All published articles of this journal are available on ScienceDirect.
Study of the Effect of the Resin Matrix Type of Glass Fiber Posts on their Retention Within the Root Canal “An In Vitro Study”
Abstract
Introduction
The restoration of endodontically treated teeth relies heavily on the retention strength of fiber posts, which is influenced by their resin matrix composition. Epoxy and Bis-GMA are the most common matrices used in glass fiber posts, but their comparative performance remains debated. This study aims to compare two types of resin matrices used in glass fiber posts in terms of their effect on post retention within the root canal.
Materials and Methods
Twenty freshly extracted lower premolars were collected, and their coronal portions were sectioned 1 mm above the cementoenamel junction. Endodontic treatment was performed on the premolars, which were then embedded in acrylic blocks. The root canals were subsequently prepared to receive the posts. The teeth were randomly divided into two groups. Group ErP: Restored with glass fiber posts containing an Epoxy resin matrix. Group BGrP: Restored with glass fiber posts containing a Bis-GMA resin matrix.
The samples were subjected to a tensile test until failure. Statistical analysis was performed using SPSS software.
Results
Epoxy-based posts exhibited significantly higher mean tensile force (203 ± 25 N) compared to Bis-GMA-based posts (173 ± 16 N). Statistical analysis (Student’s t-test) confirmed a significant difference (P = 0.007, P < 0.05), indicating superior retention for epoxy-based posts.
Discussion
The superior retention of epoxy-based posts may be attributed to their rougher surface topography, enhancing micromechanical interlocking with resin cement. These findings align with prior studies supporting epoxy-based posts for high-stress scenarios but contrast with research highlighting Bis-GMA’s pre-polymerization advantages. Variability in cementation protocols and post-surface treatments may explain discrepancies in the literature.
Conclusion
Within the study’s limitations, epoxy-based glass fiber posts demonstrated significantly higher retention strength than Bis-GMA-based posts. Epoxy-based posts are recommended for clinical cases requiring optimal retention. Further in vitro, clinical, and microscopic studies are warranted to explore additional influencing factors.
1. INTRODUCTION
Restorative dentistry focuses on the rehabilitation of teeth following endodontic or structural treatment. When a tooth undergoes a procedure, its structural integrity may be compromised, often due to pre-existing damage from carious lesions (decay) or fractures.
Treated teeth need to last for a while and function adequately; hence, one has to plan carefully when restoring a tooth. Restoring teeth after treatment is essential for recovering their strength and extending their functional lifespan. These restorations must be robust enough to ensure the tooth remains viable for as long as possible. This process is particularly challenging when the tooth has sustained extensive damage. Teeth that have undergone root canal therapy are inherently more vulnerable than vital teeth; the removal of the pulp and the subsequent alteration of the supporting structures fundamentally change their structural response to pressure [1].
The main goal of fixing a badly damaged tooth that has undergone a root canal is to prevent the remaining tooth from breaking and to replace the missing parts. The goal of restoring treated teeth is to protect the remaining dental tissues from fracture and to replace the lost tooth structure of these endodontically treated teeth [2].
Several researchers think that posts are a good idea for teeth that have undergone root canal treatment and are badly damaged. These posts help support the tooth and strengthen it. When a tooth is severely damaged after a root canal, posts and cores can help stabilize the tooth and withstand pressure [3].
People have been using fiber-reinforced resin posts a lot since 1990. This is because they look nice, do not cost a lot of money, and are flexible in dentin [4].
These posts present two primary clinical challenges. First, they often demonstrate poor adaptation to the internal morphology of the root canal, particularly in canals with oval or flared dimensions. Second, the interface frequently suffers from debonding or loss of retention between the post and the canal walls [5, 6].
To deal with these problems, people started using prefabricated posts. They coated these posts with resin, through which they could shape each post to fit the canal anatomy. This really helps the post better adapt to the canal and stay in place [7].
