.004). Most dental students from Mansoura University and UQU agreed that ethics topics were represented in their curriculum, with no significant difference (p = 0.09). About 81% of dental students at Mansoura University believed ethical knowledge was essential in their work compared to 71.4% of UQU dental students (p = 0.01). Nearly 45.7% and 63.3% of dental students in Mansoura University and UQU came across ethical issues daily, while 54.3% and 36.7% faced such issues weekly (p = 0.001). A significant difference (p=0.001) was found regarding patients enquiring about their treatment, where 91.5% of Mansoura dental students answered questions related to their patient’s diagnosis compared to 73.5% of UQU students. Dental students at Mansoura University discussed their daily work with their colleagues more than UQU students (p = 0.001). Lectures, the internet, and self-learning were the most common sources of ethical information in both Universities. Only 2.8% of dental students at Mansoura University attended training courses in bioethics, compared to 20.4% from UQU. Most dental students at UQU obtained signed informed consent from their patients, while 10.5% only were obtained from Mansoura’s dental patients. A significant difference (p = 0.001) was found between the students in the two faculties regarding the knowledge about services provided by the ethics committee in their university.
| - |
Mansoura University (600) |
Umm Al-Qura University (49) |
X2 (p-value) |
|---|---|---|---|
| N (%) | N (%) | ||
| Do you Know Hippocratic Oath? | |||
| Yes | 462 (77%) | 44 (89.6%) | 14.361 (0.04) |
| No | 138 (23%) | 5 (10.2%) | |
| Do you Helsinki Declaration? | |||
| Yes | 243 (40.5%) | 38 (77.6%) | 36.219 (0.001) |
| No | 357 (59.5%) | 11 (22.4%) | |
| Do you think ethics is represented in your curriculum? | |||
| Yes | 495 (82.5%) | 41 (83.7%) | 3.241 (0.09) |
| No | 105 (17.5%) | 8 (16.3%) | |
| How important is knowledge of ethics to you in your work? | |||
| Very | 486 (81%) | 35 (71.4%) | 14.521 (0.01) |
| Moderate | 69 (11.5%) | 10 (20.4%) | |
| Little | 45 (7.5%) | 4 (8.2%) | |
| Do you respond to patients’ questions about their cases during their visits? | |||
| Yes | 513 (85.5%) | 42 (85.7%) | 1.732 (0.218) |
| No | 87 (14.5%) | 7 (14.3%) | |
| How often do you come across any ethical issues? | |||
| Daily | 274 (45.7%) | 31 (63.3%) | 32.471 (0.001) |
| Weekly | 326 (54.3%) | 18 (36.7%) | |
| How often do patients ask you about their diagnosis? | |||
| Always | 549 (91.5%) | 36 (73.5%) | 19.542 (0.01) |
| Never | 51 (8.5%) | 13 (26.5%) | |
| How often do you discuss your daily cases with your colleagues? | |||
| Always | 399 (66.5%) | 26 (53.1%) | 22.823 (0.001) |
| Never | 201 (33.5%) | 23 (49.9%) | |
| How did you acquire your knowledge of bioethics? | |||
| Lecture | 384 (64%) | 31 (63.3%) | 4.312 (0.09) |
| Internet | 105 (17.5%) | 12 (24.5%) | |
| Self-learning | 111 (18.5%) | 6 (12.2%) | |
| Have you attended training in bioethics? | |||
| Yes | 17 (2.8%) | 10 (20.4%) | 75.452 (0.001) |
| No | 583 (97.2%) | 39 (79.6%) | |
| Have you taken informed consent? | |||
| Signed | 63 (10.5%) | 33 (67.4%) | 214.23 (0.001) |
| Verbal | 311 (51.8%) | 11 (22.4%) | |
| No | 226 (37.7%) | 4 (8.2%) | |
| Is there an ethics committee in your institution? | |||
| Yes | 10 (1.7%) | 33 (67.3%) | 335.13 (0.001) |
| No | 590 (98.3%) | 16 (32.7%) | |
Dental students’ attitude toward ethical principles and their applications is summarized in Table 3. A high percentage of students (86.3% and 63.3%) at Mansoura and UQU, respectively, believed that they knew the best, irrespective of the patients’ opinion (p=0.001). Most participants agreed to inform the patients of any wrongdoing during the patient treatment. Regarding patient autonomy, only 51.2% and 65.3% of Mansoura and UQU dental students, respectively, respected the patient’s wishes during the treatment, even though the majority agreed that respecting the patient’s choices is mandatory. Most dental students disagreed with breaching the patient’s confidentiality. Students believed that ethics guidelines are helpful tools in their professional life and agreed that teaching ethics is important.
