All published articles of this journal are available on ScienceDirect.
Squamous Odontogenic Tumor: Literature Review Focusing on the Radiographic Features and Differential Diagnosis
Abstract
Since its first publication in 1975, the squamous odontogenic tumor remains the rarest odontogenic lesion, with around 50 cases in the English-language literature in which the microscopic characteristics are frequently very well demonstrated. However, articles which discuss the radiographic aspects are scarce, especially with emphasis on the differential diagnosis. The present treatise proposes an assessment of jaw lesions with the same radiographic characteristics of the squamous odontogenic tumor to clarify the main findings for dental clinicians during routine diagnosis.
INTRODUCTION
Squamous odontogenic tumor (SOT) is a benign odontogenic tumor classified according to the World Health Organization (WHO) in 2005 as an epithelium odontogenic tumor with around 50 cases reported in the English-language literature at this time [1-3]. This rare entity was described for the first time in 1975 by Pullon et al. [4]; before this it was considered as an atipic acantomatous ameloblastoma or a squamous cell carcinoma. The pathogenesis of SOT is still unclear in which remnants of dental lamina (rests of Serres), epithelial rests of Malassez or gingival epithelium are the main suspected origin [2, 4]. The SOT presents well-defined histopathological aspects and previous studies discussed these aspects [3, 5] in which islands of squamous epithelium in a dense fibrous connective tissue stroma are the classical microscopic findings. Nevertheless, there are scarce articles that described radiographic features of SOT [6], and only one author included SOT in a list of possible diagnosis before the histopathological examination [7]. Therefore, we propose to discuss these aspects based on the clinical relevance of differential diagnosis with other lesions more frequently found in routine jaw radiographies.
LITERATURE REVIEW
Clinically, SOT can be presented as an asymptomatic, slow growing, intrabony lesion with few clinical signs and symptoms. Nevertheless, mobility and displacement of teeth, swelling of alveolar process, and mild to moderate pain are the main findings [2, 6, 8]. SOT occurs on average in the fourth decade of life with a slight predilection for males [2]. An equal distribution between maxilla and mandible with preference for posterior mandible and anterior maxilla is observed [2, 9]. Commonly, it is a central lesion with few cases occurring as peripheral lesions [3]. The most typical presentation of SOT detected in routine intraoral radiographs is an unilocular radiolucent defect with triangular or semicircular shape between or along the roots of adjacent vital teeth [3, 6-9]. Fig. (1) showed an interproximal lesion with these radiographic aspects. In these cases, a careful evaluation of all lesions found in the periodontal region should be performed, especially when a interproximal bone loss involves only one isolated area [7, 8]. This affirmation can be confirmed due to slow growing of SOT within a periodontal location, mimicking severe periodontal bone loss in a significant number of previous cases described in the English-language literature [2, 4, 6, 7, 9-20].
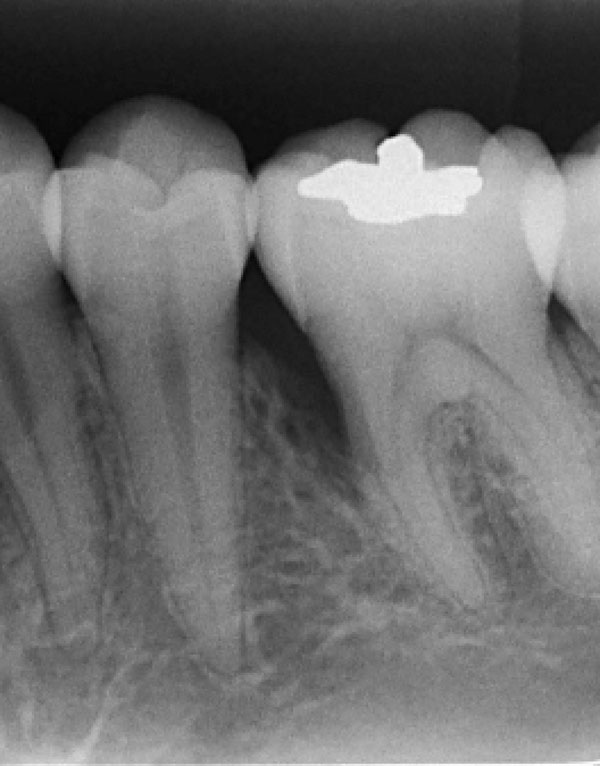
Periapical radiography showed an unilocular radiolucent defect with triangular shape between the roots of inferior left second pre molar and the inferior left first molar. A located periodontal bone loss is the main differential diagnosis of SOT.
