All published articles of this journal are available on ScienceDirect.
Shear Bond Strength and Optical Properties of Resin Composite - Layered Provisional Poly(methyl methacrylate) (PMMA)
Abstract
Aims:
To compare the shear bond strength between resin composite and Poly(methyl methacrylate) (PMMA) with various bonding protocols and to evaluate the optical properties of resin composite - layered provisional Poly(methyl methacrylate) (PMMA).
Materials and Methods:
Eighty cylindrical shape specimens were fabricated from self-polymerized provisional Poly(methyl methacrylate) (PMMA) and they were randomly divided into eight groups. Poly(methyl methacrylate) (PMMA) was mixed and bonded onto the specimens as a positive control group. Resin composite was bonded to MMA-wetted surface without bonding agent as a negative control group. All remaining groups were bonded to resin composite using different bonding agents (Scothbond Universal, Luxatemp glaze&bond, and HC Primer) with and without MMA wetting. Shear bond strength testing was performed using a universal testing machine. Various shades of 0.5 mm-thick resin composites were layered onto 1.5 mm-thick PMMA both light and dark shade, with the most effective bonding protocol. Color differences between resin composite and – layered provisional Poly(methyl methacrylate) (PMMA) were measured using Spectrophotometer.
Results:
Bonding resin composite onto Poly(methyl methacrylate) (PMMA) using luxatemp glaze, bond and HC Primer without methyl methacrylate wetting provided statistically significantly lower bond strength than those of the MMA-wetted Poly(methyl methacrylate) (PMMA) surface. The highest shear bond strength was achieved with the application of Scothbond Universal Adhesive regardless of MMA wetting. The colors of resin composite - layered provisional Poly(methyl methacrylate) (PMMA) were different from the original resin composite color with ΔE results greater than the acceptable threshold (>3.7).
Conclusion:
Resin composites were able to effectively bond to the MMA-wetted Poly(methyl methacrylate) (PMMA) surface with the application of a tested bonding agent. Layering Poly(methyl methacrylate) (PMMA) with 0.5 mm-thick resin composite could not modify the Poly(methyl methacrylate) (PMMA) shade to the original resin composite color.
1. INTRODUCTION
The provisional restorations need to satisfy the require- ments of pulpal protection, occlusal function, strength, and esthetics [1-3]. They should also have sufficient working time and -simple fabrication techniques. Poly(methyl methacrylate) (PMMA) is extensively being used for provisional restoration fabrication. Resin composite materials, such as bis-acryl composite or Urethane Dimethacrylate (UDMA) are gaining popularity for their use as a provisional restoration due to their superior esthetic and good physical properties. However, composite materials are more expensive compared to conventional PMMA. In addition, they are usually supplied in automix cartridge, which wastes some materials. Although the physical properties of PMMA have gradually been improved, esthetic parameters are still questioned. Teeth with color contrast appearance or high translucency are limited by the availability of PMMA shades. The combination of PMMA and light-cured resin composite has been proposed by layering restorative resin composite onto PMMA to enhance the esthetic appearance. Resin composite has widely been used due to its high wear resistance, ease of use, and excellent esthetic outcome along with the availability of various shades and translucencies . Therefore, the idea of modifying the PMMA restorations with resin composite for esthetic reasons seems to be possible. The thin layer of resin composite effectively bonded to the beneath PMMA would provide a satisfactory esthetic result and economic benefit compared to the whole bulk of resin composite provisional restoration.
Most of the published studies on adhesion of resin composite to PMMA have been conducted in terms of clinical methods to modify and repair acrylic denture teeth with resin composite [4-6]. Polymeric materials are bonded either to themselves or to other polymers. The adhesion mechanisms are mechanical coupling, molecular bonding, and thermodynamic adhesion [7]. Roughening the surface simply increases the surface area for more molecular bonding interactions and provides mechanical interlocking. Molecular bonding mechanisms require an intimate contact and bring intermolecular forces between adhesive and substrate and chemical interactions.
