All published articles of this journal are available on ScienceDirect.
Palatogram Analysis of Complete Upper Denture Adaptation in Producing S and Z Sound: A Cohort Study
Abstract
Introduction
This study aimed to evaluate the contact area between the tongue and the intaglio surface of complete upper dentures during the production of the /s/ and /z/ phonemes using palatography. A secondary objective was to compare palatographic findings based on gender, age, and denture-wearing history.
Methods
A clinical cohort study was conducted on 40 subjects (20 males, 20 females) with complete upper dentures. Palatograms (zone A until X) were obtained by applying Pressure Indicator Paste to the dentures, instructing subjects to pronounce the ‘S’ and ‘Z’ phonemes, and photographing the resulting tongue-palate contact patterns over 60 days. Data were analyzed using t-tests.
Results
Significant differences in ‘S’ phonetics (zones B, C, F, and G) were observed across gender (p = 0.003), age groups (p = 0.024), and denture-wearing history (p < 0.001). ‘Z’ phonetics (zones F, G, N, Q, T, and W) also showed significant differences in age groups (p = 0.004) and denture-wearing history (p < 0.001). Palatographic analysis identified specific contact zones for the /s/ and /z/ phonemes, with phonetic adaptation occurring predominantly between the second and third control visits.
Discussion
Phonetic disturbances, particularly involving the sibilant sounds /s/ and /z/, frequently occur following the insertion of complete upper dentures but typically improve within two weeks due to neuromotor tongue adaptation. This study found that female patients under 60 with prior denture experience adapted more effectively, and palatogram analysis revealed specific tongue-palate contact zones critical for accurate articulation.
Conclusion
Palatography proved to be a valuable clinical tool for assessing tongue–palate contact in complete upper denture wearers, particularly for the ‘S’ and ‘Z’ phonemes. The study highlights that optimal phonetic performance is influenced by gender, age, and prior denture experience, with adaptation occurring mainly between the second and third follow-up visits. This study highlights the importance of individualized denture adjustments in enhancing speech clarity and overall patient satisfaction.
1. INTRODUCTION
Dental health is fundamental to overall health and well-being, particularly in the elderly population [1, 2]. According to data from the 2018 Indonesian Basic Health Survey (RISKESDAS), tooth loss, whether due to extraction or spontaneous loss, was the second most prevalent dental and oral health problem in Indonesia, following tooth decay and caries [3]. The national prevalence of tooth loss is 19%, with the highest rate observed in individuals over 65 years (30.6%), followed by those aged 55–64 years (29%). These figures highlight the need for preventive measures to reduce tooth loss among the elderly in Indonesia [4]. In general, the use of dentures is the primary approach to address aesthetic, masticatory, swallowing, and phonetic issues resulting from tooth loss [5-7]. RISKESDAS data indicate that 3.5% of Indonesians use partial dentures, while 1.2% use complete removable dentures (CRDs). CRDs remain the most common treatment option for complete tooth loss within the dental arch [8].
Following the insertion of maxillary complete removable dentures, patients frequently present with unclear speech or phonetic disorders. This occurs because phonetic evaluation in complete removable denture cases is rarely performed, with greater emphasis typically placed on aesthetics, masticatory function, and comfort. Consequently, one of the primary objectives of complete removable denture fabrication, restoration of phonetic function, is often not fully achieved [5, 9]. According to Rossler, approximately 18% of patients wearing removable dentures experience phonetic dysfunction, which could significantly impact social interactions [10, 11]. Furthermore, patient expectations for improved speech clarity through complete removable dentures are not always met. Optimal phonetic outcomes could be achieved by positioning denture teeth as closely as possible to their natural tooth locations. Additionally, factors, such as tooth shape, tooth size, denture base thickness, and palatal rugae configuration contribute to enhancing phonetic function [12, 13].
Patients often attribute unclear speech to the presence of a complete removable denture base that partly or completely covers the palate, thereby disrupting its role in phonetic production [14, 15]. Coverage of the incisive papilla and palatal rugae by the denture base could lead to a loss of tactile guidance and cause airflow turbulence during articulatory sound production [16]. In addition, such coverage may alter tongue movement patterns, further affecting phonetic clarity [5, 17].
