All published articles of this journal are available on ScienceDirect.
Nasolabial Appearance Evaluation by Surgeons and Inexperienced Health Workers after Primary Unilateral Cleft Lip Repair Using the Cronin Technique
Abstract
Introduction
One of the most critical measures of successful unilateral cleft lip repair is the evaluation of nasolabial appearance. This study aimed to assess nasolabial appearance following lip repair using the Cronin technique in patients with complete unilateral cleft lip, employing the Unilateral Cleft Lip Surgical Outcomes Evaluation (UCL SOE) scale.
Methods
Nine evaluators from different professional backgrounds, including three oral and maxillofacial surgeons, three oral and maxillofacial surgery residents, and three dental nurses, conducted the assessments. Twenty-four pairs of photographs of patients with unilateral cleft lip who underwent lip repair using the Cronin technique were evaluated. Intra- and inter-evaluator reliability tests were performed using the intraclass correlation coefficient (ICC).
Results
The intraclass correlation coefficients for each component and for the total score showed that the oral and maxillofacial surgeons demonstrated very high reliability, scoring 1.00 on nearly all components, which indicates an almost perfect correlation.
Discussion
The intra-evaluator and inter-evaluator ICC values demonstrated consistent and reliable results for evaluating the esthetic outcomes of unilateral cleft lip repair using the Cronin technique. However, differences were observed in the assessments among the different evaluator groups.
Conclusion
The evaluation of nasolabial appearance using the UCL SOE scale demonstrated good reliability and consistency across evaluators, regardless of professional background. Furthermore, the Cronin technique used in this study can be recommended for unilateral cleft lip repair.
1. INTRODUCTION
Cleft lip and palate are the most common facial congenital abnormalities occurring in all populations and ethnic groups worldwide. The incidence of cleft lip and palate varies by geographic location, ethnicity, and sex [1-3]. According to the 2018 Indonesian Basic Health Research data, births with cleft lip and palate abnormalities accounted for 0.12% of the Indonesian total population, and the national prevalence of cleft lip in Indonesia is 0.2% [3, 4].
The main goal of cleft repair is to restore the lip, palate, and nose to a symmetric anatomical shape, palatal function, and normal speech [5, 6]. Additionally, a symmetrical, functional, and aesthetically acceptable lip contour, vermilion border, and nasal structure is the objective of cleft lip repair [6]. Cleft lip repair is ideally performed at 3–6 months of age [7]. Over the past few decades, surgical methods for repairing unilateral cleft lips have changed tremendously, particularly in tissue manipulation, careful surgical technique, and personalized planning [6]. However, every cleft lip repair method has its advantages and disadvantages. Among the current methods, surgeons often use the Millard, Tennison–Randall, Fisher, and Cronin techniques.
Evaluation of treatment outcomes is essential to identify and implement the highest possible standard of care [7, 8]. One of the most critical measures of successful unilateral cleft lip repair is nasolabial appearance evaluation because it enables esthetic correction of the deformity and balances midface development [8]. The appearance of the lip and nose is an aspect of concern, and if the result is unsatisfactory, patients with clefts and their parents often desire further repair [7].
Nasolabial appearance evaluation can be performed using quantitative and qualitative methods [8, 9]. Anthropometric measures of facial soft tissues are used as quantitative methods to assess the degree of asymmetry and the morphology of the nose and lip [9]. Conversely, qualitative methods are more subjective and use indices, scales, and rankings to analyze facial esthetics and appearance [8]. A standardized and objective assessment method can improve the accuracy and reliability of nasolabial esthetic outcome evaluations.
Experts in the cleft field have introduced various nasolabial appearance evaluation methods, such as the cleft lip evaluation profile and the Asher–McDade scale [10, 11]. Regarding the need for better outcome measurement, a team of cleft surgeons developed the unilateral cleft lip surgical outcomes evaluation (UCL SOE) scale. This scale evaluates four anthropomorphic elements of cleft lip repair, including the nose, Cupid’s bow, lateral lip, and free vermillion, with a three-point scoring system for each element [11].
The Faculty of Dentistry Universitas Indonesia, one of the leading dental schools in Indonesia, offers an 8-semester oral and maxillofacial surgery (OMFS) specialist program. The integrated management of cleft lip and palate is part of the curriculum for OMFS residents. Residents are introduced to the diagnosis, risk factors, embryology, and comprehensive multidisciplinary management of cleft lip and palate cases, and independently perform cleft lip and palate surgeries.