The studies of direct bonding of resin composite to PMMA are very limited. Most of the studies were performed to evaluate the bonding of resin composite to acrylic denture teeth for the purpose of repairing. However, the polymerization process of Methyl Methacrylate (MMA) and Bisphenol A-glycidyl Methacrylate (Bis-GMA) follows a similar pattern [8]. Thus, some chemical bonding may occur, although they are different in chemical structures. Boyer and Chalkley investigated the bonding between acrylic laminates and resin composite [9]. They stated that bond strength was increased by pretreating the acrylic surface with several solvents to soften or swelled the thermoplastic substrate. Then, the monomeric adhesive was diffused into the surface and polymerized. The transverse strength of repaired heat-cured acrylic resin by wetting the surface with MMA before bonding to acrylic resin was investigated and found that bond strength increased as the duration of MMA wetting increased maximum at 180 s [10]. Several studies confirmed that the pre-wetting surface with the MMA and application of bonding agent significantly increased the bond strength between resin composite and acrylic resin denture teeth [11-13].
This study proposes to modify provisional restorations by using light-cured resin composite labial veneers facing in conjunction with provisional PMMA material as substructures. However, the study regarding the bonding between provisional PMMA and resin composite is still limited. In addition, novel primers have been introduced for improving the adhesion between different substrates. The evaluation of bond strength between PMMA and resin composite with new strategies should be performed. Additionally, to obtain optimal esthetic color properties, color-matching between PMMA and resin composite should be evaluated. Resin provisional PMMA should provide the color as the original resin composite shade. However, with the thin layer of resin composite, the final restoration shade is a matter of interest. Moreover, the PMMA shade itself may affect the final color of the layered restoration. There is no previous study on this issue. According to the study by Gross and Moser, the color difference of 2.0 ΔE was set as the “perceptible threshold” [14], whereas the study of Johnston and Kao designated the color difference of 3.7 ΔE as the “acceptable threshold” [15].
The aims of this study were evaluate the shear bond strength of resin composite bonded to self-cure PMMA with various bonding protocols and to evaluate the optical properties of this resin provisional PMMA. The null hypotheses were that there was no difference in the shear bond strength of resin composite bonded to self-cure PMMA among various bonding protocols. Moreover, there was no difference in color between resin provisional PMMA and bulk resin composite with the same shade.
2. MATERIALS AND METHODS
Materials, composition, and application procedures used in this study are shown in Table 1.
2.1. Shear Bond Strength Test
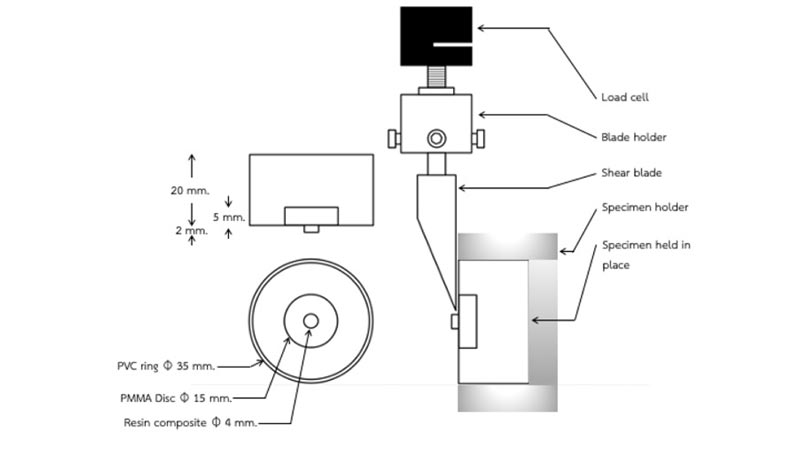
A schematic diagram of specimen preparation and shear bond strength test is shown in Fig. (1). Eighty self-polymerized provisional PMMA (Unifast III, GC America Inc., Illinois, USA) cylindrical shape specimens, 15 mm in diameter and 5 mm in thickness, were prepared using a cylindrical silicone mold. The material was mixed and cured according to manufacturer’s instruction. All specimens were embedded in denture base acrylic resin in Polyvinylchloride (PVC) rings and stored in distilled water for 48h. The specimens were randomly divided into eight groups of ten specimens each. The bonding surfaces were grounded flat and polished under running water with series of silicon carbide papers of 100, 400, and 600 grit, ultrasonically cleaned with distilled water for 5 min, and dried with compressed air. The roughness values were measured with a profilometer (Surfcorder SE2300, Kosaka Laboratory Ltd, Tokyo, Japan).
