All published articles of this journal are available on ScienceDirect.
Quality of Life in Oral Submucous Fibrosis- A Case Report with a Literature Review
Abstract
Introduction:
Oral Submucous Fibrosis (OSMF) is a potentially malignant disorder commonly found in the Southeast Asian region, classically characterized through restricted mouth opening and burning sensation in the mouth on consuming spicy food. The etiopathogenesis and treatment aspects of OSMF have been extensively researched and reviewed. However, the effect of this condition on the Quality of Life (QoL) of patients has not gained much consideration. The aim of our case report is to highlight the importance of evaluating the QoL in an OSMF patient by using discipline-specific questionnaire and also to present to the readers a review of the recently published research articles on the application of QoL questionnaires in OSMF patients.
Results:
It was observed that most of the researchers used generic and discipline-specific questionnaire for evaluating the quality of life in OSMF patients.
Conclusion:
Evaluation of QoL is recommended during the treatment of OSMF patients. There is a need to develop and employ more of disease-specific QoL instruments for OSMF patients.
1. INTRODUCTION
Oral Submucous Fibrosis (OSMF) is defined as a potentially malignant disorder and a chronic, insidious disease characterized by progressive submucosal fibrosis of the oral cavity and the oropharynx [1, 2]. Although a multifactorial etiology has been suggested for OSMF, gutkha, betel quid chewing has been implicated as the key etiological factor. A combination of areca nut, betel leaf, tobacco, and slaked lime are the components of betel quid [3].
The geographical locations associated with gutkha consumption are India, Pakistan, and South-East Asia. Though many local state governments in India banned the sale of gutkha from the year 2013, the illegal sale still continues. Apart from causing OSMF, gutkha chewing has also been implicated in periodontitis, gastrointestinal abnormalities, oropharyngeal cancers, esophageal cancers, bowel cancer. Gutkha consumption is also associated with toxicities in the immune, reproductive and cardiovascular systems [4].
A recent study among the adolescence and adults of a settlement revealed that 40% of the population was habituated to using chewable betel and tobacco [5]. Besides causing fibrotic changes of the oral mucosa, Betel quid chewing also impacts oral and periodontal health. It has been observed that betel quid chewers exhibit a higher oral hygiene index score, increased periodontal pocket depth, and gingival bleeding [6]. Impairment of day-to-day activities like consuming spicy food is observed in a majority of OSMF patients [7].
When dentists and physicians clinically evaluate the patient with OSMF, attention is given towards determining potential treatment and probable prognosis but not often on the level of impairment and alteration in the quality of life [8].
QoL comprises social, physical & psychological aspects of oral health [8]. The World Health Organization (WHO) defines Quality of life as an ‘individual's perception of his/her position in life in the context of the culture and value system in which she/he lives and in relation to his/her goals, expectations, standards, and concerns' [9]. The QoL is usually measured by means of a questionnaire which can be generic, disease-specific, or discipline-specific in nature [9]. Although each of these questionnaire has its own merits and demerits, the disease-specific questionnaire is able to evaluate the impact of the disease condition on every aspect of day to day life of the affected individual [10]. To highlight the importance of evaluating QoL in OSMF, we present to the readers a case report.
2. CASE DESCRIPTION
A 22-year-old male patient reported to a private dental clinic in Mangalore, India, with complaints of reduced mouth opening for six months. The patient stated that his mouth opening had gradually reduced over the last six months. The patient had a gutkha (a mixture of tobacco and crushed areca nut) chewing habit for one year. The patient stated that he started the gutkha chewing habit to keep himself awake during driving at night. The patient used to work as a driver for a cargo company. He later got addicted to the gutkha chewing habit, and the frequency of this habit increased from one to ten packets per day within a year. The patient stated that he developed a burning sensation in the mouth by consuming spicy and coarse food in the past three months. The patient also stated that he had difficulty in swallowing and had a change in the voice for the past month. During further conversation, he revealed that he had a fear that he had developed mouth cancer. He stated that this fear had an impact on his mental health and physical health. The patient revealed that he had lost up to ten kilograms of body weight in the past six months. He attributed this to the mental stress associated with the fear of oral cancer. He also stated that he had avoided meeting friends and relatives or attending social gatherings due to the prevailing oral condition. The patient, however, had stopped the gutkha chewing habit since the past 3 months.