Significant research has focused on enhancing the properties of Glass-Ionomer Cements (GICs) to improve their mechanical strength and biocompatibility. To reinforce the material's matrix, researchers are incorporating reinforcing fillers such as nano-hydroxyapatite or zirconia, which significantly improve fracture toughness and long-term durability. Furthermore, the integration of antimicrobial agents like chitosan or silver nanoparticles provides GICs with potent antibacterial properties, effectively inhibiting secondary decay and extending the functional lifespan of the restoration.
The people who make Glass-Ionomer Cements are also making other cements, including resin-modified Glass-Ionomer Cements. They use fillers that are easy to use. This helps the Glass-Ionomer Cements last for a long time and not exceed the optimal size. The Glass-Ionomer Cements can also send out things like fluoride and ions for a long time. This is an improvement. Now we have Glass-Ionomer Cements that are better and can be used in many different ways, which is great, for fixing teeth and other difficult jobs [8].
The modern fiber posts are made up of resin materials for the part. These fiber posts are made of carbon or silica fibers that are stretched out and then put into a resin matrix that has been treated to make it stronger. Most of the fiber posts that are reinforced with fibers have a matrix made of either Epoxy resin or Bis-GMA resin. They also have some other materials added to them [9-12].
The way carbon fiber posts look in ceramic restorations is not very nice. So people made translucent silica fiber posts that look like teeth.
These restorations, categorized as quartz or glass fiber-reinforced resin posts, are engineered to offer biocompatibility levels comparable to carbon fiber alternatives. Depending on the desired mechanical and aesthetic outcomes, these posts may incorporate E-glass, high-strength glass, or pure crystalline silica (quartz); the latter is specifically utilized to enhance the translucency and aesthetic integration of the restoration [11, 12]. Manufacturers also say that glass fiber posts have properties similar to those of carbon fiber posts [13].
Epoxy resins are a type of material that hardens when it is heated. Epoxy resins are used as the material in things like fiber-reinforced composites. Epoxy resins are used in many applications, such as adhesives, coatings, and medical implants. We also use resins in things like electrical devices. Epoxy resins, or polyepoxides, are made by mixing an epoxide base with a polyamine hardener. Epoxy resins are often used to make the material that holds fiber posts together [14].
The development of aromatic methacrylate formulations represented a significant advancement in the evolution of dental resins, which are now extensively utilized across various clinical applications [ 15]. However, the safety profile of Bis-GMA-based materials remains a subject of concern due to the potential presence of Bisphenol A (BPA). As a known contaminant within resin core materials, BPA is recognized as an endocrine disruptor; its structural similarity to estrogen allows it to interfere with hormonal pathways, potentially triggering adverse biological reactions [16].
In the case of fiber posts, the final product is usually clean. Bis-GMA is often used as the resin in glass fiber posts. Glass fiber posts are made with Bis-GMA as the resin matrix. Studies have shown that what happens after the braces come off is the reason things go wrong [17].
Clinical reports show that when a post-and-core restoration fails, it is often because the post is not staying in place. This happens 43% of the time. On the other hand, root fracture is less common; it occurs in fewer than 16 percent of post-and-core restoration failures [18].
1.1. Research Significance and Objectives
This study aims to determine what makes glass fiber posts adhere well to the dentin in the root canal and to the cement that holds them in place. The goal is to ensure the posts remain in place for a period and that the tooth does not become damaged. This is important because it helps keep the tooth stable and working properly.
The study examines the type of resin used to bond posts to dentin and cement, whereas several studies have already shown that the type of post used in the root canal affects retention [19, 20].
This study looks at two kinds of resin that are used in glass fiber posts, which are Epoxy and Bis-GMA, to see how they affect how well the posts stay in place inside the root canal of a tooth. The study evaluates the comparative efficacy of Epoxy resin and Bis-GMA in preventing the dislodgement of endodontic posts.
2. MATERIALS AND METHODS
This study was conducted in the Department of Endodontics, Faculty of Dentistry at Tishreen University, and approved by Tishreen University (Approval No. 298, Session 56, October 4th, 2022).
This study is purely in vitro and involved no direct patient intervention or clinical trial. All teeth used were obtained from extracted teeth that were discarded following routine orthodontic treatment (specifically, premolars extracted for orthodontic purposes). This study was conducted in accordance with institutional and international ethical guidelines. All teeth used in this study were extracted premolars obtained from patients undergoing orthodontic treatment at the Department of Orthodontics, Tishreen University Dental Clinic. Teeth were collected after the extraction procedure was completed for clinical purposes, and no identifiable patient information was retained.