Table 4 represents the responses of dental students to questions related to the ethical committee role. Most students agreed that the committee's role is to give advice, encounter ethical problems, and ensure ethical standards are applied. However, regarding the ethical committee's role in approving and guiding the research, only 36.2% of students at Mansoura University knew about it compared with 89.8% of students at UQU (p=0.001). Many students did not know about the ethical committees' role in settling conflicts between professionals or between professionals and patients’ relatives. Most students also did not know about the teaching role or the contributions to the committee's scientific conference. Overall, knowledge about ethics was found to be better among Saudi students than Egyptian students.
Table 3.
| - | Mansoura University | Umm Al-Qura University (UQU) |
X2 (p-value) |
|---|---|---|---|
| N (%) | N (%) | ||
| Dentists know the best irrespective of patients’ opinion | |||
| Agree | 518 (86.3%) | 31 (63.3%) | 33.523 (0.001) |
| Disagree | 82 (13.7%) | 18 (36.7%) | |
| The patient should always be informed of wrongdoing | |||
| Agree | 532 (88.7%) | 46 (93.9%) | 17.341 (0.01) |
| Disagree | 68 (11.3%) | 3 (6.1%) | |
| Patients’ wishes should always be adhered to | |||
| Agree | 307 (51.2%) | 32 (65.3%) | 9.324 (0.05) |
| Disagree | 293 (48.8%) | 17 (34.7%) | |
| Confidentiality cannot be maintained in modern care and should be abandoned | |||
| Agree | 217 (36.2%) | 6 (12.2%) | 23.597 (0.001) |
| Disagree | 383 (63.8%) | 43 (87.8%) | |
| Ethical conducts are important only for avoiding legal action. | |||
| Agree | 328 (54.7%) | 20 (40.8%) | 19.265 (0.01) |
| Disagree | 272 (45.3%) | 29 (59.2%) | |
| Ethics is helpful during professional life. | |||
| Agree | 600 (100%) | 49 (100%) | ---- |
| Disagree | -- | -- | |
| Teaching ethics is important. | |||
| Agree | 568 (94.7%) | 45 (91.8%) | 7.783 (0.07) |
| Disagree | 32 (5.3%) | 4 (8.2%) | |
| Respecting patient choice in treatment is mandatory except for an emergency. | |||
| Agree | 518 (86.3%) | 43 (87.8%) | 5.915 (0.09) |
| Disagree | 82 (13.7%) | 6 (12.2%) | |
| Patients with infectious diseases or difficult cases should be treated. | |||
| Agree | 522 (87%) | 40 (81.6%) | 10.438 (0.05) |
| Disagree | 78 (13%) | 9 (18.4%) | |
Table 4.