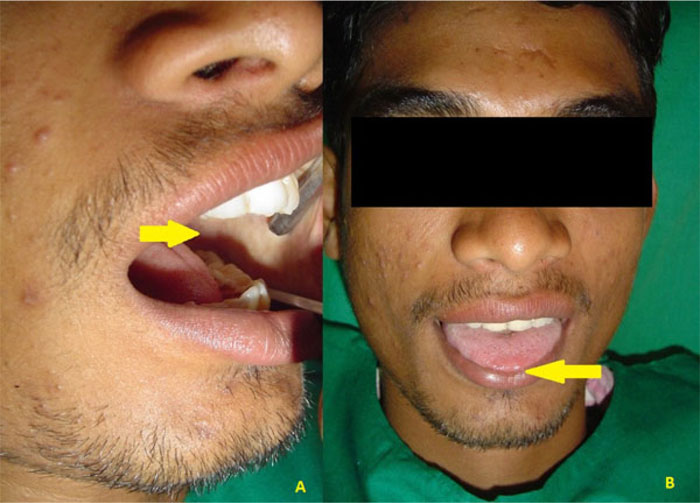
Clinical examination revealed reduced mouth opening (18 mm). There was blanching of the buccal mucosa and reduced movement of the tongue (maximal protrusion = 4 mm from the incisal edges of lower anterior) (Fig. 1A and B). Blanching was also observed in the floor of the mouth, labial mucosa, and soft palate. The patient was unable to puff his cheek. The buccal mucosa was leathery in consistency, and multiple vertical bands could be felt on palpation.
The aim of our case report is to highlight the importance of evaluating the QoL in OSMF patients, using a discipline-specific questionnaire during consultation procedure, and to also present a brief review of the recent questionnaire-based studies on QoL in OSMF patients.
Based on these findings a diagnosis of oral submucous fibrosis was made. The patient filled the OPMD QoL questionnaire in the native language [11]. The overall score obtained from the QoL OPMD questionnaire was 42, indicating a decline in patient’s QoL. The patient was counselled regarding the deleterious effect of gutkha chewing and modifications in his dietary pattern. He was also administered intra-lesional corticosteroids (biweekly basis) and oral antioxidant therapy. The patient was also given a demonstration of the physiotherapy exercise for mouth opening using a stack of ice-cream sticks. The patient was reviewed after one month of treatment. During the review visit, the patient stated that there was a significant reduction in the oral mucosal burning sensation. Clinical examination revealed an increase in mouth opening by 2 mm. However, the tongue protrusion remained unchanged. The patient’s overall score on the OPMD QoL questionnaire was 28, indicating that there was an improvement in the QoL. The patient could not continue with the follow-up appointments for treatment and review of the oral condition due to work-related commitments.
3. AIM
To determine the different types of questionnaires used to measure QoL in OSMF patients.
4. MATERIALS AND METHODS
To determine the types of questionnaires in the recently published studies about the QoL in OSMF patients, we performed a PUBMED-based search for full-text articles in the English language from the year 2015 to 2020. We used “Oral submucous fibrosis,” “Submucus fibrosis,” “OSMF,” “OSF,” “Quality of Life,” “Life Quality,” and “Health-Related Quality Of Life” as keywords for the search. Forty-one articles were identified during the initial search. Eight articles qualified for the final analysis after screening for eligibility. Narrative reviews, case reports, letters to the editors, abstracts, and non-English articles were excluded after the screening procedure. The details of the sample size, methodology, and results of the articles qualifying for the final analysis are described in Table 1.
