All published articles of this journal are available on ScienceDirect.
Vertical Teeth Preparation: A Comprehensive Systematic Review of Patient Outcomes and Clinical Complications
Abstract
Objective
This study aimed to evaluate the influence of vertical tooth preparation techniques on tooth-supported fixed restorations, with specific attention to survival and success rates, periodontal outcome, and clinical complications.
Methods
A comprehensive literature search of related randomized controlled trials, prospective/retrospective cohort studies, and clinical trials was accomplished across electronic databases (MEDLINE/PubMed, ScienceDirect, Scopus, and Cochrane Central Library) up to March 2025. Primary outcomes included survival and success rates of tooth-supported fixed prostheses, whereas secondary outcomes encompassed periodontal health indices (bleeding, plaque, and recession), patient satisfaction, and mechanical/biological complications. Studies with a minimum follow-up period of six months were considered. Two reviewers independently conducted studies collection, data extraction, and quality assessment.
Results
This systematic review (12 studies, 2012–2024) evaluated patient outcomes and clinical complications of vertical preparation. Survival rates ranged from 96.5% to 100% across preparation types [biologically oriented preparation technique (BOPT), feather-edge, and chamfer]. Success rates (78%–100%) and periodontal outcomes also varied: plaque indices (57.9%–82% score 0), pocket depths (≤3 mm in 80%–97.9% cases), and bleeding on probing (8.4%–55.5%) showed no clear preference for any preparation method. BOPT and feather-edge correlated with lower bleeding rates than chamfer. Mechanical complications (ceramic chipping: 1.4%–15%) were more frequent than biological issues (2%–2.7%). Survival rates and patient satisfaction (80%–100%) were high.
Discussion
The findings of this systematic review supported the use of vertical techniques as a reliable option for fixed prostheses, balancing structural preservation and long-term success, making them a viable, tissue-preserving choice when indicated.
Conclusion
Vertical preparation techniques demonstrated favorable periodontal outcomes, high survival rates, and high patient satisfaction. Manageable mechanical and biological complications supported their viability for tooth-supported prostheses.
1. INTRODUCTION
Tooth preparation involves the mechanical modification of diseased and/or healthy tooth structures (enamel, dentin, and cementum) to restore aesthetics, function, and structural integrity [1]. The primary challenge during tooth preparation is balancing aesthetic outcomes with minimally invasive procedures that preserve tooth structure, which enhances crack resistance, stress distribution, and long-term durability [2]. Traditional methods for preparing teeth for fixed dental prostheses, such as horizontal designs (e.g., chamfer or shoulder margins), often necessitate substantial tissue removal. These risks weaken tooth integrity, may trigger gingival margin displacement, and potentially compromise long-term outcomes due to various factors, such as insufficient keratinized tissue, procedural trauma, or chronic inflammation from prosthetic inaccuracies [3]. The designs of preparations as vertical (red bur) and horizontal (blue bur) for anterior teeth are shown in Fig. (1A), while those for posterior teeth are presented in Fig. (1B).
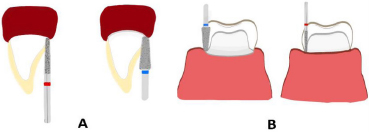
Designs of vertical and horizontal preparations for anterior teeth (A) and posterior teeth (B).
By contrast, vertical preparation techniques, including feather-edge designs and the BOPT, have emerged as conservative alternatives [4]. These methods minimize structural reduction while addressing aesthetic and biological challenges [5]. Vertical preparations are particularly advantageous for patients with thick or medium periodontal biotypes, periodontal attachment loss, or probing depths exceeding 2 mm, where horizontal approaches could exacerbate tissue loss [5, 6]. Vertical preparations are also effective for managing subgingival caries and adjusting gingival morphology by situating crown margins beneath the gingival level [7]. This strategy is especially beneficial for teeth with insufficient clinical crowns, such as lower anterior incisors, where conventional horizontal reduction could lead to excessive tissue removal [8].
