All published articles of this journal are available on ScienceDirect.
Comparison of Botulinum Toxin and Orthognathic Surgery for Gummy Smile Correction
Abstract
Objective:
This study aimed to compare the changes in the gummy smile in cases treated with botulinum toxin (BTX) application or orthognathic surgery.
Methods:
The retrospective sample comprised 61 subjects with gummy smile divided into 2 groups according to treatment received for gummy smile correction: 1-38 patients (6 male; 32 female), at a mean age of 28.60 years (s.d.=6.09), treated with BTX application; 2- 23 patients (7 males and 16 females) at a mean age of 29.59 years (s.d.=5.72) treated with orthognathic surgery. Patients from the BTX group refused to undergo orthognathic surgery. The measurement of the gingival exposure was performed in extraoral photographs of the posed smile, before and after treatment, and it was defined as the difference between the stomion of the upper lip and the incisal edge of the maxillary central incisor minus the height of maxillary central incisor obtained in the patient's dental casts. The data were obtained before (T1) and after treatment (T2) and change of gingival exposure with treatment (T2-T1). Intergroup comparison of gummy smile was performed with independent t-tests.
Results:
The surgical group presented significantly greater correction of the gummy smile with treatment than the BTX group.
Conclusion:
Gummy smile presented a greater improvement in patients treated with orthognathic surgery than with botulinum toxin application.
1. INTRODUCTION AND STATEMENT OF THE PROBLEM
The gummy smile is characterized by gingival overexposure during a smile and is one of the largest esthetic complaints of the patients [1, 2]. This problem is classified as the difference between the lower edge of the upper lip and the top edge of the maxillary central incisor [3, 4].
The causes of the gummy smile may be related to muscular, skeletal, periodontal and dental problems or combination of them; and maybe the result of a short upper lip, short crown of the teeth, excessive vertical maxillary gingival hypertrophy or hyperactivity of the upper lip levator muscle [5, 6]. Identification of the cause is important for planning the proper treatment [3].
The excessive gummy smile, for some people, represents an unfavorable esthetic, which affects self-esteem and psychosocial behavior [2]. According to previous studies, only when reaching 4mm of gingival exposure, the smile is considered unsightly, both by clinical dentists and by the laypeople [7, 8]. For some professionals, 2mm of gingival exposure is enough to compromise the smile [1, 3, 9].
Patients with a gummy smile can be treated exclusively with orthodontics, but depending on the bone deformity, alternatives should be proposed, such as clinical crown increase, Botulinum Toxin Application (BTX), and orthognathic surgery for maxillary impaction [1, 3-5, 9-11].
The use of BTX, compared to surgical procedures, is a less invasive, quick, safe and effective alternative that produces harmonic and pleasing results to the patient, when applied to the proper muscles (lift the upper lip, nose wing, zygomatic major and minor), respecting the appropriate dose and type of smile [12]. However, it presents a temporary effect of approximately 4 to 6 months, in the correction of the gummy smile [4, 8, 11, 13-15].
Several studies have demonstrated the applicability and effectiveness of gummy smile treatment with BTX [4, 11-14, 16] and also studies in orthognathic surgery demonstrate this improvement [10, 17-19]. Of our knowledge, there is no study comparing these two procedures for the correction of the gummy smile.
Therefore, the objective of this study was to compare gummy smile changes in patients treated with botulinum toxin application and orthognathic surgery for maxillary impaction.
2. MATERIALS AND METHODS
2.1. MATERIALS
This study was approved by the Ethics Committee in Human Research of the Ingá University Center (protocol n. 59231716.3.0000.5220) and all patients signed informed consent.
The sample size calculation was based on an alpha significance level of 5% (0.05) and a beta of 20% (0.20) to achieve 80% power of the test to detect a minimum difference of 1.17mm with a standard deviation of 1.4mm for the gingival display [11]. Thus, the sample size calculation showed the need for 23 individuals in each group.
Sample selection criteria included: the presence of all permanent teeth up to first molars with no extensive restorations in anterior teeth; Class I malocclusion with no anteroposterior skeletal discrepancy; indication for orthognathic surgery due to vertical maxillary excess with unpleasant gummy smile greater than 1mm before treatment.
Patients that did not agree to undergo orthognathic surgery and opted for compensatory orthodontic treatment had the option of receiving BTX therapy to reduce the gummy smile.
This way, the retrospective sample consisted of 61 adult patients divided into two groups:
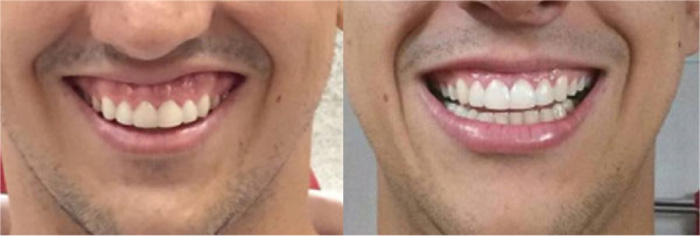
GROUP 1 (BTX): 38 patients (6 males and 32 females) who received BTX application, after the end of compensatory orthodontic treatment, with a mean age of 28.60 years (s.d. = 6.09). Photographs of a posed smile were taken before orthodontic treatment and 1 month after the BTX application (Fig. 1).