|
Authors and Year of Publication |
Type of Questionnaire Generic/Discipline-specific/Disease-specific |
Study Design | Psychometric Validation | Sample Size | Language of the Questionnaire | Number of Items/domains in the Questionnaire | Results |
|---|---|---|---|---|---|---|---|
| Gondivkar SM et al. 2019 [12] | Disease-specific OHRQoL-OSF |
Cross-sectional | Validated | 300 clinically diagnosed OSMF patients |
English translated to Marathi | 17 items | The condition-specific OHRQoL-OSF identified OSF patients with impaired oral health-related QoL more easily with greater discriminative properties. |
| Chaudhry K et al. 2019 [13] | GenericWHOQOL- BREF questionnaire |
Cross-sectional | Validated | 200 OSMF patients | English translated to Hindi | 26 items | Quality of life (QOL) scores differed significantly according to age, site affected, habit duration, and severity of OSMF. |
| Gondivkar SM et al. 2018 [14] | Generic Patient-related outcome measure (PROM) |
Cross-sectional | Validated | 30 clinically diagnosed OSMF patients |
English translated to Marathi | 4 domains | PROM reflects an integral aspect of general health and well-being and thus can be used to elucidate the impact of OSF on the quality of life (QoL) of affected individuals. |
| Jena AK et al. 2018 [15] | Generic OHIP-14 questionnaire |
Cross-sectional | Validated | 121 OSMF patients and 115 healthy individuals | English translated to Odia | 7 domains (14 items) |
Stage-4 of oral submucous fibrosis has maximum effect on the quality of life. |
| Chole RH et al. 2018 [16] | Discipline- specific European Organization for Research and Treatment of Cancer Quality of Life head and neck 35 Questionnaire (EORTC QLQ-C35) |
Prospective | Validated | 100 OSMF patients | Not specified | 7 domains (35 items) |
EORTC QLQ-C35 can be used successfully to evaluate the QoL in potentially malignant disorders like OSMF. |
| Sanasare K et al. 2018 [17] | Discipline-specific Chronic Oral Mucosal Diseases Questionnaire (COMDQ) |
Cross-sectional | Validated | 100 OSMF patients | English translated to Hindi and Marathi | 4 domains (26 items) |
COMDQ could be used as a valid and reliable tool for further clinical OSMF research. |
| Tadakmadla J et al. 2017 [11] | Discipline-specific OPMD QoL questionnaire |
Cross-sectional | Validated | 300 study subjects 150 healthy individuals 150 Oral potentially malignant disorders |
English translated to Telugu | 20 items | OPMD QoL questionnaire was valid and reliable in measuring QoL in OSMF. |
| Rimal J et al. 2015 [18] | Generic Oral Health Impact Profile–14 (OHIP-14) |
Interventional | Validated | 74 OSMF patients | English translated to Nepalese | 7 domains 14 items |
Nepalese version of OHIP-14 is a valid and reliable instrument to measure OHRQoL in OSMF patients. |
5. RESULTS
Among the eight studies analyzed, four of them used generic QoL instruments, three of them used discipline-specific QoL instruments, and one study used disease-specific QoL instrument. Oral Health Impact Profile–14 (OHIP-14), Patient-related outcome measure (PROM), and World Health Organization Quality of Life (WHOQOL- BREF) questionnaire were used in generic QoL instrument-based studies.
Oral potentially malignant disorders Quality of life (OPMD QoL), Chronic Oral Mucosal Diseases Questionnaire (COMDQ), and European Organization for Research and Treatment of Cancer Quality of Life head and neck 35 Questionnaire (EORTC QLQ-C35) were used in discipline-specific QoL instrument-based studies. Six studies had a cross-sectional study design, while prospective and interventional study design was followed in the other two studies. All the studies were using validated QoL instruments. The maximal study sample was 300, and the minimal study sample was 30. All eight studies concluded that the QoL instrument used in their respective researches were valid and reliable.
6. DISCUSSION
OSMF patients undergo significant health-related symptoms, including reduced mouth opening, burning sensation, and inability to eat, which are distinct when compared to other oral diseases. Social and emotional distress and constant cancer phobia in OSMF patients often results in increased psychiatric disease [12]. A diagrammatic representation of the factors influencing the quality of life in OSMF patients is described in Fig. (2).
