All published articles of this journal are available on ScienceDirect.
Extended Erosive Oral Lichen Planus Treated with a very Low-Level Laser Therapy: A Case Report
Abstract
Background:
Oral lichen planus is a chronic idiopathic inflammatory disease that affects the skin and mucous membrane and involves about 1-2% of the population. The management of this pathology aims to control symptoms. Clinically, it can appear as a plaque, in reticular form, or an erythematous/atrophic form. The treatment options include different classes of drugs and non-drug therapies such as a laser. In addition, most drug treatments include numerous side effects.
Objective:
The aim of this work is to evaluate the clinical effectiveness of a particular type of very Low-Level-Laser Therapy for the management of an erosive oral lichen planus case.
Methods:
An extensive form of erosive Oral Lichen Planus was treated using a Low-Level Laser Therapy with a 660 nm diode laser. The treatment was performed once per week for two sessions of five minutes each. Different outcome variables were examined: the size of lesions, evolution of pain symptoms, and presence of side effects and stability of the therapeutic results in the follow-up period.
Results:
After a week, the lesion appeared more homogenous, and the erythematous areas underwent a reduction with a simultaneous decrease in symptoms. After two weeks, the lesion seemed completely healed with the disappearance of pain. The follow-up continued for the other four months, and no relapse was reported. No adverse effects were observed during the study.
Conclusion:
This study suggests that Low-Level Laser Therapy with very low power parameters could be a safe and successful treatment for extended oral erosive lichen planus lesions.
1. INTRODUCTION
Oral Lichen Planus (OLP) is a chronic idiopathic inflammatory disease that affects the skin and mucous membrane, characterized by an autoimmune reaction versus keratinocytes mediated by T lymphocytes [1]. The pathology proved more than 1% of the population [2]. OLP affects middle-aged adults of both sexes, with a slight predominance in women [3]. Etiology is still unknown, but some factors are associated with it as genetic factors having an association with some HLA [4, 5], HCV [6], dental material, drugs [7, 8] and infective agents [9, 10]. Clinically, OLP can appear as reticular (with Wickham striae), plaque, papule, atrophic, erosive and bullous [11]. OLP is associated with several systemic diseases [12]. This influences the treatment that aims to resolve the symptoms of the disease [13]. OLP can be treated with drugs and surgical treatments. Pharmacological therapy consists of the use of corticosteroids and other immunosuppressant or immunomodulatory drugs [14]. Non-pharmacological therapy includes PUVA [15], photodynamic [16] and laser therapy [17]. Although corticosteroids represent the main treatment for OLP, they are responsible for side effects like candidiasis, adrenal insufficiency, and discomfort during the application, especially if administered systemically and for a long time [18]. Another treatment option is the Low-Level Laser Therapy (LLLT) used for the treatment of OLP [19]. The use of LLLT is a non-pharmacological and non-invasive clinical alternative modality for the treatment of OLP, which has potential analgesic, anti-inflammatory, immuno-modulatory, and biostimulating effects, with minimum adverse effect [20]. Different types of laser were tested as Helium-Neon [21], CO2 [22] and diode laser [23]. Each type of laser has different parameters, such as wavelengths, intensities, powers, and different durations, number of sessions, and therapeutic approaches that have been documented for laser therapy. The aim of this article is to report a case of a heterogeneous form of OLP treated with a particular type of LLLT following the CARE Guidelines.