In the Faculty of Dentistry Universitas Indonesia, the Cronin technique is used for unilateral cleft lip repair (Fig. 1). This technique is a modification of the Tennison–Randall triangular flap in which a triangular flap is designed 1 mm above the vermilion border, thus preventing the vermilion border from being pulled out of position postoperatively. This technique reduces the height of the vermilion on the cleft side by 1 mm compared to the unaffected side, allowing for postoperative growth. This condition could prevent drooping of the upper lip on the affected side due to growth. The Cronin technique offers ease of length measurement and design, allowing inexperienced surgeons to achieve relatively stable and reliable results [12-14].
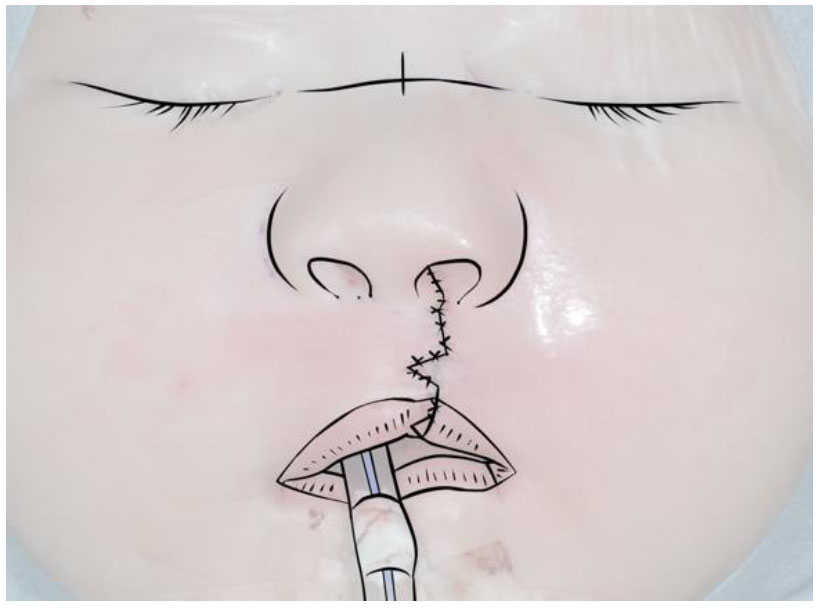
Cronin unilateral cleft lip repair.
In Indonesia, no study has evaluated nasolabial appearance following cleft lip repair with the Cronin technique using the UCL SOE scale in patients with unilateral cleft lip. Thus, this study aimed to evaluate the nasolabial appearance following cleft lip repair with the Cronin technique in patients with unilateral cleft lip performed by senior OMFS residents and surgeons who graduated from the Faculty of Dentistry, Universitas Indonesia. The study also aimed to determine whether a difference exists between the assessment of nasolabial appearance using the UCL SOE scale performed by experienced OMF surgeons, OMFS residents, and dental nurses unfamiliar with cleft lip treatment.
2. MATERIALS AND METHODS
2.1. Study Design
This cross-sectional study included 24 children with unilateral cleft lip. The 24 study subjects were obtained based on Lemeshow's formula, with a population proportion of 0.0012.