BOPT, a subset of vertical techniques, eliminates defined finish lines through vertical milling and replaces the natural crown emergence profile at the cementoenamel junction with a prosthetic-defined contour [9]. This process is complemented by rotary curettage of the gingival sulcus, adapted from periodontal protocols [10]. In periodontally healthy patients, this technique removes sulcular epithelium and prompts localized bleeding and subsequent connective tissue reorganization under provisional restorations [9]. The resulting prosthetic cementoenamel junction mimics natural anatomy and aligns crown margins 0.5–1 mm from the gingival margin to prioritize tissue stability and aesthetic integration [11, 12].
Studies comparing vertical and horizontal techniques have revealed vertical preparation to achieve similar or superior outcomes in periodontal health and clinical performance [13]. Vertical preparation of maxillary and mandibular incisor teeth for full-coverage restorations exhibited impressive longevity with survival rates exceeding 48–72 months, alongside optimal periodontal outcomes, such as stable gingival margins, enhanced tissue thickness, and minimal inflammation [14, 15]. A research study on posterior vertical preparation restorations also demonstrated enhanced marginal stability, reduced plaque accumulation, lower gingival scores, and fewer deep periodontal pockets over 60 months compared to horizontal methods [11]. While complication rates are comparable, vertical preparation cases often show better clinical responses, which positions it as another choice [11].
In addition to the type of preparation, the material used influences the behavior of the surrounding soft tissues. Long-term evaluations of minimally invasive zirconia crowns prepared with vertical preparation demonstrated reliability, no failures or complications over 36 months, and a high survival rate and patient satisfaction [4]. Other studies have exhibited ceramic restorations to achieve vertical marginal gaps falling within the clinically acceptable range [16, 17]. Vertical preparation techniques effectively balance aesthetic and structural preservation, and 84 months of studies have shown stable marginal integrity and favorable esthetic outcomes, minimizing tooth structure removal while delivering durable results [18].
Despite promising evidence, systematic reviews evaluating the vertical preparation efficacy and its influence on periodontal health remain limited. A recent meta-analysis revealed no remarkable differences in periodontal outcomes (e.g., plaque, recession, and restoration success) between BOPT and horizontal techniques [1]. This study aimed to provide a systematic review and evaluation of the clinical performance, periodontal outcomes, patient satisfaction, and clinical complications of vertical preparation as a routine alternative to conventional horizontal preparations in clinical practice, particularly in cases requiring structural preservation, aesthetic integration, and periodontal stability.
2. MATERIALS AND METHODS
2.1. Protocol Registration
This systematic review protocol was developed and registered in PROSPERO (CRD420251025721) in 2025. Its progress has been consistently tracked and reported in accordance with the preferred reporting items for systematic reviews and meta-analyses (PRISMA) guidelines [20]. The procedure and method quality of the present systematic review was evaluated utilizing the AMSTAR 2 instrument [21].
2.2. Search Strategy
An electronic search was accomplished in January 2025 and updated in March 2025. The inclusion of studies was limited to those published in English, as determined by two independent reviewers (MMA and TAB). The utilized databases included MEDLINE via PubMed (National Library of Medicine), ScienceDirect, Scopus, and Cochrane Central Library (clinicaltrials.gov, US National Library of Medicine). The published gray literature and the bibliography of full-text papers were manually searched to obtain any further articles eligible for inclusion. Boolean operators ‘AND’ and ‘OR’ were employed to combine the keywords and generate the search strategy. Table 1 displays the keywords and the complete exploration plan.