2. CASE REPORT
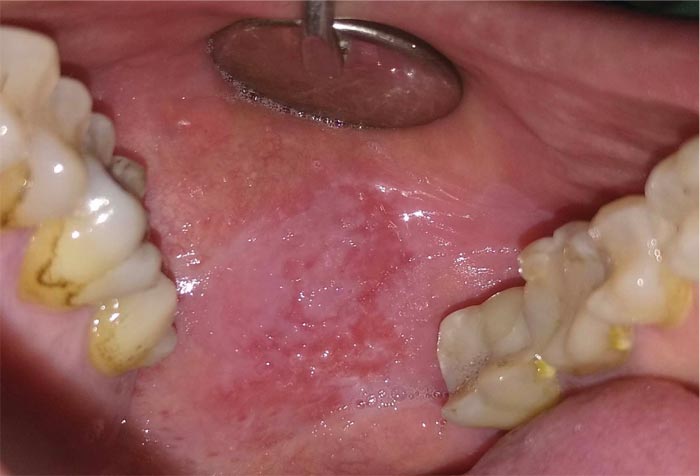
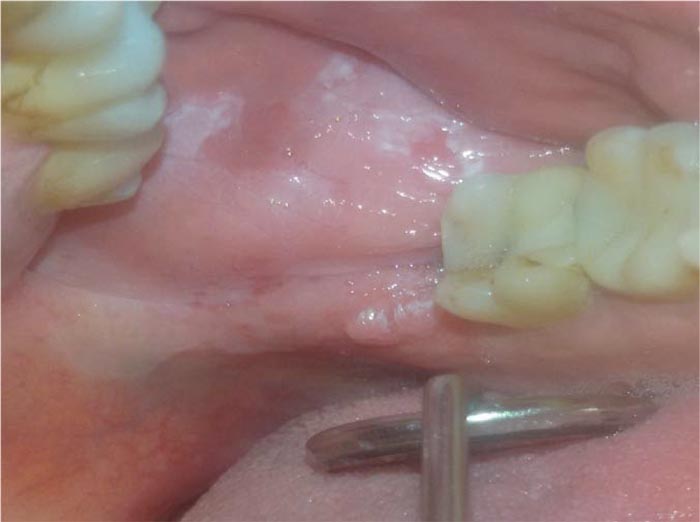
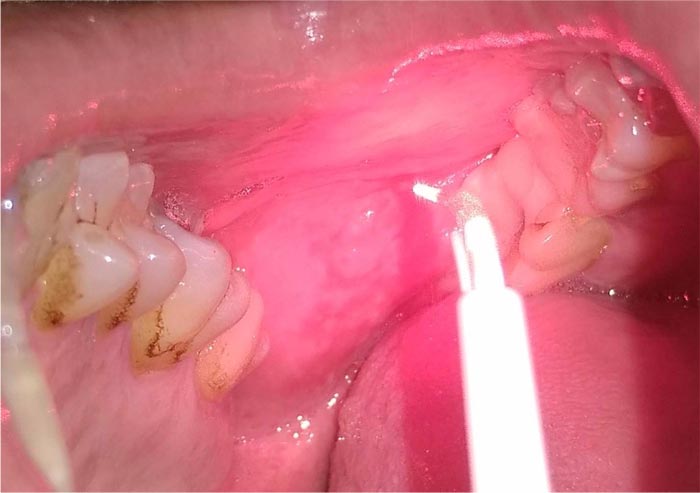
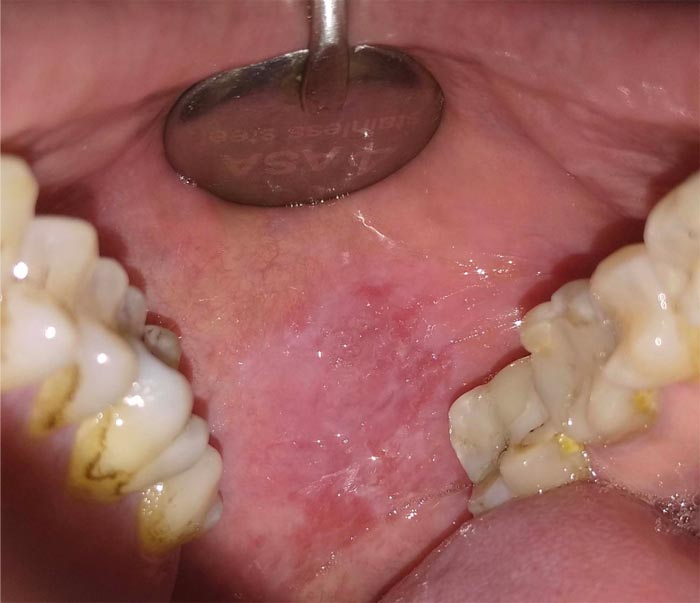
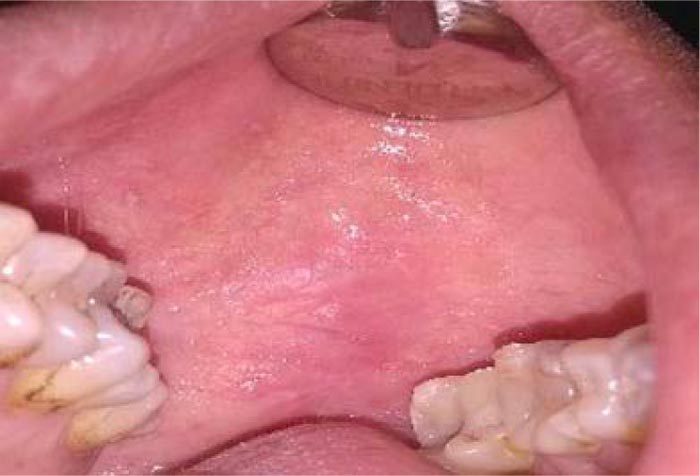
We observed a 42-years old male patient with a heterogeneous form of OLP, with 3 cm of diameter (Fig. 1), and already excised squamous papillomas in the left cheek presented five months ago (Fig. 2). He reported mild pain and a burning sensation in the area of the lesion. The patient generally had good health and reported a previous diagnosis of genital lichen planus. Despite the heterogeneous appearance, the histological examination excluded the presence of dysplasia. Considering the side effects of the conventional corticosteroid treatment and the dimension of the lesion, we have tried to treat it with LLLT (Fig. 3). Before starting the treatment, signed informed consent was obtained. Two sessions (5 minutes each session) of LLLT using a diode laser (HELBO® TheraLite Laser, 660nm of wavelength, power 100 mW, power density 60mW/cm2, continuous mode, fiber tip area 0,17cm2) were performed. After a week, the lesion appeared more homogenous, and the erythematous areas underwent a reduction with a simultaneous reduction of symptoms. After two weeks, the lesion appeared completely healed with the disappearance of pain (Fig. 4). The follow-up continued for the other four months, and no relapse was reported (Fig. 5). In addition, no adverse effects were observed during the study.