| Patient No | Sex | Diagnosis | Age at the Time of Surgery |
|---|---|---|---|
| 1 | Male | Unilateral complete cleft lip and palate–left | 7 months |
| 2 | Male | Unilateral complete cleft lip and palate–right | 4 months |
| 3 | Female | Unilateral complete cleft lip and palate–right | 2 years |
| 4 | Male | Unilateral complete cleft lip and palate–right | 3 months |
| 5 | Female | Unilateral complete cleft lip and alveolus–left | 4 months |
| 6 | Male | Unilateral incomplete cleft lip and alveolus–left | 3 months |
| 7 | Male | Unilateral incomplete cleft lip and alveolus–left | 6 years and 3 months |
| 8 | Male | Unilateral complete cleft lip and palate–left | 3 months |
| 9 | Male | Unilateral complete cleft lip and palate–left | 7 months |
| 10 | Female | Unilateral complete cleft lip and palate–left | 6 months |
| 11 | Female | Unilateral complete cleft lip and palate–left | 1 year and 10 months |
| 12 | Male | Unilateral incomplete cleft lip–right | 6 months |
| 13 | Male | Unilateral complete cleft lip and palate–right | 1 year and 9 months |
| 14 | Male | Unilateral complete cleft lip and palate–left | 7 months |
| 15 | Male | Unilateral complete cleft lip and palate–left | 6 months |
| 16 | Male | Unilateral complete cleft lip and palate–left | 1 year and 11 months |
| 17 | Male | Unilateral complete cleft lip and palate–Right | 5 months |
| 18 | Female | Unilateral complete cleft lip and alveolus–left | 4 years and 10 months |
| 19 | Female | Unilateral complete cleft lip and palate–left | 11 years and 2 months |
| 20 | Male | Unilateral complete cleft lip and palate–right | 3 years and 6 months |
| 21 | Female | Unilateral incomplete cleft lip and alveolus–right | 11 years and 8 months |
| 22 | Male | Unilateral complete cleft lip and palate–right | 4 months |
| 23 | Male | Unilateral incomplete cleft lip and palate–right | 3 months |
| 24 | Female | Unilateral incomplete cleft lip and alveolus–left | 7 months |
The population proportion was obtained from the prevalence of cleft lip in Indonesia, which was 0.12% based on the National Report of Basic Health Research by the Ministry of Health of the Republic of Indonesia (Riset Kesehatan Dasar Kementerian Kesehatan Republik Indonesia) in 2018. All patients had undergone primary unilateral cleft lip repair using the Cronin technique between 2020 and 2024, performed by six surgeons responsible for cleft surgeries (Table 1).
2.2. Nasolabial Appearance Scoring
The nasolabial appearance was assessed using the UCL SOE scale. Four distinct anthropomorphic elements of the cleft lip repair—nose, Cupid’s bow, lateral lip, and free vermillion—were scored for symmetry using the scale (Fig. 2). A three-point scoring system was used for each element: 2 points for excellent, 1 for mild asymmetry, and 0 for unacceptable (Fig. 3) [11].
2.3. Experimental
The assessment of nasolabial appearance using the UCL SOE scale was performed by three groups of evaluators (DA, NN, M), comprising three experienced OMF surgeons from the Department of OMFS, three OMFS residents, and three dental nurses from Universitas Indonesia Hospital, who were unfamiliar with cleft lip treatment. Before the assessment, all evaluators received a training session and were calibrated. All evaluators assessed the nasolabial appearance according to the UCL SOE scale two times at a 1-week interval. Furthermore, intra- and inter-evaluator reliability assessments were performed using the intraclass correlation coefficient (ICC).
3. RESULTS
The study included 24 patients with clefts, comprising 16 males and 8 females (Table 1). The results of the descriptive study show the evaluators' assessments of three groups on several aspects of the anatomical structure of the facial area, namely, the nose, Cupid’s bow, lateral lip, and free vermilion (Table 2). The OMF surgeons received the lowest average assessment, with a total average score of 4.73 and a standard deviation (SD) of 1.07, ranging from a minimum score of 3.00 to a maximum of 6.33. In the specific assessment, the nose had a mean score of 0.79 (SD 0.40); Cupid’s bow, 0.92 (SD 0.49); lateral lip, 1.31 (SD 0.37); and free vermilion, 1.47 (SD 0.39). OMFS residents assessed the same aspects with higher scores, showing an overall mean of 5.81 (SD 1.65), ranging from 3.00 to 8.00. The mean scores for individual components were: nose, 1.06 (SD 0.64); Cupid’s bow, 1.40 (SD 0.56); lateral lip, 1.62 (SD 0.48); and free vermilion, 1.72 (SD 0.43).
Dental nurses gave the highest overall assessment, with a mean score of 6.06 (SD 1.19), ranging from 4.00 to 8.00. The mean scores for individual aspects were: nose, 1.06 (SD 0.47); Cupid’s bow, 1.64 (SD 0.40); lateral lip, 1.60 (SD 0.35); and free vermilion, 1.75 (SD 0.23). Across all three evaluator groups, the nose consistently received lower scores compared with the other aspects. The free vermilion, in contrast, received the highest rating among all facial anatomy components assessed.