| Cochrane Central Library | Biological oriented preparation technique OR vertical preparation technique, OR feather-edge, chamfer, knife-edge finishing line in title, abstract, keyword, AND crown or fixed prosthesis |
| PubMed | (biological oriented) OR (vertical) OR (feather-edge) OR (chamfer) OR (knife edge) OR (finishing line) AND (preparation technique) AND (crown or fixed partial denture) |
| Scopus | (biological oriented) OR (vertical) OR (feather-edge) OR (finishing line) AND (preparation technique) AND (fixed prosthesis) |
| ScienceDirect | “Biological oriented preparation technique” OR “vertical preparation technique” OR “feather-edge finishing line” OR “knife edge finishing line” OR “chamfer finishing line” |
2.3. Eligibility Criteria
Clinical studies, including randomized controlled trials, prospective clinical trials, and retrospective cohort studies, were covered in this systematic review. The inclusion criteria were as follows: participation: tooth-supported fixed prosthesis, intervention: BOPT or vertical preparation for abutment, comparison: horizontal preparation technique or baseline (non-preparation), and outcome: a minimum of 6 months. Periodontal tissue health status (PDI) was measured as follows: bleeding index, plaque index (PI), gingival recession (GR), patient satisfaction, success or survival rates, and biological and mechanical complications. Non-randomized controlled trials and those not relevant to the review question (periodontal outcome, patient satisfaction, clinical complications), studies with low-quality methodological flow, and studies not published in the English language were excluded from the study. Case reports, case series, research studies without a control group, published papers of earlier prepared teeth, and studies without periodontal health outcomes were also excluded.
2.4. Study Selection
Titles, abstracts, and full-text assessments were performed by two independent reviewers (MMA and TAB). Disagreements between the two assessors were resolved through discussion and agreement, after which the data were extracted into a designed table.
2.5. Data Extraction
Relevant data were extracted according to the Cochrane Handbook for Systematic Reviews of Interventions guidelines [22,23], encompassing the characteristics of published papers, including intervention and comparator, periodontal health clinical outcome measures, and biological and mechanical complications.
2.6. Quality Assessment and Risk of Bias
The quality was estimated utilizing the reviewed Cochrane Risk of Bias Tool for Clinical Randomized Trials (RoB 2.0). The domains calculated and judged were randomization, deviations from the intended interventions, missing outcome data, measurement of the documented result, and overall bias. The nominated published papers were categorized into some or medium concerns and low or high risk of bias [24]. The prospective clinical trials studies were judged utilizing the Newcastle–Ottawa Quality Assessment Scale for cohort studies [25]. Percentages (%) for PI, gingival index (GI), GR, survival, success rate, and biological and mechanical complications were calculated to analyze the outcome of interventions through direct comparison.
3. RESULT
3.1. Study Selection
The PRISMA flow chart of the inclusion, selection, and exclusion criteria for the papers is presented in Fig. (2). The search provided 388 hits; 362 were duplicates, and 19 research studies were related, relevant, and obtained in full-text. Full-paper screening omitted seven references because the implant abutment utilized was not specified. Eventually, 12 studies [4, 10-12, 14, 15, 18, 26-30] were included in the present systematic review.
3.2. Characteristics of Included Studies
Table 2 presents the characteristics of the included studies, including the author (s), publication year, study design, finish line type, material used, and follow-up periods in months. The results covered periodontal outcome (PI, GI, PD, and BoP), patient-related variables (as percentage of survival rate, success rate, and patient satisfaction), and complications (mechanical and biological).
Only 12 papers were included in the current systematic review. The first paper was published in 2012 [30], whereas the last one was published in 2024 [18] with 7 prospective clinical trials [4, 10-12, 14, 15, 26, 28], 3 randomized clinical trials [27, 29], and 2 retrospective cohort studies [18, 30]. In relation to the finish line assessed, the highest type was BOPT, assessed in 6 studies [10, 11, 14, 15, 26, 28], followed by the feather or knife-edge, as well as chamfer finish lines types that were assessed in 4 studies each [12, 26, 27, 29, 30]. Vertical preparation was mentioned in 2 studies only [4, 18]. Most of the studies used monolithic zirconia as a prosthetic material or zirconia core covered by feldspathic ceramic, and one study used PFM [18].