3. DISCUSSION
This study described the successful treatment of a big lesion of erosive Oral Lichen Planus. The gold standard for the treatment of OLP is corticosteroids drugs [14]. However, many side effects were described using these drugs as opportunistic infections, impairing the hypothalamic-pituitary-adrenal axis, mucous atrophy and increasing blood pressure [24]. Sides effects are common in long-lasting treatments (e.g., for extensive lesions) and when the drug is administered systemically. A more recent approach consists of the use of LLLT, to avoid systemic drug therapy collateral events. Different parameters were described for LLLT. As stated in a recent systematic review [20], lasers used for this oral pathology had very different parameters: wavelength 630 to 970 nm, power output from 10 mW to 3 W, laser energy from 0.3 up to 6 J/cm2, power density between 10 and 1000 mW/cm. The most used type of laser was the diode laser. Reported exposure time was comprised between 5s and 8 min, and also the number of sessions varied a lot from 4 to 12 sessions. We, therefore, do not have a unique protocol for the treatment of oral lichen planus with LLLT.
However, researchers had found that LLLT could replace corticosteroids therapy for OLP [25, 19], and there are studies that have shown that LLLT, especially with diode lasers, can be very useful in preventing the extension and malignant transformation of oral potentially malignant lesions (leukoplakia and Oral lichen planus) [26].
In our case, the treatment was performed with a diode laser (HELBO® Thera Lite Laser, 660 nm wavelength, 100 mW power, 60 mW / cm2 power density, continuous mode, 0.17 cm2 fiber tip area) at power 100 mW, applied for 300s (5 min) in continuous mode, power density 60mW/cm2 in two sessions. This device has been created to perform photodynamic therapy in addition to phenotiazine chloride dye. This treatment improved the condition of the mucosa and symptoms of the patient and led to complete healing in two weeks. To our best knowledge, these parameters were not used yet for the treatment of OLP. Moreover, we needed only two sessions of LLLT to achieve complete healing of the lesion. Photodynamic therapy is a treatment in which, in addition to laser or LED light, there is the application of a photosensitizer, activated by the laser itself in the presence of oxygen, producing reactive oxygen species (ROS) and other substances that selectively affect altered cells or microorganisms. This therapy has been successfully proposed for the treatment of oral lichen planus in the literature, to even replace topical drug therapy [27, 28].
The use of the device described in this case was documented in the literature in periodontal [29], endodontic [30], orthodontic [31] field, and was also successfully used for the treatment of severe MRONJ [32], not only to perform photodynamic therapy but also for LLLT.
CONCLUSION
From the results obtained, it can also be concluded that the above method could be interesting also for OLP treatment. Using low powers, it is a safe and easy to use laser even for non-laser experts.
Currently, the main limit for the LLLT is the absence of standardization of both care and research protocols: the heterogeneity of the parameters used and the selected wavelengths, albeit in a well-defined range, in fact, prevents us from delineating the gold standard for the different LLLT applications. About clinical studies, it is important to increase the realization of long-term randomized controlled trials to improve the evidence-based approach.
LIST OF ABBREVIATIONS
| OLP | = Oral Lichen Planus |
| LLLT | = Low-Level Laser Therapy |
| ROS | = Reactive Oxygen Species |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The authors confirm that ethics approval is not required in this case report.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
The participants provided written informed involved in this study.
STANDARD FOR REPORTING
CARE guidelines and methodology were followed to conduct the study.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