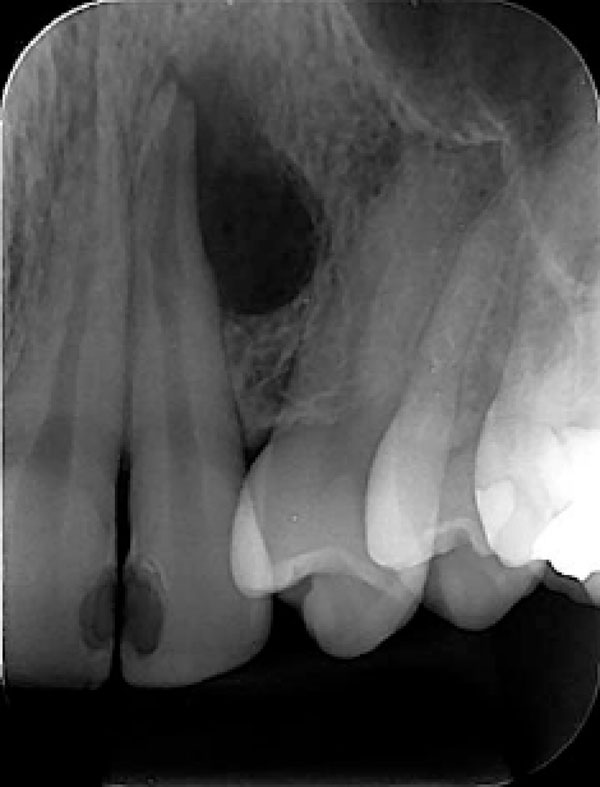
Periapical radiography showed an unilocular periradicular radiolucent defect associated with superior right central incisor. Although rare the SOT diagnosis also should be included.
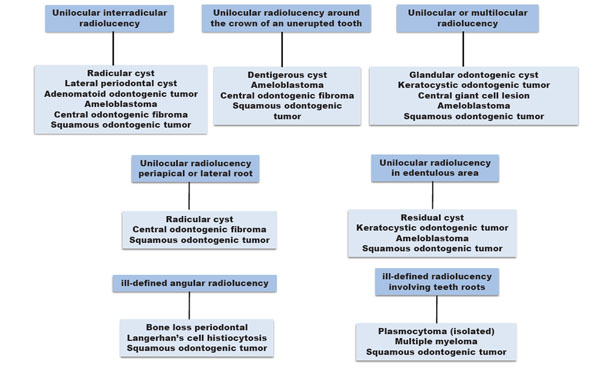
Schematic chart showing the differential diagnosis of SOT based on radiographic aspects.
SOT can also present radiographic aspects that resemble odontogenic and non odontogenic lesions as cysts and tumors with emphasis on extensive lesions with unilocular or multilocular appearance involving the mandible and/or maxilla, pushing the maxillary sinus or in association with an impacted tooth [21]. A broad list of possible diagnoses include developmental or noninflammatory odontogenic cysts, such as lateral periodontal cyst, dentigerous cyst and glandular odontogenic cyst; inflammatory odontogenic cysts, such as radicular and residual cyst; odontogenic tumors, such as keratocystic odontogenic tumor, adenomatoid odontogenic tumor, central odontogenic fibroma, unicystic and multicystic ameloblastoma; hematological disorders, such as Langerhan’s cell histiocytosis and multiple myeloma and bone pathology, such as central giant cell lesion and metastasis.
Lateral periodontal cyst (LPC) is an uncommon developmental odontogenic cyst that occurs in the adjacent or lateral area of a vital tooth [22]. LPC is asymptomatic and found in the incisor-canine-premolar region, especially in mandible, during a routine radiological examination [22-24]. A radiolucent interradicular triangular lesion associated or not with displacement of the teeth root and with sclerotic borders is the classical radiography aspect [24]. SOT can arise in the same area and also present characteristic circumscription with frequent root divergence; however, the margin may or may not be corticated as in LPC. Of all cases reviewed for SOT, at least 8 previous cases present similar aspects of LPC [2, 4, 7, 9, 10, 16, 17, 25] and considering radiological aspects, SOT should be included as a differential diagnosis of LPC.