A total of 1,033 cemented prostheses, as a single crown or as a part of fixed prosthodontics (FPD), were observed, and the highest numbers per study were 198 and 196, cemented on all types of teeth (incisors, premolars, and molars) [12, 29]. The minimum follow-up period was 6 months [12], whereas the longest follow-up period was 84 months [18].
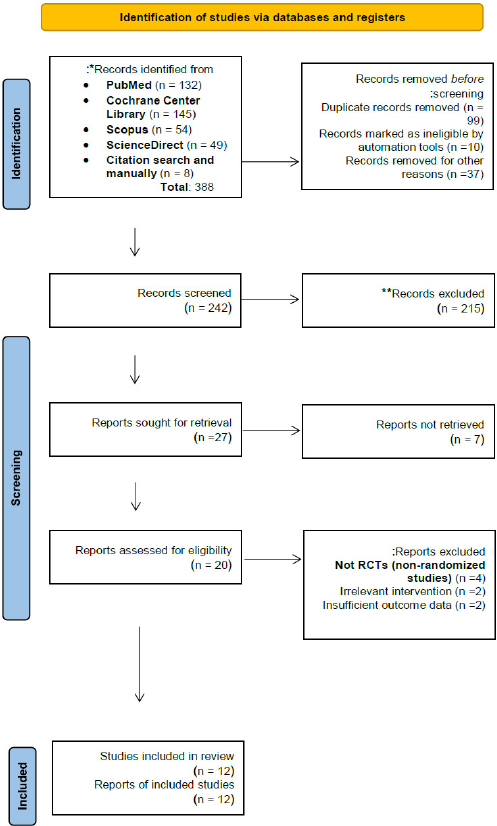
PRISMA flow diagram representing the selection, inclusion, and exclusion of studies at each screening step.
| Author, Year, Type of Study/Refs. | Finish Line Type | Tooth (restoration and material type) | Follow-up Period | Survival/success Rate | Periodontal Outcome | Patient Satisfaction | Mechanical/biological Complications |
|---|---|---|---|---|---|---|---|
| Gonzalez-Bonilla et al., 2024/retrospective cohort study [18] |
Vertical preparation | 50 molars and premolars (25 zirconia crowns and 25 PFM crowns) | 60 and 84 months | NM/zirconia 100% and PFM 86% | PI: 82% score 0, 6% score 1, and 12% having 2 | NM | 4% chipping of the PFM/NM |
| GI: 50% index of 0; 28% index of 1; 20% index of 2 | |||||||
| PD: 80% ≤ 3mm - 20% ↔3 and 5 mm | |||||||
| Serra-Pastor et al., 2023/prospective clinical trial [15] | BOPT | 70 teeth (25 FPDs) | 12, 24, 36, 48, 60, and 72 months | 100%/NM | A 100% significant increase in gingival thickness and a stable gingival margin | NM | NM |
| Kasem et al., 2022/clinical study [4] | Vertical preparation | 40 premolars/20 zirconia and 20 ZL crowns | 6, 12, 18, 24, and 36 months | 100%/NM | 40% scored as 1 and 60% scored as 2 | 100% | No mechanical complications/NM |
| Talaat et al., 2022/clinical study [26] | Chamfer | 44 teeth/zirconia crowns | 6, 9, and 12 months | NM/NM | 40.9% score 0 and 59.1% score 1 in gingival inflammation | NM | NM/NM |
| BOPT | 36.4% score 0 and 63.6% score 1 in gingival inflammation |
||||||
| Serra-Pastor et al., 2021/prospective clinical study [10] | BOPT | 74 incisors, canines, and premolars/zirconia core and feldspathic ceramic covering | 12, 24, 36, 48, 60, and 72 months | 97%/93% | PI: 78.6% score 0; 14.3% score 1; 7.1% score 2 | 90% | 4.1% decementation and complete crown fracture/2.7% pulpitis and vertical fracture |
| PD of 4–6 mm in 1.7% of cases | |||||||
| GR: 2.9% of cases | |||||||
| Agustin-Panadero et al., 2021/prospective observational study [11] |
BOPT | 65 posterior teeth in both arches/zirconia FPD | 12, 36, and 60 months | 100%/95% | PI: 35% of 1 | NM | 10% chipping of ceramic veneer/2.5% irreversible pulpitis |
| GI: 30% of 1 | |||||||
| PD: 10% of 3 mm | |||||||
| Chamfer | PI: 57.9% of 1 | ||||||
| GI: 68.4% of 1, | 15% chipping of veneer/2.5% vertical root fracture | ||||||
| PD: 26.3% of 3mm | |||||||
| Cagidiaco et al., 2019/randomized clinical trial [27] | Feather-edge | 25 premolars and molars/zirconia crowns | 6, 12, 24, 36, and 48 months | 96%/80% | BoP: 48% of cases | NM | 15% crowns chipped and 5% irreparable fractures/NM |