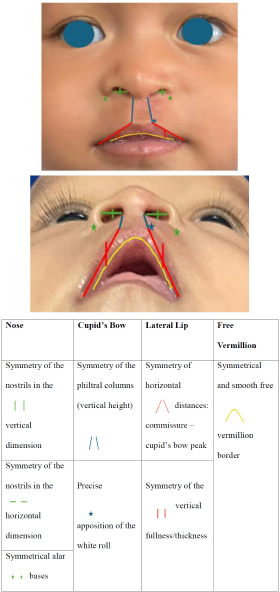
Four distinct anthropomorphic elements of cleft lip repair based on the UCL SOE scale.
3.1. Intra-evaluator ICC
A reliability test was conducted using the ICC to ensure consistent measurement results that can be applied repeatedly. ICC <0.20 indicates poor agreement; 0.21–0.40, fair agreement; 0.41–0.60, moderate agreement; 0.61–0.80, substantial agreement; and 0.81–1.00, almost perfect agreement. The ICCs for individual assessments and the average for each group are displayed in Table 3.
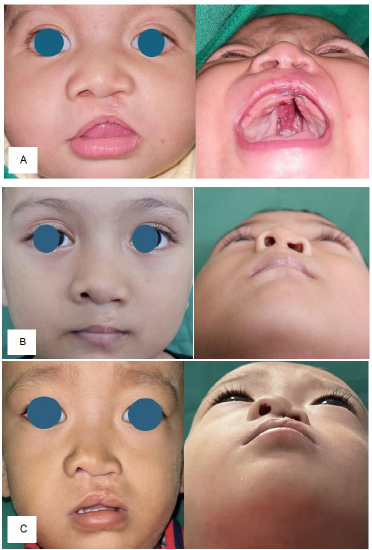
Photographs of 3 patients with different scores from the evaluators for the nose, cupid's bow, lateral lip, and free vermilion aspects. A) Excellent; B) Mild asymmetry; C) Unsatisfactory.
Table 3 shows the ICCs for the intra-evaluator reliability test of the three groups of raters for the nose, Cupid’s bow, lateral lip, vermilion border, and total score. Overall, the ICCs for each component and the total score showed that OMF surgeons had very high ICCs and scored 1.00 on nearly all components, indicating an almost perfect correlation. For the lateral lip, the ICCs were slightly lower, ranging from 0.911 to 0.860. The ICCs for the total score were also high, with values between 0.975 and 0.976, indicating an excellent consistency level among assessments by OMF surgeons.
OMFS residents showed good to excellent consistency on most components. The highest ICCs were obtained for Cupid’s bow and the total score (0.968 and 0.980, respectively), indicating an almost perfect correlation. The lowest ICC was recorded for the lateral lip (0.807); however, it was still in the good category. These results indicate that OMFS residents also had a good level of consistency in their ratings, albeit slightly lower than OMF surgeons.
Dental nurses showed greater variations in ICCs on the various components. The highest ICC was obtained for the nose and free vermilion (1.00), indicating an almost perfect correlation, whereas the lowest value was recorded for the lateral lip (0.623). However, the correlation was still good. The ICC for the total score was also in the good to excellent category, showing that the consistency level of nurses’ assessments varied between components. However, the results were still classified as moderate to good overall.
3.2. Inter-evaluator ICC
To assess the consistency of the measurement results between the evaluators (inter-evaluator reliability), an ICC test was performed on the assessment of the nose, Cupid’s bow, lateral lip, free vermilion, and total score. This inter-evaluator reliability test aimed to ensure the consistency of assessments between evaluators from diverse backgrounds and expertise levels, thereby ensuring that measurement results are considered valid and reliable across various evaluation conditions.
Table 4 shows the ICC values for the inter-evaluator reliability test of the three groups of evaluators for the nose, Cupid’s bow, lateral lip, vermilion border, and total score. Overall, the ICCs for each component and the total score showed that all evaluators had fairly good ICCs, with a total ICC of 0.929, indicating an almost perfect correlation. The component with the highest ICC was the nose (0.918), which was categorized as very good, whereas the free vermilion had the lowest ICC (0.714), which was categorized as good. This result shows good consistency between evaluators, despite variations between the components.