| Product | Composition | Manufacturer | Application procedures |
|---|---|---|---|
| Unifast III | methyl methacrylate (MMA), dimethacrylate, dibenzoyl peroxide, iron(III) oxide, UV-light absorber, accelerant | GC America Inc. Illinois, USA | Dispense the powder in a rubber cup and add liquid, quickly mix with a plastic spatula for 10-15 s, immediately pour the mixture into the mold, and left it to cure for 5 min |
| Scotchbond Universal Adhesive |
MDP phosphate monomer, dimethacrylate resins, HEMA, VitrebondTM Copolymer, filler, silane, ethanol, water | 3M ESPE, Minnesota, USA | Apply onto the PMMA surface with the disposable applicator and rubbed for 20 s followed by air blow for 5 s and light-curing for 20 s |
| Luxatemp glaze & bond | multifunctional acrylates, methyl methacrylate, catalysts, stabilizers, additives | DMG, Hamburg, Germany | Apply onto the PMMA surface with the disposable applicator and allowed material to work for 20 s, followed by light-curing for 20 s |
| HC Primer | acetone, methyl methacrylate, UDMA, polymerization initiator | SHOFU Inc., Kyoto, Japan | Apply onto the PMMA surface with disposable applicator followed by air blow for 5 s and light-curing for 20 s |
| Filtek Z350 | bis-GMA, UDMA, TEGDMA, bis-EMA, filler | 3M ESPE, Minnesota, USA | Condense into the mold and light-cure for 40 s |
| Treatment groups (n=10) | ||||||||
|---|---|---|---|---|---|---|---|---|
| -ve | +ve | Uni | UniW | Lux | LuxW | Hc | HcW | |
| Wetting with MMA for 3 minutes | + | + | + | + | + | |||
| Application of Scotch Bond Universal | + | + | ||||||
| Application of Luxatemp glaze&bond | + | + | ||||||
| Application of HC Primer | + | + | ||||||
| Build up with PMMA | + | |||||||
| Build up with resin composite | + | + | + | + | + | + | + | |
There were eight experimental groups according to the bonding protocol. Bonding strategies given to each group of specimens are described in Table 2. Specimens in the positive control group were wetted with MMA for 3 min [10]. Then, the mixture of PMMA was condensed into the cylindrical-shaped metal split mold, 4 mm in diameter and 4 mm in height, and left for self-polymerized for 5 min. For the negative control group, after wetting PMMA surface with MMA for 3 min, resin composite (Filtek z350, 3M ESPE, Minnesota, USA) was condensed into the mold without any bonding agent application and light-cured for 40s with the intensity of 600 mW/cm2.
For the other six remaining groups of specimens, resin composite was bonded to prepared PMMA surface with one of the surface treatment protocols; 1) Uni: Scotchbond Universal Adhesive (3M ESPE, Minnesota, USA) 2) UniW: PMMA surface was pre-wetted with MMA for 3 min prior to the same procedure as 1). 3) Lux: Luxatemp glaze & bond (DMG, Hamburg, Germany) 4) LuxW: PMMA surface was pre-wetted with MMA for 3 min prior to the same procedure as 3). 5) Hc: A single uniform coat of the HC Primer (Shofu Inc., Kyoto, Japan) 6) HcW: PMMA surface was pre-wetted with MMA for three minutes prior to the same procedure as 5).