| Chamfer | 25 premolars and molars/zirconia crowns | 100%/76% | BoP: 55.5% of cases | 5 crowns chipped/NM | |||
| Serra-Pastor et al., 2019/prospective study [14] | BOPT | 144 all types of teeth (74 crowns and 75 FPDs)/zirconia core and feldspathic ceramic covering | Every 12 months for 48 months | Zirconia crowns 97%; FPDs 96%/97% | Plaque affecting 20% of teeth after 24 months | 90% | 1.4% porcelain veneer chipping and connector fracture in one FPD/2% pulpitis and vertical fracture |
| GR: 1.4% after 24 months | |||||||
| GI: 12% after 24 months | |||||||
| PD: 97.9% 0 to 3 mm; 2.1% 3–6 mm after 24 months | |||||||
| Agustin-Panadero, 2018/prospective study [28] | BOPT | 149 incisors, canines, premolars (74 crowns and 27 FPDs)/zirconia core and feldspathic ceramic covering | 6, 12, and 24 months | 100%/NM | 80.5% remained without gingival inflammation or bleeding, while 29 (19.5%) showed inflammation and/or bleeding |
80% | 2% porcelain veneer chipping; 0% |
| Paniz et al., 2017/prospective randomized clinical study [12] | Chamfer | 198 incisors, canines, premolars/zirconia crowns | 6 months | NM/ NM | GI: 33.3% score 1; 10.5% score 2; 1.9% score 3 | 91% | NM/NM |
| PI: 15.2% score 1 | |||||||
| BoP: 30.5% score 1 | |||||||
| Feather-edge | GI: 33.3% score 1; 7.5% score 2; 0% score 3 | ||||||
| PI: 9.7% score 1 | |||||||
| BoP: 8.4% score 1 | |||||||
| Paniz et al., 2016/prospective randomized controlled double-blind clinical trial [29] | Feather-edge | 196 incisors, canines, premolars/zirconia crowns | 12 months | NM/NM | GI: 31.5% score 1 and 9.8% score 2 | NM | 1.88% restoration fracture/NM |
| PI: 17.4% score 1 and none score 2 | |||||||
| BoP: 52.2% | |||||||
| GR: 3.3% | |||||||
| Chamfer | GI: 33.7% score 1; 11.5% score 2; 1.9% score 3 | ||||||
| PI: 14.4% score1; 3.8% score 2 | |||||||
| BoP: 36.5% | |||||||
| GR: 11.5% | |||||||
| Poggio et al., 2012/retrospective study [30] | Knife-edge | 102 (38 incisors, 13 canines, 29 premolars, 22 molars)/zirconia core and feldspathic ceramic covering | 72 months | 100%/NM | NM | NM | 1.02% porcelain chipping/NM |
Patient satisfaction was recorded in 5 studies only, with 90% overall satisfaction; the lowest percentage was 80% [28], and the highest was 100% [4]. Only 7 studies documented the survival rate and determined it as 100% [4, 11, 15, 28, 30] and an average of 98% (Cagidiaco et al., 2019) and 96.5% (Serra-Pastor et al., 2019) [14, 27]. Similarly, only five studies reported on the success rate, with findings indicating a 100% success rate for zirconia crowns and 86% for FPD [18]. The reported success rates were 93%, 95%, an average of 78%, and 97% in the studies by Serra-Pastor et al. (2021), Cagidiaco et al. (2019), and Serra-Pastor et al. (2019), respectively [10, 11, 14, 27].