A change of just 0.5 mm in the base thickness of the palatal area of the anterior teeth can lead to phonetic disturbances, particularly with sibilant sounds such as ‘S’ and ‘Z’. Palmer’s study indicates that, among complete removable denture (CRD) wearers, the most frequent pronunciation difficulties occur with these sibilant sounds due to the contour of the anterior palatal area. To address this issue, adjusting the palatal contour in the region contacting the tongue is essential to promote easier adaptation and improve speech clarity. The area of the palate contacted by the tongue during speech could be assessed using a palatogram, which records the pattern of tongue–palate contact during phonation [18, 19].
The Indonesian Palatogram Gold Standard for the pronunciation of linguo-palatal consonants was developed by Dewita et al. [20] and serves as a reference for addressing phonetic disorders, particularly in patients using maxillary complete dentures [21]. Adaptation to maxillary complete removable dentures—specifically the ability to articulate linguo-palatal consonants—varies widely among individuals, with some never achieving full adaptation. Given this variability, the present study aimed to develop a new method for assessing the adaptability of maxillary complete removable denture users based on the Indonesian Palatogram Gold Standard for the letters ‘S’ and ‘Z’. This method evaluates the tongue–intaglio denture contact area involved in producing these sibilant sounds, measured through palatography.
2. MATERIALS AND METHODS
This clinical cohort study (2020-2021) involved subjects who were complete upper denture wearers. Informed consent was obtained from all participants prior to the commencement of the study. Ethical clearance was obtained from the Ethical Committee, Faculty of Dentistry, Universitas Indonesia, No. 72/Ethical Clearance/FKGUI/XI/2011.
2.1. Subject Recruitment
Subjects were recruited at the Dental Hospital, Universitas Indonesia, Jakarta, Indonesia, regardless of age or gender. Eligible participants were complete denture wearers with normal occlusion and jaw relationships, verified through clinical and radiographic examinations. Inclusion criteria also required the absence of cognitive impairments, mental disabilities, speech disorders, or articulation impairments, as confirmed by a certified prosthodontics, as well as the absence of neuromuscular disorders affecting orofacial muscle function, oral motor control, or tongue-palate contact during speech. Subjects with partial tooth loss or wearing partial dentures were excluded. Sample size was calculated using Eq. (1) [22]:
 |
(1) |
N: Total sample.
Zα: The z-score corresponding to the type I error rate. Zα = 1.96.
Zβ: The z-score corresponding to the type II error rate. Zβ = 0.84.
S: The standard deviation of the population or the estimated standard deviation from the sample. S = 4.
X1-X2: The minimum mean difference considered clinically meaningful (X1-X2 = 2).
2.2. Pressure Zone Evaluation
The thickness of the anterior palatal base was measured within a range of 1.5 to 2.5 mm [23]. Pressure Indicator Paste (P.I.P.) was then evenly applied to the palatal surface of the maxillary complete removable denture using a brush, with strokes directed from anterior to posterior. Lemon juice solution was used as a cleanser for any remaining P.I.P. material.
After the application, the complete removable denture was inserted into the oral cavity, and each subject was instructed to pronounce the sibilant sounds ‘S’ and ‘Z’ to produce a palatal contact pattern. The complete removable denture was then carefully removed from the mouth. In the case of maxillary removable dentures, removal was performed without touching the palatal surface to avoid erasing the palatogram result due to direct contact with the fingers. A score of 0 was assigned if less than 50% of the P.I.P. in the polished surface contact area was worn away. A score of 1 was assigned if more than 50% of the P.I.P. in the polished surface contact area was worn away after the patient articulated the sounds ‘S’ or ‘Z’ one time, while wearing the upper complete denture. The scoring was conducted by three researchers (NF, HK, O), and in the event of a disagreement, a third person provided a score. The majority vote was determined as the final score. This technique was adapted from Andries et al. (Fig. 1A-C) [21].