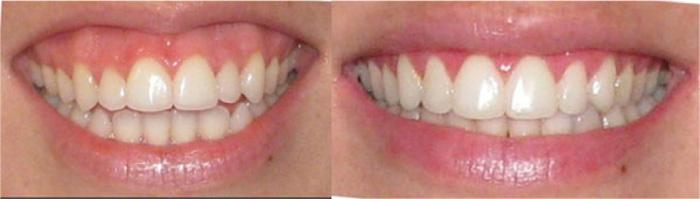
GROUP 2 (SURG): 23 patients (7 males and 16 females) who received orthodontic treatment and orthognathic surgery of maxillary impaction for correction of the gummy smile, at a mean age of 29.59 years (s.d. = 5.72, minimum 19.83 and maximum 40.66). Photographs of a posed smile were taken before the beginning of treatment and one month after the removal of the fixed orthodontic appliance (Fig. 2).
2.1.1. Group 1- Botulinum Toxin Application
In patients of the group 1, before the application of the BTX, the digital pressure maneuver was performed on the upper lip and the nasal wing and the zygomatic major and minor muscles, request the patient smile to evaluate the actual function that the muscle exerted and its need for treatment before the result in the improvement of the smile.
The application of BTX was performed after anamnesis and initial examination, treatment plan, frontal photographs (expression mimics), signed informed consent form, face hygiene, demarcation of the BTX application site with a white pencil (makeup), after analgesia with the application of 2 minutes of ice at the site.
Diluted solutions of BTX were applied in specific points to harmonize the gummy smile. The toxin used was Dysport (Ipsen Biopharm Lt, Wrexham, UK), and 1 ml of saline solution was diluted in the flask and then applied with a 0.3 ml syringe and 8 mm BD Ultra-Fine II needle.
The technique used in the application of BTX was 1 point on each side 2 mm below the nasolabial sulcus, at the level of the nostril, for inhibition of contraction of the upper lip and nose lift muscles. Two toxin units were used on each side (equivalent to 2 syringe risks 0.02ml BTX).
After the application, the recommendations to the patient were: head elevated for 4h; do not compress the region; do not perform physical activities for 24 hours, do not stay close to heat, and do not apply any type of cosmetic product on the skin for 24 hours.
2.1.2. Group 2 - Ortho-surgical Treatment
Patients of this group were submitted to orthodontic treatment and orthognathic surgery of maxillary impaction performed in a hospital under general anesthesia. The orthognathic surgery included Le Fort I osteotomy in the maxilla to correct the vertical excess, without mandibular surgery.
2.2. METHODS
The measurement of the gingival exposure was performed on frontal extraoral photographs of the posed smile before (T1) and after treatment (T2) in each patient, using the Corel Draw X5® software (CorelCorporation, Ottawa, Canada).
A spontaneous smile for staged photography is difficult to replicate. This way, patients were trained to smile as extreme as possible, until producing a squint with a noticeable decrease in the palpebral fissure, which refers to the distance between the open eyelids. Three photographs were taken at each time point for each patient, and the photograph with the greatest gingival exposure was chosen for measurement.
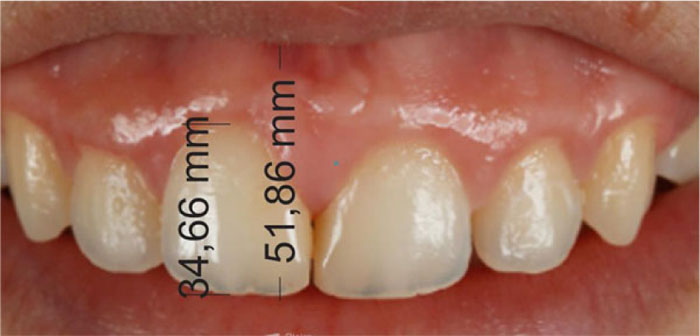
Gingival exposure (GING EXP) was defined as the distance between the stomion of the upper lip (UL) to the incisal edge of the maxillary central incisor (UL-Mx1) minus the length of the maxillary central incisor (Mx1).
For the magnification of the photographic measurements, a rule of three (proportion) was used with the real length of the maxillary central incisor (Real Mx1) performed on the dental casts of each patient with a digital caliper.
Real UL-Mx1= Photo UL-Mx1 x Real Mx1 / Photo Mx1
Then, Real UL-Mx1 subtracted the real value of the length of the Mx1, finding the measure of GING EXP (Fig. 3). Negative values of gingival exposure indicate that the upper lip is covering part of the maxillary central incisor. The gingival exposure of the right and left maxillary incisors of each patient was measured and averaged.
2.2.1. Error Study
Twenty new measurements were taken on photographs, randomly selected and re-measured in the Corel Draw software, after 30 days to determine the systematic (dependent t-test) and casual error (Dahlberg formula).