Recently extracted, single-rooted mandibular first premolars, removed for orthodontic reasons and free from caries or deformities, were collected. Twenty premolars with similar dimensions were selected, excluding any teeth showing more than 1 mm variation in measurements. The teeth were cleaned of periodontal ligament remnants and calculus.
The clinical crowns were sectioned 1 mm above the cementoenamel junction (CEJ), resulting in standardized root lengths averaging 15 ± 1 mm. Endodontic treatment was then performed using the Eighteeth (China) rotary system following the manufacturer’s protocol. 2.5% sodium hypochlorite (NaOCl) was used for irrigation between files. After canal preparation, a final rinse with NaOCl was performed, and the canals were dried with absorbent paper points (Metabiomed, Korea).
Obturation was completed using the single-cone technique with gutta-percha points (Metabiomed, Korea) and a eugenol-free sealer (ADSEAL, Metabiomed, Korea). The teeth were stored at 100% humidity and 37°C for 7 days. Post space was prepared using Gates Glidden drills (#2), leaving 5 mm of gutta-percha apically to accommodate a 10 mm post from the CEJ.
The teeth were randomly divided into two groups:
- Group ErP: Restored with epoxy resin-based glass fiber posts (DentinPost, Komet, Germany).
- Group BGrP: Restored with Bis-GMA resin-based glass fiber posts (everStick Post, GC Corporation, Japan).
2.1. Post Space Preparation and Cementation
2.1.1. Post Space Irrigation
The remaining canal space was irrigated with 2 mL of 17% EDTA to remove the smear layer, followed by 5 mL of distilled water and drying with paper points.
2.1.2. Post Treatment
Each post was cleaned with ethanol, dried, and coated with two layers of silane coupling agent (Ultradent, USA), then left to dry for 1 minute .
2.1.3. Post Length Verification
A rubber stopper was used to confirm a 10 mm post length from the CEJ.
2.1.4. Dentin Conditioning
- The canal was dried with paper points (avoiding desiccation).
- 37% phosphoric acid was applied for 15 seconds, rinsed for 20 seconds, and lightly dried.
- A dual-cure dentin bonding agent (Excite-FDSC, Ivoclar Vivadent) was applied to canal walls, lightly air-thinned, and excess was removed with paper points.
2.1.5. Resin Cement Application
- Dual-cure resin cement (Harvard Zirconcore, Germany) was mixed (1:1) and injected into the canal.
- The post was seated with finger pressure for 10 seconds to avoid voids.
- Excess cement was removed with a cotton brush, and light-curing was performed for 40 seconds only at the coronal end.
2.2. Embedding and Testing
- Teeth were embedded in acrylic blocks (20×20×20 mm), leaving 1 mm of root exposed to simulate bone level and evaluate failure modes.
- Samples were numbered (1–20) and stored until mechanical testing.
2.3. Tensile Resistance Testing
- A universal testing machine (Ibertest, Spain) at Tishreen University’s Faculty of Mechanical Engineering was used (Fig. 1).
- For this test, the teeth embedded in acrylic blocks were vertically secured to the base of the testing machine. The post was gripped by a fixture attached to the moving crosshead of the machine, which applied a tensile force at a rate of 1 mm/min in the vertical direction.
- Testing continued until complete post dislodgement from the root canal occurred. The maximum tensile force (in Newtons, N) required for failure was recorded for each specimen, as displayed on the machine's load-displacement graph (Fig. 2).

The tensile strength test using a universal mechanical testing machine (Ibertest, IBMU series, Spain).
The peak tensile force, as indicated in the stress-strain curve.