3.3. Mechanical and Biological Complications
Nine studies included the mechanical complications. The highest was related to ceramic chipping and represented as 10%–15% [11, 27], and the lowest was only 1.4% [14]. With regard to biological complications, only three studies reported cases of reversible and irreversible pulpitis, as well as vertical root fractures, accounting for between 2% and 2.7% of the follow-up cases [10, 11, 14].
3.4. Periodontal Outcome
Regarding periodontal outcome, PI was documented in 6 studies, and scores ranged from 82% of cases scoring 0 (no plaque) [18] to 57.9% scoring 1 (mild plaque) under chamfer preparations [11]. The lowest plaque accumulation was observed in the study by Serra-Pastor et al. (2021) [10] with 78.6% scoring 0, whereas the highest occurred under BOPT in the study by Agustin-Panadero et al. (2021) with 35% scoring 1 [11]. Gingival health, assessed via GI, was reported in 6 studies. Healthy gingiva (score 0) ranged from 36.4% [26] to 68.4% with a score of 1 (mild inflammation) under chamfer preparation [11]. Severe inflammation (score 3) was rare and noted in only 1.9% of cases [12]. Serra-Pastor et al. (2019) demonstrated improvement over time, with GI reduced to 12% after 24 months [14].
The GR was recorded in 3 studies, with rates as low as 1.4% after 24 months [14] and up to 11.5% under chamfer preparations [12]. PD outcomes were favorable, as documented in 4 studies. The majority (80%–97.9%) of the cases showed PD ≤3 mm [14, 18]. Deeper pockets (4–6 mm) were rare and occurred in 1.7%–2.1% of the cases [10, 14]. Bleeding on probing (BoP) was reported in 4 studies and varied by preparation technique. The lowest BoP (8.4%) was observed with feather-edge [12], whereas higher rates (36.5–55.5%) were associated with chamfer preparations [12, 27]. BOPT demonstrated intermediate results and 19.5% inflammation/bleeding [28].
| Authpr/Refs. | Randomization Process | Deviations from Interventions | Missing Outcome Data | Measurement of Outcomes | Selection of Reported Results | Overall Risk of Bias |
|---|---|---|---|---|---|---|
| Gonzalez-Bonilla et al., 2024 [18] | √ | √ | √ | √ | √ | √ |
| Serra-Pastor et al., 2023 [15] | √ | √ | √ | √ | √ | √ |
| Kasem et al., 2023 [4] | √ | √ | √ | √ | √ | √ |
| Talaat et al., 2023 [26] | – | √ | √ | – | √ | x |
| Serra-Pastor et al., 2021 [10] | √ | √ | √ | √ | √ | √ |
| Agustín-Panadero et al., 2021 [11] | √ | √ | √ | √ | √ | √ |
| Cagidiaco et al., 2019 [27] | √ | √ | √ | √ | √ | √ |
| Serra-Pastor et al., 2019 [14] | √ | √ | √ | √ | √ | √ |
| Agustín-Panadero et al., 2018 [28] | √ | √ | √ | √ | √ | √ |
| Paniz et al., 2017 [12] | √ | √ | √ | √ | √ | √ |
| Paniz et al., 2016 [29] | √ | √ | √ | √ | √ | √ |
| Poggio et al., 2012 [30] | √ | – | √ | √ | √ | x |
3.5. Risk of Bias Appraisal
Most of the reviewed clinical studies provided information about sample randomization, deviations from interventions, and assessments of outcomes, except for a single study that focused on randomization and measurements of outcomes [26] and deviations from interventions [30], as shown in Table 3. Parameters, including missing outcome data and the selection of reported results, were present in all studies. However, the overall risk of bias was low in 10 studies [4, 10-12, 14, 15, 18, 27-29] and high in 2 studies [26, 30].