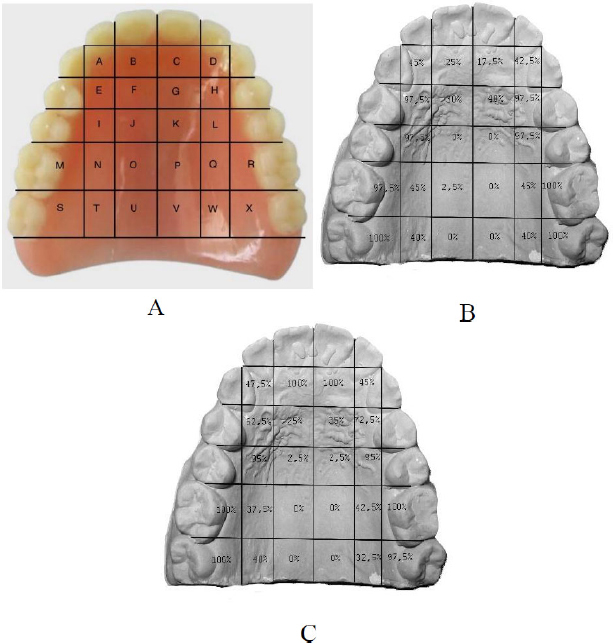
(A) Division of phonetic zones on the complete upper denture; (B) Standardized percentage for each zone for ‘S’ sound; (C) ‘Z’ sound.
2.3. Palatogram Evaluation
The resulting palatogram was documented using a Canon PowerShot A2200 digital camera (Canon Inc., Japan) with a resolution of 14.1 megapixels. Photos were taken from a perpendicular distance of 20 cm from the object. This documentation aimed to ensure that the images could be further processed using Adobe Photoshop CS5 software (Adobe Systems Incorporated, United States) (Fig. 1).
The photo processing was carried out using Adobe Photoshop to obtain data that could be analyzed both quantitatively and qualitatively for each subject. Examination and documentation of palatogram results were carried out periodically—at the time of appliance insertion, then during the first control (1–2 days after insertion), second control (3–5 days after insertion), third control (10–14 days after insertion), fourth control (30 days after insertion), and fifth control (60 days after insertion).
3. RESULTS
This study obtained 40 subjects (M: F = 1:1) with an age group <60 years old, about 52.5% (Table 1). Table 2 shows a comparison of the mean percentage for each variable. Based on the mean percentage for phonetics ‘S’, there was a significant difference in gender (p =0.003), age group (p =0.024), and history of complete upper denture (CUD) wearer (p <0.001). For phonetics ‘Z’, there was a significant difference in age group (p =0.004) and history of CUD wearer (p <0.001).
As shown in Table 1, a total of 21 participants were under the age of 60. The distribution of participants based on gender (female and male) and prior experience with complete removable dentures usage (experienced and inexperienced) was evenly balanced, with 20 individuals in each respective category.
| Variable | n (%) |
|---|---|
| Gender | - |
| Male | 20 (50) |
| Female | 20 (50) |
| Age group | - |
| <60 yo | 21 (52.5) |
| >60 yo | 19 (47.5) |
| History CUD | - |
| Yes | 20 (50) |
Table 2 shows a comparison of the mean values of ‘S’ and ‘Z’ phonetics based on several variables. For the production of the phoneme 'S', a statistically significant difference was observed based on gender, where females showed a higher mean value (955.45 ± 63.66) than males (880.00 ± 87.19) (p = 0.003). A significant difference was also found based on age groups, with participants under 60 years showing a higher mean value (946.03 ± 80.95) compared to those aged 60 and above (886.44 ± 78.84) (p = 0.024). In addition, a highly significant difference was observed in relation to the history of denture use, where experienced users had a higher mean value (964.93 ± 72.88) than inexperienced users (870.52 ± 68.17) (p < 0.001).