3. RESULTS
The tensile force (Newtons, N) was measured for each tooth in the study sample to evaluate and compare the bond strength of epoxy-based and Bis-GMA-based posts. Descriptive statistics are shown in Table 1.
| Sample Group | N | Mean (N) | SD | Max (N) | Min (N) | SEM |
|---|---|---|---|---|---|---|
| Epoxy Posts | 10 | 203 | 25 | 241 | 172 | 7.91 |
| Bis-GMA Posts | 10 | 173 | 16 | 195 | 143 | 5.29 |
The raw tensile force values for all specimens are presented in Table 2, showing the range of retention forces observed across both groups. Comparative descriptive statistics revealed that epoxy-based posts exhibited higher mean tensile force values (203 ± 25 N) than Bis-GMA-based posts (173 ± 16 N), suggesting potentially superior retention capabilities.
| Sample No. | Epoxy Group (ErP) | Sample No. | Bis-GMA Group (BGrP) |
|---|---|---|---|
| 1 | 215 N | 11 | 154 N |
| 2 | 218 N | 12 | 180 N |
| 3 | 235 N | 13 | 167 N |
| 4 | 211 N | 14 | 195 N |
| 5 | 172 N | 15 | 181 N |
| 6 | 199 N | 16 | 190 N |
| 7 | 190 N | 17 | 143 N |
| 8 | 172 N | 18 | 178 N |
| 9 | 241 N | 19 | 188 N |
| 10 | 178 N | 20 | 163 N |
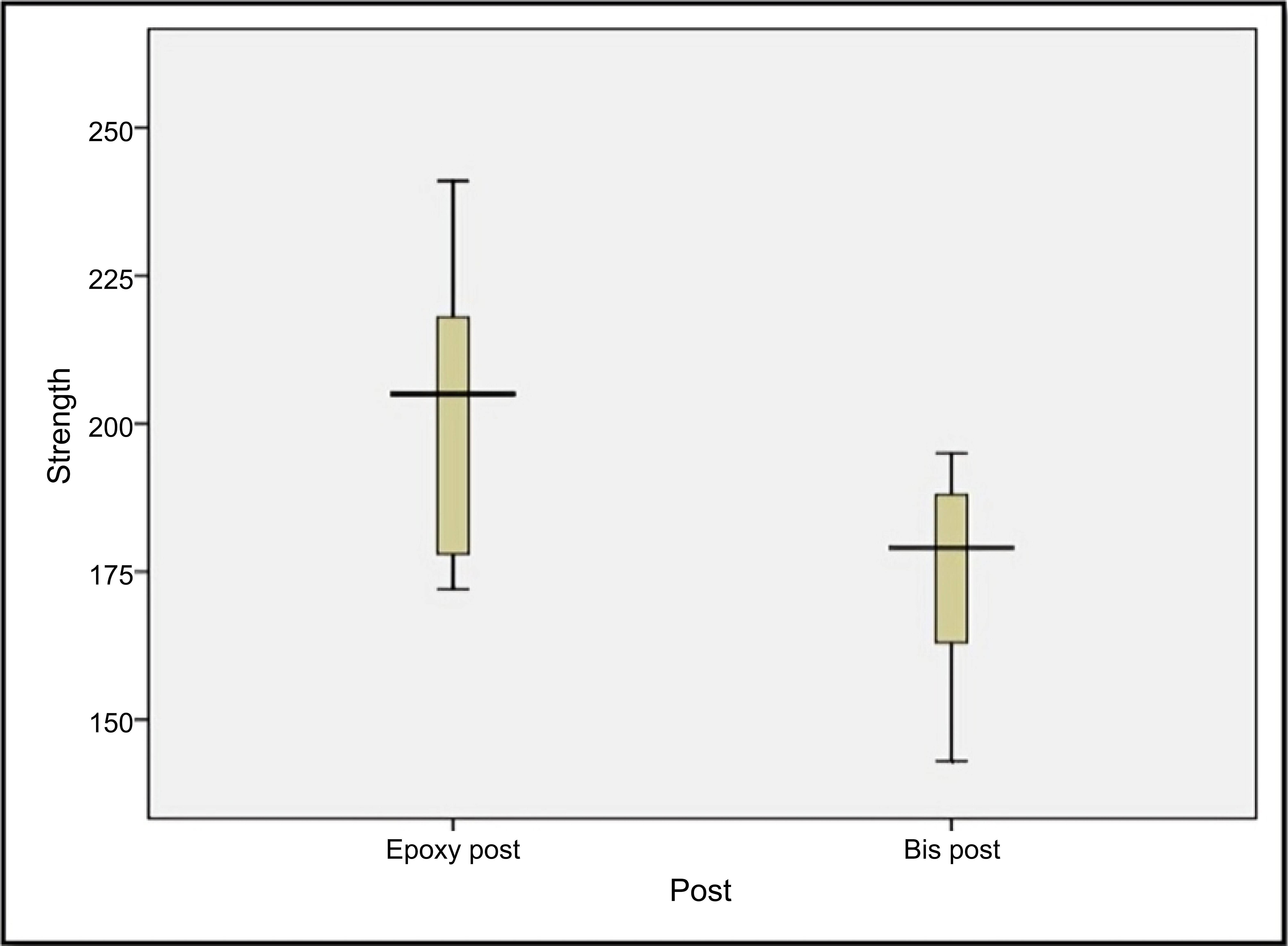
Before conducting comparative analyses, the normality of the data distributions was assessed using the Kolmogorov-Smirnov test, which indicated that both datasets followed a normal distribution (p-value > 0.05). This allowed for the use of parametric statistical tests. The distribution of tensile forces was further visualized using a box plot, which showed the median, interquartile range, and any outliers in each group.