| Evaluator | Anthropomorphic Elements of Cleft Lip Repair | N | Mean | SD | Min. | Max. |
|---|---|---|---|---|---|---|
| OMF surgeons | Nose | 24 | 0.79 | 0.40 | 0.00 | 1.33 |
| Cupid’s bow | 24 | 0.92 | 0.49 | 0.16 | 1.66 | |
| Lateral lip | 24 | 1.31 | 0.37 | 0.66 | 2.00 | |
| Free vermilion | 24 | 1.47 | 0.39 | 0.66 | 2.00 | |
| Total score | 24 | 4.73 | 1.07 | 3.00 | 6.33 | |
| OMFS residents | Nose | 24 | 1.06 | 0.64 | 0.00 | 2.00 |
| Cupid’s bow | 24 | 1.40 | 0.56 | 0.16 | 2.00 | |
| Lateral lip | 24 | 1.62 | 0.48 | 0.83 | 2.00 | |
| Free vermilion | 24 | 1.72 | 0.43 | 1.00 | 2.00 | |
| Total score | 24 | 5.81 | 1.65 | 3.00 | 8.00 | |
| Dental nurses | Nose | 24 | 1.06 | 0.47 | 0.33 | 2.00 |
| Cupid’s bow | 24 | 1.64 | 0.40 | 0.66 | 2.00 | |
| Lateral lip | 24 | 1.60 | 0.35 | 1.00 | 2.00 | |
| Free vermilion | 24 | 1.75 | 0.23 | 1.33 | 2.00 | |
| Total score | 24 | 6.06 | 1.19 | 4.00 | 8.00 |
| Evaluator | Nose | Cupid’s Bow | Lateral Lip | Free Vermilion | Total |
|---|---|---|---|---|---|
| OMF surgeons | |||||
| 1 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| 2 | 1.00 | 0.981 | 0.911 | 0.954 | 0.975 |
| 3 | 1.00 | 1.00 | 0.860 | 1.00 | 0.976 |
| OMFS residents | |||||
| 1 | 1.00 | 0.968 | 0.807 | 1.00 | 0.980 |
| 2 | 0.926 | 0.911 | 0.933 | 0.839 | 0.954 |
| 3 | 0.954 | 0.935 | 1.00 | 1.00 | 0.978 |
| Dental nurses | |||||
| 1 | 1.00 | 0.935 | 0.902 | 1.00 | 0.979 |
| 2 | 1.00 | 0.836 | 0.623 | 0.734 | 0.956 |
| 3 | 1.00 | 1.00 | 1.00 | 1.00 | 1.00 |
| Evaluator | Nose | Cupid’s Bow | Lateral Lip | Free Vermilion | Total |
|---|---|---|---|---|---|
| OMF surgeons | 0.852 | 0.798 | 0.769 | 0.763 | 0.858 |
| OMFS residents | 0.986 | 0.976 | 0.971 | 0.982 | 0.992 |
| Dental nurses | 0.860 | 0.876 | 0.773 | 0.371 | 0.897 |
| all | 0.918 | 0.909 | 0.840 | 0.714 | 0.929 |
OMF surgeons had a total ICC of 0.858, indicating reasonably good consistency between evaluators in this group. The highest ICC was obtained for the nose (0.852), which was considered very good, whereas the lowest ICC was noted for the lateral lip (0.769), which was in the good category. This result indicates that the consistency between specialists is quite high, but slightly low in some components.
OMFS residents showed high reliability, with a total ICC of 0.992. All components had high ICCs, particularly the nose (0.986) and free vermilion (0.982). This result shows that residents have an almost perfect correlation among evaluators, indicating a very good assessment of all components.
Dental nurses had ICCs that varied between components, with a total of 0.897, which showed an almost perfect correlation. The highest ICC was obtained for Cupid’s bow (0.876), which was in the very good category, whereas free vermilion had the lowest ICC (0.371), which was in the fair category. These results show high variability between dental nurses’ assessments for this component.
These results indicate that OMFS residents had the highest inter-evaluator consistency compared with other groups, followed by OMF surgeons and then dental nurses. Free vermilion appeared more challenging to rate consistently, particularly among dental nurses, who may require further training to improve inter-evaluator consistency.