For the production of the phoneme 'Z', a significant difference was found between age groups, with subjects under 60 years showing a higher mean value (1,010.39 ± 87.57) compared to those over 60 years (921.62 ± 96.55) (p = 0.004). Prior experience with complete removable dentures also showed a highly significant difference, where experienced users demonstrated a higher mean value (1,031.08 ± 83.95) compared to those with no prior experience (905.37 ± 75.33) (p < 0.001). Although the mean value for females (999.39 ± 93.28) was higher than that of males (937.06 ± 101.46), the difference was close to but did not reach statistical significance (p = 0.05).
| Variable | Phonetics | |||
|---|---|---|---|---|
| ‘S’ | p-value | ‘Z’ | p-value | |
| x̄ (SD) | x̄ (SD) | |||
| Gender | - | 0.003** | - | 0.05 |
| Male | 880.00 (87.19) | 937.06 (101.46) | ||
| Female | 955.45 (63.66) | 999.39 (93.28) | ||
| Age | - | 0.024* | - | 0.004** |
| <60 yo | 946.03 (80.95) | 1010.39 (87.57) | ||
| >60 yo | 886.44 (78.84) | 921.62 (96.55) | ||
| History CUD | - | <0.001** | - | <0.001** |
| Yes | 964.93 (72.88) | 1031.08 (83.95) | ||
| No | 870.52 (68.17) | 905.37 (75.33) | ||
In addition to the statistical analysis of phonetic adaptation, a visual evaluation through palatograms was conducted to identify the pattern of tongue contact with the palate during the pronunciation of the phonemes 'S' and 'Z' (Fig. 2). As shown in Fig. (1), the phoneme 'S' shows predominant contact areas in zones B, C, F, and G, while the phoneme 'Z' showed a wider distribution across zones F, G, N, Q, T, and W. Zones marked in red indicated areas of excessive pressure, indicating the need for denture base thinning in those areas to support clearer articulation. In observation, the most noticeable phonetic adaptation occurred during the second (C2) and third (C3) controls, indicating a critical period in the neuromuscular adjustment process to the prosthesis.
Figure 2 shows the mean percentage for ‘S’ and ‘Z’ phonetics. For ‘S’ phonetics, the critical areas were B, C, F, and G; meanwhile, for ‘Z’ phonetics, the critical areas were F, G, N, Q, T, and W. The color indicates that a thin basis is recommended based on these zones. Physiological adaptations were observed at C2 and C3.
Figure 2 depicts the mapping of tongue-to-palate contact based on palatograms during the pronunciation of the phonemes 'S' and 'Z', from the initial insertion of the acrylic denture up to the fifth control visit. Red colored letters indicate areas of excessive pressure where relief or thinning of the denture base is needed to improve articulation. For the phoneme 'S', dominant contact occurred in zones B, C, F, and G; whereas for the phoneme 'Z', a broader contact pattern was observed, covering zones F, G, N, Q, T, and W. Phonetic adaptation became noticeably significant during the second and third control sessions (C2 and C3).
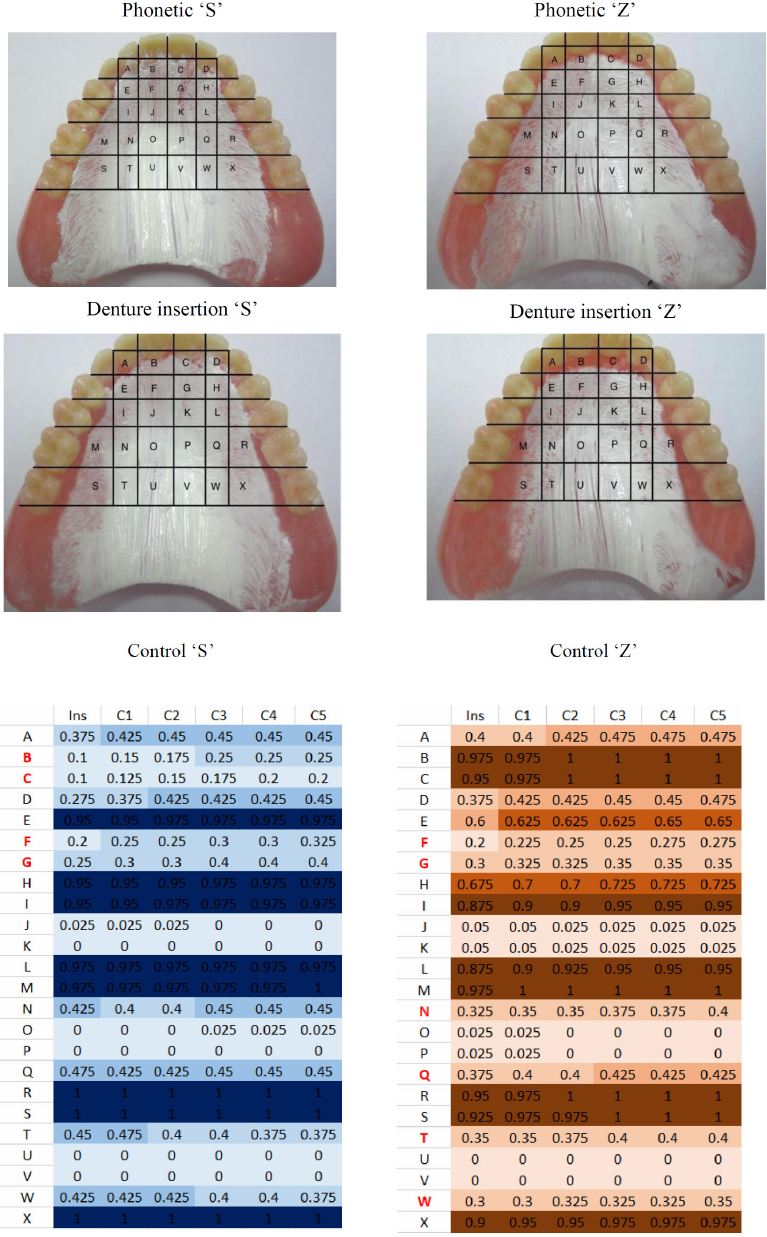
Confusion matrix of phonectis ‘S’ and ‘Z’. Ins Denture insertion; C1 Control 1st; C2 Control 2nd; C3 Control 3rd; C4 Control 4th; C5 Control 5th. Red color indicates that the basis of the denture should be relieved.