An independent samples t-test was then performed to statistically compare the mean tensile forces between the two post systems. The results demonstrated a significant difference (p-value = 0.007), with epoxy-based posts exhibiting substantially higher bond strength than Bis-GMA-based posts (p-value < 0.05) (Table 3).
| Sample Group | N | Mean (N) | Mean Difference | 95% CI of Difference | T-value | p-value |
|---|---|---|---|---|---|---|
| Epoxy Posts | 10 | 203 | 29.2 | 9.2 – 49.2 | 3.07 | 0.007* |
| Bis-GMA Posts | 10 | 173 | - | - | - | - |
This finding is graphically represented in Fig. (3), which clearly highlights the superior retention performance of epoxy-based posts. The observed difference in tensile force suggests that epoxy-based posts may offer greater resistance to dislodgement in clinical settings, potentially making them a more reliable choice for restorative procedures.
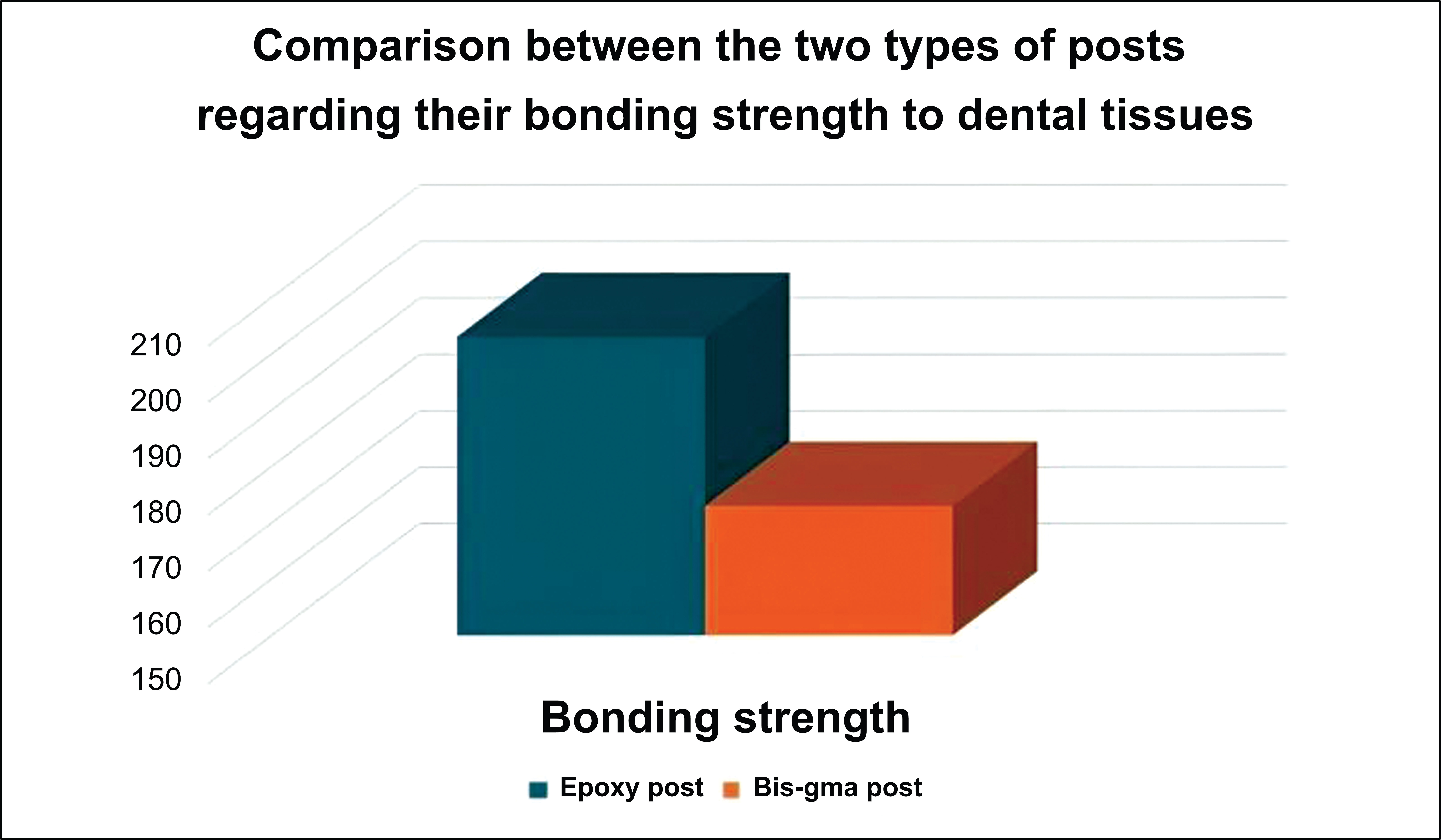
Comparison between the two types of posts regarding their bonding strength to dental tissues.
4. DISCUSSION
Restoration, particularly of endodontically treated and structurally compromised teeth, presents a clinical challenge for dentists due to the loss of essential dental properties, including pulp tissue and surrounding dentin structures [1].
The primary goals of restoring such teeth are to protect remaining dental tissues from fracture and replace lost tooth structure [2].
Consequently, many researchers have recommended the use of posts to restore endodontically treated, structurally compromised teeth and reinforce remaining dental tissues [9, 10, 21].