4. DISCUSSION
Esthetics, speech function, maxillary growth, dental arch relationships, and psychosocial factors are factors considered in cleft lip and palate treatment evaluation [15, 16]. There is more to unilateral cleft lip and palate than a lip and palate defect. Maxillary bone deficiency, nasal deformity, and dynamics of lip and muscular strength—which account for most of the nose and maxilla distortion—are among the components of the issue that must be addressed to repair this deformity. The orbicularis oris muscle significantly influences the growth of the maxilla. To balance the force on the maxilla, nasal tip, and lip, muscular reconstruction is essential [17]. Primary unilateral cleft lip–nose repair aims to physiologically restore the anatomy of the lip and nose by ensuring the correct repositioning of the various structures, including the nose. In 1965, Dr. Thomas Cronin modified the Tennison–Randall unilateral cleft lip repair technique by adding a 1-mm vertical line above the vermillion. Dr. Cronin’s consideration arose from the likelihood of confusing the vermilion ridge with the oblique scar of the triangular flap when the two were connected [12]. The modified Cronin technique is currently being used at the Faculty of Dentistry, Universitas Indonesia, for primary cleft lip–nose repair [18].
The assessment of the nasolabial appearance is an essential esthetic factor in the evaluation following cleft lip repair. The esthetic outcome of cleft lip repair is frequently assessed using reliable and simple scoring methods. Individual evaluations of nasolabial appearance based on standardized objective rating scales are more detailed than approaches without a standard reference [19]. The UCL SOE scale was developed by cleft surgeons at Operation Smile to assess the esthetic results of primary UCL repair rapidly, effectively, reliably, and efficiently. Founded in 1982, Operation Smile is a global nonprofit organization that provides free cleft surgeries and comprehensive cleft care to patients with clefts in developing countries. The UCL SOE scale presents as a reliable instrument that is easy to use, even by laypersons, to evaluate the results of cleft lip repair [11]. The more straightforward approach of the UCL SOE scale makes it easier to apply. It increases the consistency of assessment compared with the Asher–McDade scale, which uses a consistent method that rates each of the four nasolabial components (nasal form, nasal symmetry, nasal profile, and vermilion border) on a 5-point scale [11, 20].
In this study, the UCL SOE scale was used to evaluate patients with unilateral cleft lip who underwent lip repair using the Cronin technique, which was performed by three groups: three OMF surgeons, three OMFS residents, and three dental nurses. The results showed that the average UCL SOE scale score was the highest among dental nurses (6.06), followed by OMFS residents (5.81), and the lowest among OMF surgeons (4.73). These results demonstrate that the Cronin technique is a reliable and effective method for unilateral cleft lip repair, yielding satisfactory outcomes. The difference in assessment between OMF surgeons and OMFS residents may be due to several factors, such as the experience level, in-depth understanding of surgical techniques, and subjective perception of the esthetic results of the surgical procedure. OMF surgeons generally have more extensive experience and more profound knowledge of surgical techniques, whereas OMFS residents, although well-trained, may not have the same experience in performing procedures or evaluating their results [21, 22]. In addition, differences in the education and training of specialists and residents may lead to variations in the accuracy level of assessments, as specialists are more familiar with various, more complex surgical outcomes and may identify subtleties that may be missed by residents who are still in the learning stage. Furthermore, this difference may also be influenced by subjectivity in esthetic assessment [22, 23].
Esthetics is highly dependent on individual perception; thus, the standard for assessing surgical outcomes may vary among individuals [24, 25]. OMF surgeons who have performed various procedures may be more likely to have higher expectations regarding symmetry and functionality. In contrast, OMFS residents with less experience may focus more on achieving basic results according to the surgical technical guidelines.
Specific knowledge of surgical techniques and the ability to identify and assess esthetic outcomes more critically may also influence this assessment. The results of the intra-evaluator reliability test showed that OMF surgeons had the highest ICCs among the three groups. OMF surgeons demonstrated almost perfect ICCs and scored 1.00 in nearly all assessment components, indicating excellent consistency in their assessments. Only the ICC of the lateral lip component was slightly lower, ranging from 0.911 to 0.860, but still within the high category. This ICC indicates that OMF surgeons have an excellent consistency level in providing assessments in the main aspects, such as the nose, Cupid’s bow, and free vermilion. This very high level of consistency may be influenced by extensive experience and a deep understanding of what should be evaluated in surgical outcomes. With years of experience, specialists can provide more consistent assessments despite slight variations between individuals.