Generic QoL questionnaires are incapable of identifying minor but clinically significant variations related to a specific disease. However, generic questionnaires permit QoL comparisons across different types of diseases [19]. Discipline-specific questionnaires compared the QOL of patients with related diseases [20]. Disease-specific questionnaires have increased sensitivity to disease-specific changes and precisely forecast clinical variations associated with a certain disease. However, disease-specific QoLs do not permit a comparison among different diseases [9].
While most of the researchers used generic specific QoL questionnaires, Tadakmadla et al. developed and validated a questionnaire for patients with oral potential malignant disorders (OPMD) [11]. Prior to developing the questionnaire, inputs were obtained from personal interviews and group discussions with individuals affected by OPMDs. Feedbacks from specialist clinicians were also obtained. After preparing the questionnaire, it was validated using 150 OPMD patients and 150 healthy individuals. The OPMD QoL questionnaire developed by Tadakmadla et al. exhibited good discrimination and convergent validity. Patients with OPMD showed poorer QoL compared to healthy individuals. The authors suggested the application of the OPMD QoL questionnaire in epidemiologic and treatment studies of OPMD. We used the questionnaire by Tadakmadla et al. in our patients to determine the QoL during diagnostic and treatment phases.
Sansare et al. used the Chronic Oral Mucosal Diseases Questionnaire (COMDQ) in a study involving 100 OSMF patients and found that COMDQ was a valid and reliable tool to assess QoL in OSMF patients. It is also important to note that COMDQ appears to be more discipline-specific questionnaire and could be used to compare QoL among oral mucosal disorders [17].

In a systematic review performed by Gondvikar SV et al., it was observed that the majority of the Oral Health-Related (OHRQoL) assessment instruments focused on patients diagnosed with Oral Lichen Planus (OLP), which could not be applied to all OPMD’s, thereby, emphasizing the need for a specific OHRQoL tool for habit-associated disorders such as OSMF and Oral Leukoplakia (OL) [21].
Gondvikar et al. followed a strategy similar to Tadakmadla et al. to develop a questionnaire based on Patient Related Outcome Measure (PROM). The study findings revealed the impact of OSMF on different aspects of a participant’s life. The effect of OSMF was not just restricted to local discomfort and functional impairment but also interfered with other important domains, namely psychological, social, and physical wellness. The researchers stressed that viewpoints from psychological and social aspects should be considered along with a clinical examination to effectively manage the overall health care needs of the OSMF patients [11, 14]. Gondvikar SV et al. also developed and assessed the validity of a novel disease-specific Oral Health-Related QoL (OHRQoL-OSF) instrument specifically for patients diagnosed with OSMF with a Likert type four-point rating scale [12]. They followed and tested various steps such as item generation, item reduction, pretesting, validity testing, and reliability testing. They concluded that the OHRQoL-OSF instrument could be used as an adjunctive tool in clinical examination for evaluating patient well-being and perception.
In a recent article, Gondvikar SV et al. analysed the effects of socioeconomic status (SES) and its variables on the QoL in patients diagnosed with OSMF. He reported that patients with lower SES were diagnosed with advanced stages of OSMF with poor QoL, thereby highlighting the importance of SES as a major determinant [22].
Gondivkar et al. carried out a systematic review to assess the most appropriate OHR-QoL instrument for OSMF using the Consensus-based Standards for the selection of health Measurement Instruments (COSMIN) checklist. They stated that selecting the right instrument in routine practice was challenging, as the psychometric quality of measurement was not explored. Their compiled study included three generic and one disease-specific questionnaire based on the literature review as per the PRISMA guidelines. The review reported that using disease-specific OHRQoL-OSF was more valid and reliable as compared to OPMDQoL because it helps to recognize disease severity and define management protocol. They also stated that selecting an instrument depends on the choice of the clinician [21].
Chaudhry et al. performed a cross-sectional study to assess the QoL of 150 patients diagnosed with OSMF using a generic WHOQoL-BREF questionnaire. The questionnaire focused on physical health, psychological health, environmental health, and social relationships. On statistical analysis, a significant difference in the QoL was observed between the diseased and the control groups. The study reported that patients with OSMF had a negative impact on their social and personal relationships [13].