After PMMA surface treatment, resin composite was filled in the metal mold described earlier and light-cured for 40s. The metal split mold was then gently removed. All specimens were stored in distilled water for 24h before shear bond strength testing.
For shear bond strength measurement, the specimens were positioned in the universal testing machine (Lloyd Instruments, Model LRX-Plus, AMETEK Lloyd Instrument Ltd., Hampshire, UK). A metal blade was set to move vertically to the interface at a crosshead speed of 0.5 mm/min until debonding of the PMMA-resin composites interface occurred. The maximum load (N) was recorded and divided by the bonding area (mm2) to exhibit the bond strength in MPa. The modes of bonding failure were examined with 50x magnifying digital microscope and classified as one of the following categories: adhesive failure at the interface, cohesive failure within the PMMA, and mixed failure of those two modes.
Shear bond strength values were distributed as assessed by the Shapiro-Wilk test, and there was homogeneity of variances assessed by Levene's test. A one-way ANOVA was performed to compare means among eight experimental groups, and Tukey’s HSD was used for post hoc comparison with the 95% level of confidence.
2.2. Optical Properties Testing
After the shear bond strength test, the optimal bonding protocol was selected and used for optical properties testing. Forty PMMA specimens of each light shade (A1) and a dark shade (A3.5), the diameter of 30 mm and thickness of 1.5 mm, were prepared using Teflon mold. The polymer and monomer were mixed following the manufacture’s instruction and packed into the mold. The glass slab was placed over the mold, compressed, and left for self-polymerized for 5 min. Then, 0.5 mm-thick resin composites shade A1, A2, A3, and A4 were layered onto the surface of PMMA using selected bonding protocol. Eight experimental groups were obtained with four shades of resin composite on light(L) and dark(D) shades of PMMA; LA1, LA2, LA3, LA4, DA1, DA2, DA3, and DA4. Thickness was controlled by using two pieces of 0.5 mm-thick acetate strips as stoppers. Resin composite was filled, covered, and compressed onto the treated surface using a glass slab. Finger pressure was exerted and light-cured for 40s. The glass slab and acetate strips were then removed. The excess area of specimens was trimmed and then stored in distilled water for 24h before optical properties measurement was done.
For the control groups, three specimens of each shade of resin composite (A1, A2, A3, and A4) were prepared into a cylindrical shape using Teflon mold, 15 mm in diameter and 4 mm in thickness which is reached the infinite optical thickness of the materials to measure the true color of the material regardless of the thickness. Resin composite was condensed into the mold, compressed with a glass slab, and light-cured for 40s.
The optical parameters were determined using a spectrophotometer (ColorQuestXE, Hunter Associates Laboratory, Inc., Virginia, USA.). The spectrophotometer was set to the standard illumination source D65 according to the CIELAB color scale. Three measurements of L*, a*, and b* were recorded for each specimen and averaged to obtain a value for the following calculations.
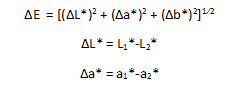 |
3. RESULTS
The surface roughness (Ra) of PMMA discs was between 0.25 – 0.40 µm with a mean of 0.34 ± 0.05 µm. The means and standard deviations of shear bond strength are shown in Table 3. One-way ANOVA revealed that shear bond strength values were statistically significantly different among bonding protocols (P < 0.001). The initial bond strength of 0.21 ± 0.04 MPa was obtained in the negative control group which resin composite bonded to PMMA without a bonding agent. The mean shear bond strength of the positive control group, in which PMMA was bonded to pre-wetted PMMA, was 9.67 ± 1.11 MPa. Applying Scotchbond Universal Adhesive onto PMMA surface without MMA wetting (Uni) provided the highest mean shear bond strength (11.30 ± 0.77 MPa) and comparable to that of the non-wetted group (11.06 ± 0.93) (P > 0.05). Applying Luxatemp glaze & bond and HC Primer onto PMMA surface without MMA wetting (Lux and Hc) resulted in the shear bond strength of 6.44 ± 2.07 MPa and MPa, respectively, which were significantly lower than those of the MMA wetted PMMA surface, 11.19 ± 1.16 MPa, and 9.92 ± 1.53 MPa respectively (P < 0.05).