Regarding inter-evaluator reliability, OMFS residents showed the best results with a total ICC of 0.992, indicating an almost perfect correlation between the raters in this group. All assessment components by the residents showed very high ICCs, particularly the nose (0.986) and free vermilion (0.982). This finding shows that despite background and experience differences between raters, the consistency in the evaluation is very high. Although the ICCs vary between components, dental nurses showed a total ICC of 0.897, which still shows an almost perfect correlation. However, specific components, such as the free vermilion, had the lowest ICC at 0.371, indicating fair agreement. This result shows that the assessment by dental nurses is less consistent in some aspects; however, overall, it is still acceptable.
In this study, the reliability of the ICC also indicated that the assessment results were reliable even with evaluators with different backgrounds, including specialists, residents, and dental nurses. Based on the ICCs obtained, the esthetic assessment of primary cleft lip repair results using the UCL SOE scale can be well accepted. The ICCs higher than 0.80 in most assessment components indicate very good consistency, which is in line with the findings of other studies also using the UCL SOE scale. “Very good” reliability (ICC ≥ 0.80) was achieved by combining the results of several evaluators, as indicated by the ICC approaching 1 in several components.
This study shows that the Cronin technique can produce adequate esthetic results, improve facial symmetry, and enhance patients’ quality of life. Evaluation using the UCL SOE scale provides an objective, reliable, and consistent assessment, which is important in determining optimal care standards for patients with unilateral cleft lip. Evaluation using the UCL SOE scale provides an objective, reliable, and consistent assessment, which is important in determining optimal care standards for patients with unilateral cleft lip.
5. STUDY LIMITATIONS
This study has several limitations. Firstly, this study was unable to determine the age at surgery or the nasolabial evaluation in the same age group. This condition was due to the different characteristics of each region, the hospital's remote location, the fact that children were already attending school, and other factors, which made it challenging to recall patients. The second limitation was that different operators performed the surgeries, but all had the same background from the Faculty of Dentistry, Universitas Indonesia.
CONCLUSION
In this study, intra-evaluator and inter-evaluator ICCs yielded consistent and reliable results for evaluating the esthetic outcomes of unilateral cleft lip repair using the Cronin lip repair technique; however, differences were observed in the assessments between the different evaluator groups. The evaluation of nasolabial appearance using the UCL SOE scale demonstrated good reliability and consistency, regardless of the evaluator's background. In addition, the technique used in this study, the Cronin method, can be recommended for unilateral cleft lip repair.
AUTHORS’ CONTRIBUTIONS
The authors confirm their contribution to the paper as follows: D.A.: Research concept and design; G.W.P., K.F., S.A.: Collection of data; D.A., G.W.P., K.F., M., N.N.: Data analysis and interpretation; D.A., G.W.P.: Writing the article; D.A., G.W.P., K.F., M.N.A., N.N.: Critical revision of the article; D.A., G.W.P., K.F., M., S.A., M.N.A., N.N.: Final approval of the article. All authors have read and agreed to the published version of the manuscript.
LIST OF ABBREVIATIONS
| ICC | = Intraclass Correlation Coefficient |
| OMF | = Oral and Maxillofacial |
| OMFS | = Oral and Maxillofacial Surgery |
| UCL SOE | = Unilateral Cleft Lip Surgical Outcomes Evaluation |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
The present was approved by the Dental Research Ethics Committee of the Faculty of Dentistry, Universitas Indonesia, Indonesia (No.43/Ethical Approval/FKGUI/VII/2024).
HUMAN AND ANIMAL RIGHTS
All procedures performed in studies involving human participants were in accordance with the ethical standards of institutional and/or research committee and with the 1975 Declaration of Helsinki, as revised in 2013.
CONSENT FOR PUBLICATION
Written informed consent has been taken from the patients’ parents for publication of this study.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article is available in the: https://drive.google.com/drive/folders/1 O00COZ6Az_LpOPAN124uOYIEeebA8rpe?usp=share_link.
FUNDING
This study received financial support from the Directorate of Research Funding and Ecosystem, Universitas Indonesia, Indonesia, through the International Indexed Publication Grant 2024 (Hibah PUTI Pascasarjana 2024), Grant number NKB-94/UN2.RST/HKP.05.00/2024.
ACKNOWLEDGEMENTS
Declared none.