4. DISCUSSION
Establishing an optimal relationship between prosthetic restorations and the periodontium is essential for achieving long-term functional and aesthetic success in FPDs [31]. Historically, horizontal finishing lines have led to issues, such as marginal discrepancies, biological complications, and affected aesthetics due to crown adaptation difficulties [3]. Vertical preparation designs have been proposed to enhance precision at the restoration–tooth interface [5]. These preparations, which lack a defined finishing line, may improve marginal seal and soft tissue stability compared to traditional horizontal designs [27].
The majority of systematic reviews and meta-analyses of existing literature have examined the effect of cemented fixed maxillary and mandibular prostheses on the status of gingival and periodontal health as GI and PI, and concentrated on the category and form of the cemented prosthesis, finishing line location, and prosthesis materials [31-33]. One published meta-analysis study focused on the effect of horizontal, traditional, or conventional preparation on soft tissue surrounding associated with natural, unprepared sound teeth [34]. The impact of vertical preparation designs on patient outcomes and clinical complications in fixed prosthodontics remains inconsistent across the literature, making it difficult to draw definitive conclusions.
Previous studies have characterized survival rate as the duration of the fixed prosthesis in situ, regardless of adjustments made during follow-up, whereas success rate has been referred to as prostheses remaining intact without any clinical intervention [19]. In this review, the average survival rate was 98%. These results have been found to align with prior reviews and meta-analyses that have indicated vertical techniques to demonstrate excellent long-term survival potential when performed correctly [13, 19]. Success rates have been found to exhibit more variability, especially for horizontal preparations. Cagidiaco et al. (2019) reported a success rate of 76%, influenced by factors, such as material selection (zirconia versus metal-ceramic), biomechanical challenges, and occlusal loading variations [27]. These discrepancies highlight the importance of evaluating case-specific factors, such as masticatory forces and parafunctional habits, in the choice of preparation design [33].
In this review, six studies [10-13, 26, 27, 29] compared BOPT with chamfer finishing lines. Agustín-Panadero et al. (2021) and Paniz et al. (2017) reported lower PI and GI for BOPT than chamfer with 60 months of follow-up [11, 12]. Talaat et al. (2022) found comparable gingival inflammation outcomes between BOPT (63.6%; score 1) and chamfer (59.1%; score 1) [26]. For BoP, Cagidiaco et al. (2019) reported 48% BoP with feather-edge versus 55.5% with chamfer, suggesting the superiority of BOPT [27]. Moreover, Paniz et al. (2017) observed lower BoP (8.4%) with the feather-edge technique than with chamfer (30.5%) at 6 months [12]. However, Paniz et al. (2016) observed higher BoP (52.2%%) with the feather-edge technique than with chamfer (36.5%) at 12 months [29]. GR outcomes also varied; Serra-Pastor et al. (2021) [10] reported 2.9% GR with BOPT, whereas Paniz et al. (2016) noted 11.5% GR with chamfer [29].
Throughout the follow-up intervals, both groups showed a trend of increasing PD while remaining within clinically acceptable ranges (≤3 mm), particularly with BOPT. Over 80% of cases in the studies carried out by Gonzalez-Bonilla et al. (2024) and Serra-Pastor et al. (2019) had PD ≤3 mm, which indicated stable periodontal health [14, 18]. Deeper pockets (4–6 mm) were rare but more common in chamfer cases [11]. This outcome has been found to be in accordance with other studies that have demonstrated that the placement of margins within the supracrestal tissue can lead to gingival inflammation and possible recession or pocket formation [3, 32]. Despite various clinical factors influencing periodontal health, effective assessment, treatment, self-care instructions, and adherence to maintenance protocols are crucial to mitigating the negative effects of fixed restorations.