There was no statistically significant difference in shear bond strength among the groups of pre-wetted PMMA surface (UniW, LuxW, and HcW) (P > 0.05), and they were comparable to that of the positive control group. On the contrary, without MMA wetting, the high shear bond strength was achieved only with Scotchbond Universal Adhesive (Uni) using Luxatemp glaze & bond and HC Primer had resulted in statistically significant inferior bond strength.
The distribution of fracture modes of debonded specimens is shown in Fig. (2). For the groups in which resin composite was bonded to pre-wetted PMMA surface, except the HcW group, the specimens are more likely to fail as a cohesive failure. The groups without MMA wetting mostly failed as adhesive failures. With the use of Scotchbond Universal Adhesive, nearly 100% displayed cohesive failures regardless of MMA wetting.
L*, a*, and b* values of various shades of resin composite specimens and eight experimental groups are shown in Table 4. The means and standard deviations of ΔE results of layered resin composite shades A1, A2, A3, and A4 bonded to light shade PMMA were 9.79 ± 0.21, 10.92 ± 0.14, 12.31 ± 0.15, and 16.83 + 0.13 respectively, and to dark shade, PMMA were 8.40 ± 0.12, 7.27 ± 0.14, 7.19 ± 0.11, and 10.62 ± 0.18, respectively as shown in Table 4. The ΔE results did not reach the acceptable threshold.
|
Treatment groups (N=10) |
Mean (SD) (MPa) |
|---|---|
| Negative control | 0.21 (0.04)a |
| Positive control | 9.67 (1.11)b |
| Uni | 11.30 (0.77)b |
| UniW | 11.06 (0.93)b |
| Lux | 6.44 (2.07)c |
| LuxW | 11.19 (1.16)b |
| Hc | 6.82 (1.23)c |
| HcW | 9.92 (1.53)b |
| Group | - | Mean (SD) | - | |
|---|---|---|---|---|
| L* | a* | b* | ||
| Resin Composite | A1 | 67.66 (0.13) | -0.29 (0.03) | 10.34 (0.02) |
| A2 | 65.34 (0.03) | 2.11 (0.02) | 13.55 (0.01) | |
| A3 | 63.46 (0.03) | 2.55 (0.03) | 16.02 (0.08) | |
| A4 | 56.07 (0.03) | 2.97 (0.01) | 17.57 (0.04) | |
| Resin composite-layered PMMA | LA1 | 76.59 (0.21) | 1.52 (0.11) | 13.86 (0.27) |
| LA2 | 75.79 (0.14) | 2.37 (0.09) | 16.60 (0.33) | |
| LA3 | 74.83 (0.13) | 2.38 (0.14) | 20.71 (0.10) | |
| LA4 | 71.71 (0.15) | 3.65 (0.08) | 23.75 (0.16) | |
| DA1 | 67.43 (0.07) | 5.04 (0.05) | 16.81 (0.15) | |
| DA2 | 66.74 (0.24) | 6.01 (0.07) | 19.49 (0.14) | |
| DA3 | 65.27 (0.08) | 6.10 (0.02) | 22.00 (0.10) | |
| DA4 | 63.10 (0.12) | 7.00 (0.04) | 24.43 (0.15) | |

| Compared groups | ΔE Mean (SD) | Compared groups | ΔE Mean (SD) | ||
|---|---|---|---|---|---|
| Exp. | Control | Exp. | Control | ||
| LA1 | A1 | 9.79 (0.21) | DA1 | A1 | 8.40 (0.12) |
| A2 | 11.29 (0.22) | A2 | 4.87 (0.14) | ||
| A3 | 13.36 (0.22) | A3 | 4.77 (0.09) | ||
| A4 | 20.91 (0.22) | A4 | 11.58 (0.07) | ||
| LA2 | A1 | 10.63 (0.20) | DA2 | A1 | 11.17 (0.12) |
| A2 | 10.92 (0.14) | A2 | 7.27 (0.14) | ||
| A3 | 12.37 (0.13) | A3 | 5.91 (0.18) | ||
| A4 | 19.77 (0.14) | A4 | 11.26 (0.23) | ||
| LA3 | A1 | 12.89 (0.14) | DA3 | A1 | 13.52 (0.84) |
| A2 | 11.90 (0.15) | A2 | 9.35 (0.10) | ||
| A3 | 12.31 (0.15) | A3 | 7.19 (0.11) | ||
| A4 | 19.04 (0.14) | A4 | 10.68 (0.11) | ||
| LA4 | A1 | 14.56 (0.12) | DA4 | A1 | 16.52 (.11) |
| A2 | 12.13 (0.13) | A2 | 12.15 (0.12) | ||
| A3 | 11.37 (0.12) | A3 | 9.53 (0.14) | ||
| A4 | 16.83 (0.13) | A4 | 10.62 (0.18) | ||