4. DISCUSSION
Phonetic problems often arise after the insertion of removable dentures, both in new denture wearers and in patients who have previously worn dentures [24]. A new denture will inevitably affect phonetic function. However, this typically lasts only a few weeks, as the tongue has a high capacity for adaptation [25]. Phonetic disturbances after the insertion of complete dentures can arise from the palatal coverage of the denture base, which disrupts tongue-palate contact essential for the precise articulation of sibilant sounds, such as ‘S’ and ‘Z’. This phenomenon aligns with the observations of Meira et al. [26], who demonstrated that modifications in palatal contour and thickness, whether in removable complete dentures or implant-supported prostheses, can alter speech patterns, particularly for consonants that depend on accurate linguopalatal contact [9].
As shown in Table 1, all subjects had a complete upper denture, with a similar proportion by gender (50% vs 50%) and age groups (52.5% vs 47.5%). About 50% of subjects had a history of using a complete upper denture. All upper denture prosthesis were applied with pressure indicator paste as shown in Fig. (2). Next, the complete denture was tried in the mouth, and the patient was instructed to pronounce the letters 'S' and 'Z'.
This study demonstrates a statistically significant difference in phonetic adaptation among patients who use complete dentures, particularly in the linguo-palatal phonetic pronunciation of the sounds ‘S’ and ‘Z’, when comparing factors, such as gender, age group, and history of denture use (Table 2). Female subjects under the age of 60 with prior experience wearing complete removable dentures were found to adapt better to the phonetic articulation of the letters ‘S’ and ‘Z’.
Several factors affect the goal of optimal sound production, including internal factors (such as patient’s tongue physiology, mental attitude toward wearing removable dentures, ability to adapt) and external factors (such as the correct determination of vertical occlusal dimension, proper arrangement of anterior and posterior teeth based on aesthetics and function, well-contoured palatal polished surfaces) [18, 27].
Each individual has a different tongue physiology, but the neural induction is the same. A functional magnetic resonance imaging (fMRI) study by Inamochi et al. [28] demonstrated that individuals experience tongue motor impairment immediately after the insertion of a palatal plate, indicating an initial disruption in the oral neuromotor control system. However, after seven days, there was a significant improvement in tongue motor skills, objectively marked by decreased activity in brain areas, such as the angular gyrus and precuneus. These findings suggest that the central nervous system begins to adapt to the altered intraoral environment through mechanisms of neuroplasticity. Therefore, neuromotor adaptation of the tongue to the presence of a denture could occur within a physiological timeframe of approximately one week, particularly in individuals with intact neurological function [28].