The reviewed studies have indicated a high overall patient satisfaction rate of 90%, though mechanical complications, such as ceramic veneer chipping, have remained a concern, with reported incidence rates ranging from 1.4% (14) to 15% [11, 27]. BOPT demonstrated lower mechanical failures of 10% for ceramic chipping and 15% for chamfer [11], whereas feather-edge demonstrated higher mechanical failures of 15% for ceramic chipping and 5% for chamfer [27]. Other studies focused on vertical preparations have reported a 4% PFM chipping rate over 60–84 months as the most common complication (Gonzáles-Bonilla et al., 2024). Serra-Pastor et al. (2021) have found 4.1% crown fractures to be associated with teeth prepared using BOPT [10]. Knife-edge preparations have shown lower complication rates, with Poggio et al. (2012) reporting 1.02% porcelain chipping over 72 months [30]. Biological failures, though less frequent, have included irreversible pulpitis and vertical root fractures associated with chamfer and BOPT [10, 11, 14].
In addition to the clinical trials and cohort studies included in this systematic review, numerous case reports and observational studies have further underscored the promising efficacy of vertical tooth preparation techniques [35]. Agustín-Panadero and Solá-Ruiz (2015) have highlighted the biological advantages of BOPT in maintaining gingival health and stability through controlled tissue remodeling, particularly in aesthetic zones [36]. Recent case reports have further illustrated the efficacy of vertical techniques in achieving optimal aesthetic and functional outcomes for patients with limited clinical crown height, underscoring them as a minimally invasive approach and their adaptability to advanced materials, such as zirconia [37, 38]. These findings have been found to align with the broader literature, which frequently associates vertical preparation with reduced procedural trauma, enhanced marginal adaptation, and improved soft tissue integration [39-41].
The collective evidence reinforces the clinical potential of BOPT techniques, particularly in complex cases requiring structural preservation or periodontal rehabilitation [3, 7]. This growing body of evidence supports the paradigm shift toward vertical preparation as a viable alternative to conventional methods, though its broader adoption necessitates further high-quality, long-term investigations.
5. LIMITATIONS
Only literature published in the English language was included in this study, which represents a limitation. This language restriction may have excluded relevant data and limited the exchange of knowledge from studies published in other languages. The small sample size and limited number of studies on certain outcomes, such as success rates and level of patient satisfaction, may further limit the generalizability of the results. The evidence obtained from the current analysis has supported the usage of vertical preparation, especially BOPT, because it is associated with better periodontal health status, increased patient satisfaction, and lower complications. Future research should focus on periodontal health parameters with similar case selection criteria, larger sample sizes, and long-term follow-ups, and should compare various vertical preparation techniques. This approach could enhance the evidence base for promoting vertical preparation as a standard practice or maintaining it as a specialized approach.
CONCLUSION
This systematic review has demonstrated vertical preparation techniques, such as BOPT and feather-edge designs, to be associated with favorable periodontal outcomes, including reduced plaque accumulation, gingival inflammation, and recession. Survival rates (≥95%) and patient satisfaction (≥90%) have also been found to be high. Mechanical complications, primarily ceramic chipping (1.4%–15%), and rare biological issues (2%–2.7%) have underscored their reliability. While longer-term studies are needed, vertical preparation emerges as a promising approach for tooth-supported fixed prostheses and for balancing periodontal health and prosthetic success.
AUTHORS’ CONTRIBUTIONS
The author confirms sole contribution to the paper as follows: study conception and design, data collection, analysis and interpretation of results, and drafting of the manuscript. The author has reviewed the results and approved the final version of the manuscript.
LIST OF ABBREVIATIONS
| BOPT | = Biologically Oriented Preparation Technique |
| PI | = Plaque Index |
| GR | = Gingival Recession |
| FPD | = Fixed Prosthodontics |
AVAILABILITY OF DATA AND MATERIALS
The data and supportive information are available within the article.
CONFLICT OF INTEREST
Dr. Mohammed M. Al Moaleem is an editorial board member of the Open Dentistry Journal.
ACKNOWLEDGEMENTS
Declared none.