4. DISCUSSION
Polymers bonding requires mechanical coupling, molecular bonding, and thermodynamic adhesion [7]. From surface roughness data, the assumption was made that the surface roughness of all PMMA specimens was standardized. Although roughening PMMA surface, whether bonding to resin composite or PMMA itself, has increased debonding-resistance [4-6], some studies stated that debris from roughening process prevented flowing of adhesive and decreases the Van der Waals force [16]. In this study, 600 grit carbide paper was used in PMMA surface preparation exhibited the dental bur gliding geometry for mechanical bond mechanism and ultrasonic clean was done to prevent the debris accumulation (Table 5).
This study compared the effect of different bonding protocols. The results showed that shear bond strength values were statistically significantly different among the groups. According to the results, the shear bond strength of the negative control group was statistically significantly lower than those of others. In this group, resin composite was directly cured on MMA wetted PMMA surface without any bonding agent. Although the chemical bond possibly occurred, resin composite was light-cured onto the polymerized PMMA, which already obtained a high degree of conversion. The free double bond might not be enough to be copolymerized with the added resin composite. Even with MMA wetting, which is believed to dissolve the polymerized PMMA surface and increase the PMMA surface potential for chemical interaction and adaptability of added resin composite, the bond strength was still very low. There was evidence that resin composite had high viscosity and poor wettability [17]; therefore, it could not flow and penetrate the MMA wetted surface even if it softened and swelled. In the positive control group, the mixture of PMMA was bonded to wetted PMMA surface. The high fluidity of the PMMA mixture produced good penetration resulting in better adhesion between these two identical materials.
Previous studies reported that wetting PMMA surface with MMA as a pretreatment was effective for the bond strength [10, 13]. In addition, several studies have verified that the application of some bonding agents was necessary for bonding resin composite to PMMA [13, 18]. However, this study found that the application of Scotchbond Universal Adhesive provided the highest shear bond strength even without MMA wetting. There was no significant difference in bond strength whether MMA was wetted or not when using this bonding agent. The observation of failure modes in these groups showed cohesive failure within PMMA. This implied that the shear bond strength values could not be directly evaluated due to the strong bond between two substrates causing the failure initiation from some flaws within PMMA itself. Scotchbond Universal Adhesive contains MDP and silane. The roles of silane and MDP on bonding to PMMA are still uncertain. However, ethanol in this bonding agent is a plasticizer that could soften the PMMA surface and enhance bonding performance to PMMA. Silane and MDP might improve bonding to resin composite. Additionally, there are fillers in Scotchbond Universal Adhesive, which could be a responsibility in reinforcing its strength.