| - | Mansoura University | Umm Al-Qura University (UQU) |
X2 (p-value) |
|---|---|---|---|
| N (%) | N (%) | ||
| What do you think an ethical committee’s role is? | |||
| To ensure standard ethical practices among healthcare personnel | |||
| Yes | 404 (67.3%) | 37 (75.5%) | 13.475 (0.04) |
| No | 196 (32.7%) | 12 (24.5%) | |
| Not sure | - | - | |
| To advise healthcare personnel when they encounter ethical/legal problems | |||
| Yes | 310 (51.7%) | 28 (57.2%) | 5.537 (0.09) |
| No | 192 (32%) | 12 (24.5%) | |
| Not sure | 98 (16.3%) | 9 (18.3%) | |
| To approve and guide research | |||
| Yes | 217 (36.2%) | 44 (89.8%) | 43.264 (0.001) |
| No | 191 (31.8%) | 3 (6.1%) | |
| Not sure | 192 (32%) | 2 (4.1%) | |
| To settle conflicts between professionals | |||
| Yes | 135 (22.5%) | 12 (24.5%) | 3.272 (0.145) |
| No | 218 (36.3%) | 26 (53.1%) | |
| Not sure | 247 (41.2%) | 11 (22.5%) | |
| To settle conflicts between professionals and patients’ relatives | |||
| Yes | 219 (36.5%) | 7 (14.2%) | 86.435 (0.001) |
| No | 128 (21.3%) | 39 (79.7%) | |
| Not sure | 253 (42.2%) | 3 (6.1%) | |
| To teach bioethics to students | |||
| Yes | 142 (23.7%) | 2 (4.1%) | 73.623 (0.001) |
| No | 341 (56.8%) | 41 (83.7%) | |
| Not sure | 117 (19.5%) | 6 (12.2%) | |
| To conduct bioethics conferences | |||
| Yes | 186 (31%) | 13 (26.5%) | 34.218 (0.001) |
| No | 295 (49.2%) | 32 (65.3%) | |
| Not sure | 119 (19.8%) | 4 (8.2%) | |
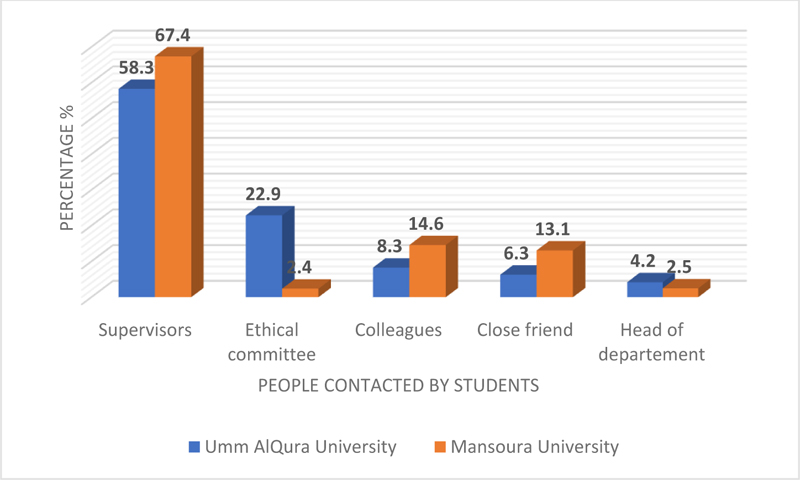
Fig. (1) shows the difference between students’ responses to the question related to their behavior when facing an ethical problem. Many students (58.3%) and (67.4%) at UQU and Mansoura University will approach their supervisor if they face an issue. The ethical committee was approached by 22.9% of students from UQU compared to 2.4% at Mansoura University. Approaching colleagues or close friends (14.6% and 13.1%) among dental students at Mansours University compared with (8.3% and 6.3%) of counterparts at UQU.
4. DISCUSSION
Students have been taught medical and dental ethics in Saudi and Egyptian Universities, yet they still face ethical dilemmas that they’re not confident enough to handle properly. Therefore, incorporating dental ethics training with dental education and testing students’ knowledge is crucial.
This study reported a lack of proper consent recording among Saudi and Egyptian students regardless of the student’s efforts. Informed consent in dentistry is not well documented, which can lead to legal action [8].