During speech in oral conditions, the articulation of the ‘S’ and ‘Z’ sounds is achieved when the soft palate and uvula are raised, the lateral edges and tip of the tongue are pressed close to the alveolar ridge, the anterior teeth are approximated, and the mouth is not opened wide, narrowing the air passage to prevent nasal airflow and direct it orally. However, tongue-palate contact patterns vary between individuals; they consistently follow a referential pattern [29]. The clarity of sibilant letter articulation, particularly the phonemes /s/ and /z/, is highly dependent on the precise contact relationship between the tongue and the palatal contour. In complete denture prosthodontics, the palatal portion of the maxillary denture base plays a crucial role in shaping the resonant characteristics of the oral cavity as well as the overall articulatory function [30, 31]. Consonant sounds can be classified based on the technique and place of articulation, which involve efforts to obstruct the flow of expiratory air by the articulators before releasing it. Based on these criteria, consonant sounds can be devided into: 1) plosive consonants: /t/, /d/, /p/, /b/, /k/, /g/; 2) fricative consonants: /f/, /v/, /θ/, /ð/, /s/, /z/, /ʃ/, /ʒ/, and /h/; 3) affricate consonants: /tʃ/, /dʒ/; 4) semivowel consonants: /r/, /l/; and 5) nasal consonants: /n/, /m/, /ŋ/; and 6) glide consonants: /w/, /j/, /hw/ [30]. The term sibilant is applied to any sound that resembles the 'S' sound, including /s/ and /z/. Misarticulation of sibilant sounds is referred to as lisping or sigmatism [12].
The reference for the Indonesian language has been studied by Dewita et. al. [20], who established the standard gold palatogram for linguo-palatal consonants in Indonesians. It has been noted that, in the analysis of palatograms, the primary consideration is the consistency of contact patterns or positions observed during the articulation of the same consonant. As defined in the Glossary of Prosthodontic Terms, a palatogram is a representation depicting the area of the palate that comes into contact with the tongue during a specific activity, most commonly during phonetic articulation [17, 32]. The function of a palatogram is to evaluate phonetic disorders in patients who use removable dentures, in individuals with cleft palates, or as a tool for speech pathologists working with patients with speech disorders [20]. This study focuses specifically on the letters ‘S’ and ‘Z’ because, according to Palmer's research, pronunciation difficulties commonly encountered are related to the use of complete removable dentures in the anterior palatal contour area, which is associated with the pronunciation of the sibilant sounds ‘S’ and ‘Z’ [12].
Figure 2 shows the palatogram analysis, providing a complete visualization of the contact patterns between the tongue and the palate during articulation. The phoneme ‘S’ showed dominant contact in the anterior palatal zones, specifically B, C, F, and G. In contrast, the phoneme ‘Z’ involved a broader area, including zones F, G, N, Q, T, and W. The red areas on the palatogram indicate regions of excessive contact pressure, particularly from the time of denture insertion to the second follow-up. These areas should be relieved (by grinding or adjustment) on the polished surface of the denture base to support more optimal articulation [18].
In terms of adaptation, our study showed that all subjects were able to adapt in around two weeks (Fig. 2). Based on Inamochi et al's [28] study, improved phonetic adaptation was observed during the second (days 3–5) and third (days 10–14) controls, indicating a phase of tongue adaptation to the presence of a denture [28, 32]. These findings highlight the importance of continuous phonetic evaluation during the post-insertion period, as well as the need for visual-based interventions, such as palatograms, to support more individualized and functional prosthesis modifications [33].
For external factors, clinicians should carefully evaluate the thickness of the denture. Various studies and clinical experiences showed that the ideal thickness of the palatal base in the anterior area, especially around the palatine rugae region, ranges from 1.5 mm to 2.0 mm. This thickness is considered to provide adequate space for the tongue to form a narrow airway required in fricative sounds. A thickness exceeding 2.5 mm tends to interfere with tongue movement and may lead to phonetic distortion, such as the pronunciation of ‘S’ shifting to /ʃ/ (as in the word “sapa” sounding like “syapa”) [34, 35]. Even minimal changes (as small as 0.5 mm) in the anterior palatal contour and denture base thickness can impair airflow and tactile guidance, affecting sibilant sound production, thereby underscoring the palatogram’s role as both a diagnostic and clinical tool for evaluating and adjusting palatal morphology during complete denture fabrication or modification. If a patient exhibits unclear articulation of the ‘S’ and ‘Z’ phonemes after the insertion of a maxillary complete denture, a structured phonetic evaluation is necessary. The patient can be asked to repeatedly pronounce words containing sibilant sounds, such as “sebelas” and “zebra.” If any distortion is detected, selective reduction of the palatal base becomes a mandatory procedure [30].