Chole RH et al. used a discipline-specific European Organization for Research and Treatment of Cancer Quality of Life head and neck 35 Questionnaire (EORTC QLQ-C35) along with Performance Status Scale for Head and Neck Cancer Patients (PSS-HN) to assess the QoL in OSMF patients receiving treatment with spirulina and intralesional steroids. The key feature of their study was that the researchers measured QoL outcomes at different intervals after diagnosis of OSMF when the patients were undergoing clinical trials with different medications. The QOL scores at these different intervals were compared to baseline values. The authors stated that QOL is an important outcome to be considered in clinical trials and routine treatment [16].
Tyagi et al. conducted a study on 30 patients receiving treatment for oral submucous fibrosis by using standardized measures of quality of life (QOL). The Chronic Oral Mucosal Diseases Questionnaire (COMDQ) was employed in the study. They stated that the questionnaire provided information for determining potential treatment options and also provided insight into the prognosis. It was also stated that the questionnaire might not directly reflect the resulting level of impairment resulting from the disease [8].
Oral potentially malignant disorders Quality of life (OPMD QoL), Chronic Oral Mucosal Diseases Questionnaire (COMDQ), and European Organization for Research and Treatment of Cancer Quality of Life head and neck 35 Questionnaire (EORTC QLQ-C35) were discipline-specific QoL instrument used to evaluate QOL patients. The EORTC QLQ-C35 consists of items explicitly for cancer of the head and neck region. However, it might be of lower relevance when evaluating QoL in patients with OPMDs. While developing and validating COMDQ, patients with OSMF and oral leukoplakia were not involved, thereby reducing its relevance in evaluating the QoL in OSMF and oral leukoplakia patients.
Jena et al. used the oral health impact profile-14 (OHIP-14) to assess the QoL in OSMF patients. The researchers observed that QoL among male study subjects was severely affected by OSMF. They also observed that the Stage-4 OSMF had maximum effect on the QoL when compared to healthy study subjects. Apart from oral discomfort, individuals with OSMF often reported psychological stress, especially when they were seeking treatment during their first visit without knowing their diagnosis and prognosis [16]. This type of anxiety was noticed in our case as well. Individuals with OSMF, particularly those cases in which lip and tongue were involved, frequently reported social embarrassment [23, 24]. In one of the qualitative studies, patients with OSMF reported a lack of enthusiasm, low esteem, and embarrassment at their workplaces. The researchers have found that the fear associated with the term “cancer” is responsible for psychological stigma linked with OSMF in the southeast Asian region [23]. Many of the factors associated with social embarrassment were observed in our case. The use of an appropriate QoL questionnaire during every consultation with the patient provides the dental surgeon with a complete evaluation of the patient’s general and mental health status, which is key for the success of the treatment.
A holistic management of OSMF is only possible if the medical management is coordinated with appropriate patient education, timely patient counseling, and constant assurance about the success of the available treatment modalities [25-28].
7. LIMITATIONS
One of the limitations of this article is that only one source was used for data collection. We plan to conduct future studies using multiple databases for data collection.
CONCLUSION AND SCOPE FOR FUTURE RESEARCH
Currently, there is a scarcity of research studies using disease-specific QoL assessment questionnaires in OSMF patients, in spite of the higher prevalence of this condition in certain parts of the world. However, there are a few path-breaking studies that have addressed the importance of assessing the quality of life in individuals with OSMF. Assessment of the quality of life of OSMF patients is intricate because of the vast number of variables that determine the patient’s self-perception. However, there is a scope for future research encompassing all the aspects determining the QoL in individuals with OSMF. It is evident that the future scope of the research will be based on developing and validating disease-specific questionnaire for OSMF rather than using generic QoL questionnaires.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this research.
CONSENT FOR PUBLICATION
Informed written consent obtained for using patient photographs and data obtained.
STANDARDS OF REPORTING
CARE guideline and methodology were followed.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.
SUPPLEMENTARY MATERIAL
Supplementary material is available on the publisher’s website along with the published article.