In the present results, there was no statistically significant difference of shear bond strength among the groups which bond resin composite onto pre-wetted PMMA surface using bonding agents (Uni, Lux, and Hc) and positive control group. These results implied that wetting with MMA was a necessary procedure for some bonding agents. Both Luxatemp glaze & bond and HC Primer contained their specific solvents. Luxatemp glaze & bond contained MMA, whereas HC Primer contained both MMA and acetone in their formulations. They are supposed to achieve high bond strength without using MMA wetting procedure. The explanation was that MMA concentration in the formulation and contact time might not be enough to dissolve the PMMA surface. The acetone in HC Primer was a non-polymerized solvent; therefore, it could not act as the plasticizer even though it was a strong solvent [11].
The best bonding protocol was selected to bond specimens for the optical properties test. After layering the PMMA substrate with resin composite, color differences between each experimental group and its veneering composite shades were evaluated to determine whether the layered specimen turn into its veneering resin composite shade or not. The null hypothesis was rejected. The ΔE results were not reaching the acceptable threshold [15]. This indicated that 0.5 mm-thick resin composite could not modify the PMMA shades to their color. Jae et al. found that there was a strong positive correlation between thickness and masking effect of resin composites [19]. All specimens were not regarded as acceptable with the exception of 3 mm thickness PMMA specimens. It was also found that at least 3 mm-thick of PMMA provisional restoration was required to achieve the acceptable threshold, which is not clinically relevant. Arikawa et al. applied a thin layer of light-cured paint-on resin to the surface of the restoration and reported that even a thin layer of paint-on resin could effectively modify the color of restoration [20, 21].
The resin composite used in this study was the Filtek Z350. Generally, there are four opacities choices available which are Translucent, Enamel, Body, and Dentin. The Body shades were used in this study as they claimed to properly use as single shade restoration. They are slightly opaquer than the Enamel so that they can properly mask the PMMA substrate, but they still have a proper translucency to use as anterior teeth restorations.
There were several studies mentioned about the masking abilities of resin composite [22-24]. Kim et al. evaluated the masking ability of six brands of resin composite, including Filtek Z350, and reported that with a thickness of 0.5 and 1 mm. of resin composite, the C4 background was properly masked while the black background required thicknesses of 1.0 – 2.0 mm [23]. Miotti et al. reported that Filtek Z350 XT was capable of masking the C4 color background [24]. One previous study determined the critical thickness at which translucent (TP) dropped below 2.0 to mask a black background and reported that opaque composite required 2.56 mm of thickness to achieve the 2.0 TP value [22]. The thickness of 0.5 mm of resin composite was used in this experiment because the strength of PMMA at 1.5 mm-thickness needed to be maintained corresponding to the real clinical situation. Although the previous studies reported that 0.5 mm of Body shade of resin composite can mask the C4 background [23]. Contrary to the present study, the color difference results showed that 0.5 mm. of A1 A2 A3 and A4 resin composite shade could not mask the light and dark PMMA background. The explanation was that PMMA substrate both light and dark colors used in this study were A1 and A3.5. The thickness of the PMMA substrate was only 1.5 mm. The specimens were placed over a white background to mimic the color characteristic of temporary cement. This study inferred that with a 0.5 mm thickness of resin composite, even an opaque shade could not effectively mask the PMMA color. The color differences results should be done comparing with the gold standard shade guide system for further investigation. In addition, increasing resin composite thickness might provide more positive results. The effect of thickness of resin composite on color properties and the strength of the layered materials with different thicknesses should be additionally assessed.
CONCLUSION
Within the limitation of this study, it can be concluded that resin composites were able to effectively bond to MMA-wetted PMMA surface with the application of a tested bonding agent. The application of Scotchbond Universal Adhesive provided a high shear bond strength regardless of MMA wetting. Layering PMMA with 0.5 mm-thick resin composite could not modify the PMMA shade to the original resin composite color.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this research.
CONSENT FOR PUBLICATION
Not applicable.
AVAILABILITY OF DATA AND MATERIALS
Not applicable.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