For this study, mandibular premolars extracted for orthodontic reasons were selected as the sample teeth. These single-rooted teeth were chosen because they are relatively easy to obtain intact (free of caries or defects) without violating research ethics. Additionally, they possess sufficient dental tissue mass to accommodate most root post systems [22].
Some clinical studies have identified premolars as the most fracture-prone teeth [23, 24], further justifying their selection for this research.
This study aimed to compare the retention strength of two types of resin matrices (Epoxy vs. Bis-GMA) in glass fiber posts within root canals. Statistical analysis revealed that Epoxy-based posts exhibited significantly higher retention than Bis-GMA-based posts. This difference can be attributed to the varied bonding mechanisms between fiber posts and resin cement, including micro-mechanical interlocking and chemical adhesion [25].
A scanning electron microscopy (SEM) study by Zicari et al. (2012) [26] found that Epoxy-based fiber posts had a rougher surface than Bis-GMA-based posts, leading to stronger bonding due to enhanced mechanical interlocking with resin cement.
Our findings align with those of Alnaqbi et al. (2018) [27], who concluded that Epoxy-based fiber posts demonstrated superior bond strength when cemented with dual-cure dimethacrylate resin cement. Similarly, Zicari et al. (2012) [26] reported that traditional glass fiber posts with an Epoxy matrix outperformed those with a Bis-GMA matrix in retention strength, attributing this to differences in surface micro-interlocking, as confirmed by microscopic examination.