Another approach for assessing denture thickness is Electropalatography (EPG) [36]. EPG enables the real-time recording of tongue–hard palate contact patterns during speech through a custom-fitted artificial palate embedded with electrodes. This method is considered relatively simple, cost-effective, and clinically convenient, as palatograms are widely utilized in prosthetic dentistry and speech assessment. It requires only basic materials, such as a Fletcher’s compound, eugenol, and a brush, to visually map tongue–palate contact during articulation, allowing for rapid chairside application on trial or processed dentures. However, the use of EPG has notable limitations, including its high equipment cost, complex setup procedures, and the potential to interfere with natural speech dynamics [37].
5. STUDY LIMITATIONS AND FUTURE RECOMMENDATIONS
This study had several limitations. One notable limitation was the insufficient consideration of accent variations, which may be influenced by participants’ language, ethnic backgrounds, and the shape of the palatum. Furthermore, the palatography method presents inherent constraints, as it is limited to detecting and analyzing the articulation of linguo-palatal consonants. Consequently, its utility is restricted to evaluating phonetic disturbances involving this specific consonant group. In the present study, the analysis was confined to the phonemes ‘S’ and ‘Z’; therefore, further investigations are warranted to assess other linguo-palatal consonants. In addition, future research should also address the articulation of non-linguo-palatal consonants, including the development of appropriate diagnostic tools for their assessment. Moreover, this study did not evaluate the mental attitude of the participant and the correct determination of the vertical occlusal dimension, as well as the proper arrangement of anterior and posterior teeth.
CONCLUSION
Phonetic disturbances following the insertion of maxillary complete dentures, particularly affecting the sibilant sounds ‘S’ and ‘Z’, are common but generally transient, typically resolving within one to two weeks through neuromotor adaptation of the tongue. This adaptation is mediated by both intrinsic factors, such as neuromuscular adaptability, and extrinsic prosthetic factors, most notably the contour and thickness of the anterior palatal base. An optimal thickness in the range of 1.5–2.0 mm has been shown to facilitate clearer sibilant articulation. The palatogram remains a practical, cost-effective, and visually demonstrative method for mapping tongue-palate contact, thereby enabling precise modifications to denture design that can enhance speech intelligibility during both clinical try-in and post-insertion assessments. Considering the documented variability in adaptation based on patient age, gender, and prior denture experience, individualized prosthodontic planning supplemented with phonetic monitoring via palatography is mandatory.
AUTHORS’ CONTRIBUTIONS
The authors confirm their contributions to the paper as follows: N.F., H.K.: Study conception and design; I.G.: Analysis and interpretation of results; S.R.H.: Draft manuscript; O., F.L.K.: Project administration. All authors reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| RISKESDAS | = Indonesian Basic Health Survey |
| CRD | = Complete Removable Dentures |
| PIP | = Pressure Indicator Paste |
| CUD | = Complete Upper Denture |
| fMRI | = Functional Magnetic Resonance Imaging |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Ethical clearance was obtained from Ethical Committee Faculty of Dentistry Universitas Indonesia No.72/Ethical Clearance/FKGUI/XI/2011.
HUMAN AND ANIMAL RIGHTS
All procedures performed in studies involving human participants were in accordance with the ethical standards of institutional and/or research committee and with the 1975 Declaration of Helsinki, as revised in 2013.
CONSENT FOR PUBLICATION
Informed consent was obtained from all participants prior to the commencement of the study.
AVAILABILITY OF DATA AND MATERIALS
All data generated or analyzed during this study are included in this published article.
ACKNOWLEDGEMENTS
Declared none.