2.2.2. Statistical Analysis
Normality of the data was tested with the Shapiro-Wilk test and all variables present normal distribution, and then parametric tests were used.
The comparability of the groups of sex distribution was performed by Fisher's exact test. Comparability of the mean age of the groups was performed by an independent t-test.
Intergroup comparison of gingival exposure before (T1) and after treatment (T2) and changes with treatment (T2-T1) was performed by independent t-tests.
The tests were performed using Statistica software (Statistica for Windows, version 7, Statsoft, Tulsa, Oklahoma, USA). The data were considered significant for P <0.05.
3. RESULTS
There was no significant systematic error and the casual error for the GING EXP was 0.11mm.
Groups were comparable regarding sex distribution and initial age (Tables 1 and 2).
|
Sex Groups |
Female | Male | Total |
|---|---|---|---|
| 1- BTX | 32 | 6 | 38 |
| 2- SURG | 16 | 7 | 23 |
| Total | 48 | 13 | 61 |
| P value = 0.151 | |||
The surgical group presented significantly greater correction of the gummy smile with treatment than the BTX group (Table 2).
4. DISCUSSION
The esthetics of the smile presents a great perspective for the patient and has become a great challenge for the orthodontist and dentistry in general [1, 20]. In this context, the orthognathic surgery and the application of BTX gain space in search of a pleasant smile.
The groups presented similar gingival exposure before treatment (Table 2). Since the surgical-orthodontic treatment was recommended for all patients in both groups, the same severity of the malocclusion and the craniofacial discrepancy was expected.
The surgical group presented more reduction of gingival exposure with treatment than the BTX group (Table 2). This way, we can affirm that orthognathic surgery corrects significantly more the gummy smile than the botulinum toxin application (Table 2). However, one may think this is obvious since the greater initial severity of the gummy smile.
| Variables |
Group 1 - BTX (n=38) |
Group 2 - SURG (n=23) |
P-value | ||
|---|---|---|---|---|---|
| Mean | s.d. | Mean | s.d. | ||
| Initial Age (years) | 28.60 | 6.09 | 29.59 | 5.72 | 0.532 |
| GING EXP (T1) (mm) | 3.57 | 1.66 | 4.32 | 1.74 | 0.098 |
| GING EXP (T2) (mm) | 0.18 | 1.56 | -0.38 | 1.09 | 0.131 |
| GING EXP (T2-T1) (mm) | -3.39 | 1.59 | -4.70 | 2.15 | 0.008* |
The improvement of the gummy smile in the BTX group was greater than 3mm (Table 2). This was similar to other studies [7, 13, 14], but less than other studies [4, 11]. BTX corrected the gummy smile in the patients of the present study, but the final gingival exposure was still positive, i.e., gingiva showed some display after BTX application (Table 2).
The orthognathic surgery group showed a greater reduction of gingival exposure, and the final mean value was negative (Table 2), indicating that the upper lip was covering part of the maxillary central incisor.
Both treatments compared in the present study must be correctly indicated in each case individually.
The botulinum toxin application is a treatment that provides transitory improvement of the gummy smile, with some loss of the results in 6 to 8 months [11, 14]. However, it is an option less invasive and with a lower cost than orthognathic surgery.
Orthognathic surgery for maxillary impaction is an invasive alternative, with high cost, but it provides a definitive and stable result of the gummy smile correction [21, 22]. Besides, many of these patients that are submitted to orthodontic and orthognathic surgery presented other malocclusion features and craniofacial discrepancies than only the gummy smile. Then the improvement and benefit of this treatment extend to other aspects of the face and profile than only the gummy smile correction.
The BTX application can be used when surgical treatment is refused by the patients, like the patients in the present study [16]. Besides, both procedures can be combined to achieve a better result [10].
Moreover, maxillary lip repositioning surgery is an alternative procedure to correct the gummy smile and much less invasive than orthognathic surgery [23]. It should also be considered by patients and professionals when the patient refuses orthognathic surgery.
Besides the treatment protocols compared are different, both corrected the gummy smile on different levels; this must be considered in the treatment planning of each patient individually. When gingival exposure is severe, and more craniofacial deformities are involved, the best treatment planning is orthognathic surgery; however, if the gummy smile is not so severe, botulinum toxin injection is a viable treatment option, but with temporary results.
Limitations of the present study were the retrospectively obtained sample and the absence of an evaluation of patient satisfaction with both treatments.
CONCLUSION
There was a statistically significant difference in gummy smile changes between patients treated with the BTX application and orthognathic surgery with maxillary impaction.
Gummy smile presented significantly greater improvement in patients treated with orthognathic surgery than with botulinum toxin application.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
This study was approved by the Ethics Committee in Human Research of the Ingá University Center, Brazil (protocol n. 59231716.3.0000.5220).
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
CONSENT FOR PUBLICATION
All patients signed informed consent.
AVAILABILITY OF DATA AND MATERIALS
The data supporting the findings of the article is available upon request to the corresponding author [ K. M.S.F].
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflicts of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