However, our results contradict those of Le Bell et al. (2004) [28], who found that Bis-GMA-based fiber posts had higher bond strength than Epoxy-based posts. This discrepancy may stem from their pre-light-polymerization of Bis-GMA post surfaces for 40 seconds before cementation, allowing resin monomers to penetrate deeper into the pre-polymerized post surface [25].
To further elucidate the mechanisms behind the superior retention of epoxy-based posts, it is essential to consider the chemophysical interactions at the post-cement interface. Beyond micromechanical interlocking, the potential for chemical adhesion between the resin cement and the post's matrix is crucial. Epoxy resins possess polar hydroxyl and ether groups that may form more effective secondary bonds with the methacrylate-based resin cement. In contrast, while Bis-GMA posts are also methacrylate-based, which theoretically promises better chemical compatibility with the luting cement, their smoother surface topography, as noted in the literature [27], may limit the effective surface area for such bonding. This study's protocol, which did not include pre-polymerization of the Bis-GMA posts, likely precluded the formation of a superficial polymerized layer that could enhance monomer interdiffusion-a factor that may explain the contradictory findings reported by Le Bell et al. [28]. Therefore, the retention strength appears to be a function of a complex interplay between surface roughness (favouring epoxy posts) and the potential for chemical bonding or monomer interpenetration (which may favour Bis-GMA under specific pre-treatment conditions).
The clinical implications of these findings are substantial. Given that post debonding is a leading cause of failure [17, 18], selecting a post system with inherently higher retention, such as the epoxy-based posts in this study, could enhance the longevity of the restoration. This is particularly critical for teeth with minimal coronal structure and a reduced ferrule effect, where retention relies heavily on the post itself. The use of epoxy-based posts in such high-stress scenarios may provide a greater safety margin against catastrophic debonding. However, it is also crucial to acknowledge that the clinical performance is a sum of all parts; the choice of luting cement, adhesive protocol, and post surface treatment remain pivotal co-factor in achieving a durable bond. Future research should standardize these variables to isolate the resin-matrix effect and explore surface-treatment protocols to optimize the performance of both post types.
5. STUDY LIMITATIONS
This in vitro study has certain limitations. The laboratory setting cannot replicate complex oral conditions, such as fatigue loading or humidity. The sample size, though common, was relatively small. The use of a static tensile force does not simulate clinical masticatory stresses. Findings are also specific to the materials and protocols used; different brands or techniques might yield different results. Finally, the lack of microscopic analysis of the post surfaces or interfaces means the retention mechanism is inferred rather than directly confirmed.
CONCLUSION
Within the limitations of this in vitro study, it can be concluded that the resin matrix type significantly influences the retention strength of glass fiber posts. Epoxy-based glass fiber posts demonstrated significantly superior tensile resistance and retention within the root canal compared to Bis-GMA-based posts.
This enhanced performance is likely attributable to the distinct surface characteristics of the epoxy matrix, which promote more effective micromechanical interlocking with the resin cement.
Therefore, based on these findings, epoxy-based fiber posts are recommended for clinical cases where optimal post retention and long-term stability are paramount. Further research, including clinical trials and microscopic analyses of the post-cement-dentin interface, is warranted to validate these results and explore the influence of other clinical variables.
AUTHORS’ CONTRIBUTIONS
The authors confirm their contribution to the paper: study conception and design: T.S.: Data collection; N.S.: Analysis and interpretation of results: N.S., M.K.: Draft manuscript; N.S.: Author. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| GICs | = Glass-Ionomer Cements |
| CEJ | = Cementoenamel Junction |
| SEM | = Scanning Electron Microscopy |
ETHICAL STATEMENT
This study was conducted in the Department of Endodontics, Faculty of Dentistry at Tishreen University, Syria, (Approval No. 298, Session 56, October 4th, 2022) for the use of anonymized, discarded human teeth in this in vitro study.
CONSENT FOR PUBLICATION
Written informed consent has been taken from the patients for the use of discarded, anonymous extracted teeth in in vitro research.
AVAILABILITY OF DATA AND MATERIALS
The data that support the findings of this study are available from the corresponding author, [N.S], on special request.
ACKNOWLEDGEMENTS
We thank the participants for their cooperation and the clinical staff for their support.