Dentigerous cyst (DC) is the most common developmental odontogenic cyst arising from the crowns of unerupted teeth in mandible and maxilla [26]. Mandibular third molars and maxillary canines are the most often involved teeth, followed by the mandibular premolars and the maxillary third molars [26, 27]. The classical radiographic aspect of DC appears as a well-defined unilocular radiolucent with sclerotic borders associated with the crown of an unerupted tooth [26-28]. Some cases of SOT also presented similar aspects to DC and involved mandible and maxillary third molars [4, 29-32]. Moreover, both lesions can be found only in routine radiographic examination [1,4, 26-32]. Glandular odontogenic cyst (GOC) is a rare developmental odontogenic cyst with aggressive behavior that frequently involves the anterior mandible [33]. GOC is now well accepted being odontogenic origin; however, it presents glandular or salivary features as mucus cells and ductal structures [33, 34]. An extensive unilocular or multilocular radiolucent lesion with well-defined scalloped borders is a common finding in radiographic exams [33]. Tatemoto et al. in 1989 described a case of SOT presenting as radiolucency in the apical area of the vital mandibular central incisors in which the differential diagnosis of GOC was considered [25].
Inflammatory odontogenic cysts such as radicular cyst and lateral radicular cyst are the most common jaw cysts [34]. These lesions are derived from odontogenic ephitelium stimulated by inflammatory process primarily caused by root canal infection [34, 35]. Radiographic examination shows a circular or ovoid radiolucent lesion with sclerotic borders and, frequently, associated with destruction of periradicular tissues and loss of lamina dura [36]. A lesion located near periapical or lateral region superimposed on the root completes the classical radiographic findings [35, 36]. SOT occurring in the same circumstances was described by at least 14 authors [4, 5, 7, 10-14, 16-18, 22, 37, 38]. Fig. (2) showed a radiolucent periradicular lesion with similar findings. Residual cyst (RC) is considered a retained radicular cyst from one tooth that was previously removed [34]. A radiolucent lesion usually asymptomatic involving an edentulous area, and discovered during a routine radiographic examination is the main aspect of RC [39]. One author described a case of SOT with radiographic characteristics of a residual cyst [14].
Keratocystic odontogenic tumor (KOT) is a benign odontogenic lesion with aggressive and infiltrative behavior that frequently appears in the posterior mandible areas; however, it can affect any site of the jaws [40]. Radiographically, KOT presents as a well or poorly circumscribed uni- or multilocular radiolucent lesion with variable sizes and shapes [40] and mimicking several jaw lesions including SOT. Thirteen authors presented SOT cases in which KOT should be mentioned as a highly suspicious differential diagnosis [4, 10, 13, 16-18, 25, 38, 41-45].
Adenomatoid odontogenic tumor (AOT) is an epithelial odontogenic tumor with slow and progressive growth that commonly involves the anterior portion of maxilla; however, anterior portions of mandible can also be affected [46]. The follicular AOT is the most frequent type and is associated with a crown and root of an unerupted tooth, especially canines. Extrafollicular AOT is not associated with teeth and it can be found between the roots of erupted teeth. An asymptomatic well-defined unilocular radiolucent lesion with or without radiopaque foci, eventual teeth displacement, and cortical expansion is the radiographic aspect of intraosseous AOT [46]. SOT lesions can show similar findings to follicular and extrafollicular AOT [4, 9, 10, 18, 47].
Central odontogenic fibroma (COT) is a rare odontogenic tumor with benign behavior and classified as a fibroblastic neoplasm that contains a wide amount of inactive odontogenic epithelium [1, 48]. COT presents as a slow and progressive lesion found in maxilla and mandible involving frequently periradicular region [48, 49]. Favia et al. 1997 described a case of SOT involving the apex of a first superior molar resembling this frequent radiographic appearance of COT [38]. However, some lesions can be found as a nonspecific well-defined unilocular radiolucency between erupted teeth causing root displacement or become associated with the crown of a unerupted tooth [48, 49]. In these cases, LPC, DC and ameloblastomas are some lesions that should be included as differential diagnosis of COT and, therefore, also of SOT[2, 4, 8, 9-11,16, 17, 25, 29-32, 50, 51].