More than 80% of the present sample agreed to treat patients with infectious diseases, which is considered ethical. This finding agrees with other studies where dental staff have been found to have positive behavior regarding patients with HIV and hepatitis [9, 10]. Furthermore, they were thoughtful and profound for patients with mental health illnesses [11]. Dentists and dental students must treat all patients in the community without discrimination [12].
A similar attitude was reported regarding gaining ethical approval before starting a research project. Among this study sample, Mansoura University students (36%) did not understand the role of the ethics research committee regarding research and obtaining ethics approval before starting a project, unlike UQU students who were found more knowledgeable about it (89%).
It is reported that more than 20% of investigators in the Middle East did not attain ethical approval for their research plans submitted for funding [13, 14]. Moreover, several of these applications had no plans to gain informed consent [15]. The students in the present study showed very limited understanding of the role of the ethics clinical committees in other areas, such as settling any conflicts between health care workers themselves or with patients, in addition to the role of the research ethics committee in student continuing education and conference planning. The light should be shed more on the topics allied to ethics and professionalism in the dental field, which can be social, environmental, practical, honesty, plagiarism, and moral misconduct [16-18]. Therefore, focusing more on helping future and current dentists become ethically and morally professional necessitates improving the existing knowledge and skills. This may be achieved by increasing the number of courses and mandating ethical training alongside the clinical requirement. Dental students should understand the legal consequences of their ethical choices in all aspects of research, behavior and attitude towards patients and colleagues through a proper assessment before practicing any clinical practice.
The participants in this study have revealed a decent exercise in notifying and consulting their supervisor regarding their ethical problems (more than 50%). Parallel findings were stated by a study in Barbados and Saudi Arabia. 40% of the students informed their supervisor about their ethical dilemmas [3, 19]. On the other hand, in India, it was reported that medical doctors attempted to manage difficulties independently instead of consulting their supervisors or the ethics committee [20].
This study found that UQU dental students have an acceptable ethical knowledge compared to Mansoura’s. This could be explained because Mansoura’s students studied the topic of medical ethics in only a few lectures incorporated with the subject of Dental Public Health. On the other hand, UQU students have a whole course of ethics and dental and medical ethics subjects in their curriculum. This difference confirms that universities must work on their programs and ensure that a full ethical course should be given to their dental students before they start practicing on patients.
There is a gap in knowledge among students from UQU and Mansoura, which requires additional attention, as mentioned in other studies where a third of their medical residents had poor ethical understanding [3]. Therefore, preparing upcoming dentists to become ethically skilled is critical to avoid medico-legal matters. This can be achieved via undergraduate curriculums and post-graduate continuing education seminars. The results from this study can be used as a baseline to estimate the present knowledge to allow proper future training programs.
Data from this study is useful, yet it cannot be generalizable. This limitation can be improved in future studies by including a larger sample from different universities in the Middle East and not relying only on self-reported data. This study is one of few in the region that focuses on ethics, knowledge, and attitudes, and even with its methodological limitations, it offers valued evidence that can be used to construct additional knowledge.
CONCLUSION
The findings of this study raise some fundamental issues in ethical practice in some Middle Eastern dental schools. The findings show that even with the available ethics courses, there is a gap in knowledge, attitude, and practices of medical ethics among dental students of the two faculties, especially among Mansoura’s students. Attention should be paid to establishing continuous educational courses and assessment systems to ensure that dentists are equipped to resolve any ethical dilemmas before and after graduation.
LIST OF ABBREVIATION
UQU = Umm Al-Qura University
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study received approval from the Institutional Review Board of Mansoura University, Faculty of Dentistry (A03051020).
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All human research procedures followed were per the ethical standards of the committee responsible for human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
All participants signed the consent before participating in the study.
STANDARDS OF REPORTING
STROBE guidelines have been followed.
AVAILABILITY OF DATA AND MATERIALS
The data supporting this study's findings are available from the corresponding author [A.N] upon reasonable request.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
The authors would like to acknowledge dental faculty students from Mansoura University and Umm Al-Qura University for their valuable contributions.