Ameloblastoma is a benign epithelial odontogenic tumor with two quite different intraosseous biologic variants [52]. The multicystic ameloblastoma (MA) is the most frequent type presenting aggressive and destructive characteristics with the involvement of posterior areas of jaws and impacted third molars in some cases [53]. Radiographically, MA shows as a radiolucent multilocular lesion with a ‘‘soap-bubbles” aspect associated with expansion and disruption of bone cortical [52, 53]. A unicistic ameloblastoma (UA) is less aggressive and commonly mimics odontogenic cysts frequently related with teeth in the area, especially, mandible third molars. A well-defined unilocular radiolucent lesion is the classical radiographic finding of the UA [52, 53]. Eleven cases of SOT were described with aspects that resemble uni- or multicystic ameloblastomas variants [2, 7-9, 11, 16, 17, 25, 38, 50, 51].
Langerhan’s cell histiocytosis (LCH) involves a rare group of hematological disorders originating from Langerhans cells that may affect the oral cavity [54]. Periodontal tissues are frequently involved and appear as located or generalized angular bone loss mimicking radiographic characteristics of an advanced periodontitis, such also is found in SOT [2, 4, 6, 7, 9-20, 54, 55]. Therefore, LCH and SOT should be considered as differential diagnosis when a severe periodontitis is present in the x-ray findings and no improvement is reached after periodontal treatment.
Multiple myeloma is a hematologic malignancy characterized by proliferation of plasma cells and nonfunctional monoclonal immunoglobulin in which medullary involvement through radiolucent osteolytic lesions is the most frequent presentation [56]. Nevertheless, a localized ill-defined radiolucency involving roots of teeth with lamina dura loss is also found in solitary plasmacytomas, and these myelomatous lesions could be misdiagnosed as periodontitis [56]. Thus, considering that the main radiographic aspect of SOT also mimics severe periodontitis, it should be included as a differential diagnosis of multiple myeloma and solitary plasmacytoma [2, 4, 7, 9, 11-16, 30, 41, 42, 50, 51].
Central giant cell lesion (CGCL) is considered a benign jaw lesion composed of osteoclast-like giant cells and commonly found in the mandible [57]. CGCL is more accepted as a reactive lesion presenting aggressive and non-aggressive behavior. The radiographic presentation is a well-defined non-corticated unilocular radiolucency in the small lesions until a multilocular aspect associated with ondulate septae in the bigger cases [57]. Some authors described SOT cases with x-ray findings suggestive of CGCL [2, 4, 8-14, 16, 25, 41, 42, 50, 51, 58, 59]. Finally, distant metastasis affecting oral cavity is quite uncommon; however, it can involve soft and bone tissues and requires a careful diagnostic process [60]. An osteolytic radiolucent lesion with irregular borders mimicks other jaw pathologies, since severe periodontitis until tumor process is the most frequent radiographic characteristic [60]. SOT also presents the same wide and unspecific possibility of radiographic findings and, therefore, it should also be included in a list of differential diagnosis of metastatic lesions of the jaws [2, 4-20, 25, 32, 38, 51].
CONCLUSION
Although, all SOT cases in the literature present histopathological aspects which are well described, the variety of radiography findings of SOT mimicking odontogenic and non odontogenic jaw lesions is not well elucidated. Given the limitations of our approach, a review of the main radiographic presentations of SOT was proposed as a clinical diagnosis exercise for practicing clinicians.
This paper suggested a scheme to enhance the differential diagnosis hypotheses considering the routine image findings. Thus, this concise approach can help the clinicians to outline feasible diagnostic possibilities in front of the wide spectrum of odontogenic and non-odontogenic lesions. Fig. (3) showed a schematic chart based on the radiographic aspects of SOT. Nevertheless, due to the rarity of SOT and range of radiographic aspects for this entity, a careful microscopic examination should be performed before definitive diagnosis can be reached.
CONFLICT OF INTEREST
The authors confirm that this article content has no conflict of interest.
ACKNOWLEDGEMENTS
Declared none.


