All published articles of this journal are available on ScienceDirect.
Endodontic Management of Hypercementosis in Conjunction with Asymptomatic Apical Periodontitis: A Case Report
Abstract
Introduction:
Hypercementosis is characterized by an excessive deposit of dental cementum. While it is considered a benign pathology, it can sometimes be associated with a chronic pulpal or periapical infection. Furthermore, its management is complex, because establishing an accurate apical limit for a root canal procedure is not always possible.
Methods:
When a periapical lesion is present, a conservative, surgical approach to remove the inflammatory tissue from the periapical lesion can be considered as a treatment option.
Conclusion:
This paper reports on the management of a tooth with hypercementosis accompanied by an asymptomatic apical periodontitis affecting a left mandibular second molar.
1. INTRODUCTION
Dental cementum is a specialized connective tissue that generally covers the entire root surface from the Cemento-Enamel Junction (CEJ) to the root apex, and serves as a medium for the attachment of fibers of the periodontal ligament. It is considered an adaptable component of the periodontium, which may respond to functional demands, and its formation is characterized by apposition throughout the functional stage of tooth life. Its position on the root may vary in two specific situations; 1) Cemental hypoplasia [1, 2]; and 2) A failure of the cementum to cover the dentin or unite with the enamel at the CEJ [3].
When cementum occurs in excess it is known as hypercementosis, which is the thickening or increase in the deposition of cementum on the root surface that may involve the entire root or appear nodular or bulbous around the root apex [4, 5]. While the etiology of hypercementosis is still uncertain, it has been associated with several local factors, such as chronic pulpal or periapical inflammation or infection, occlusal trauma, dental mobility, repair of root fractures, disorders during the deposition of cementum, absence of an antagonist, and so forth. Furthermore, genetic or systemic factors, such as thyroid and bone diseases, vitamin deficiency, calcinosis, have also been identified. Moreover, in some cases it is considered as being idiopathic in nature [4-8]. Radio-graphically, hypercementosis includes a thickening of the cementum layer, adjacent to the normal radicular cementum and is contained within the limits of the periodontal ligament and the lamina dura [4].
Apical periodontitis is an infection of the osseous tissue that emanates from the root canal system to the periapical tissues. It is characterized by host defense response to a microbial injury causing inflammation of the periodontal ligament and bone resorption [9].
The cementum is considered the least studied dental tissue and the literature on hypercementosis, as well as its etiology and treatment options is somewhat limited, with reports regarding hypercementosis and its endodontic management as being sparse [7].
2. CASE REPORT
A 51-year-old female patient was seen in the Department of Postgraduate Endodontics, Faculty of Dentistry, Pontificia Universidad Javeriana, reporting an episode of mild pain ten months prior to consultation located in the area of the left mandibular second molar (tooth 37), the patient remained asymptomatic since this mild pain episode. Her medical history was insignificant and she reported that no medications were being taken at this time.
The extra oral physical examination indicated no visible abnormalities, such as lymphadenopathy, swelling, and so forth. An intraoral examination revealed absence of a sinus tract, swelling or mobility, and there was no tenderness to palpation or percussion. A composite, intact resin restoration was present in the tooth.
The intraoral peri-apical radiograph showed a previous root canal procedure on tooth 37. There was a radiolucent area in the middle and apical third of the root, as well as in the furcation region that may or may not be contiguous with the apical radiolucency, as it appeared to be an isolated entity on a two-dimensional film. A radiolucent vertical line was also seen that extended to the area of the furcation, which may indicate the presence of a root fracture.
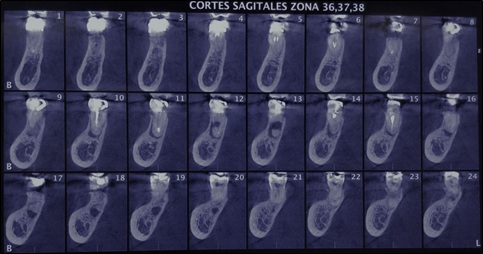
As an incidental finding at the level of the apical third, a thickening of the roots was observed due to the symmetrical and excessive deposition of a radiopaque material (hyper-cementosis). The periodontal ligament and lamina appeared normal (Fig. 1). The clinical and radiological findings were consistent with a diagnosis of asymptomatic apical periodontitis with hypercementosis. These initial findings were corroborated with a panoramic reconstruction (Fig. 2). In a preoperative tomography (CBCT) provided by the patient at the time of consultation, different sections presented with hyperdense roots and hypodense zones compatible with hypercementosis and apical periodontitis, respectively (Fig. 3). A treatment planning decision identified exploratory surgery, as a diagnostic way to rule out the possibility of a root fracture, due to the previously described radiographic findings. The prognosis the tooth was established as guarded.


Surgically, an intrasulcular tissue incision was made and a tissue flap was reflected from mesial of tooth 36 to distal of tooth 38. No radicular fracture was observed and the granulomatous tissue in the interradicular zone was curetted. A small dental crack was observed on the mesial surface of the distal root, which was removed with a conical bur at high speed. The reflected tissue was repositioned and the patient was instructed to attend follow-up appointments at 3, 6, 9, 12 months, with subsequent yearly assessments. Presently, the patient has not returned for the requested follow-up appointments, which often happens when there are no signs or symptoms. In this case, apical surgery was not performed due to the finding of hypercementosis and the impossibility of establishing an accurate apical limit in this condition.
3. DISCUSSION
Cementum is a specialized connective tissue that has the capacity to respond to functional demands. Excessive deposition of cement is known as hypercementosis, and this condition can be idiopathic or associated with local or systemic factors. It is usually associated with premolars and often appears symmetrically, as well as in both jaws. However, the mandible is associated with twice the frequency (68.2%) of hypercementosis teeth than that seen in the maxilla (31.8%) [4, 5].
The differential diagnosis may include any radiopaque structure that is seen in the vicinity of the root, such as a dense bone island or cemento-osseous dysplasia in mature stage [10]. There may be a resemblance to a small cementoblastoma. Cementoblastoma and hypercementosis are lesions associated with tooth roots that may, in some circumstances, challenge the clinician on their diagnosis. The differentiating characteristic is the presence of the periodontal membrane space around the hypercementosis [11].
Although hypercementosis and cementoblastoma are typical conditions with distinct clinical evolution, because cementoblastoma is a neoplasm with unlimited growth potential, the usual treatment is complete surgical removal, while no treatment is required for hypercementosis [11].
From an endodontic perspective, several authors suggest that a chronic periapical infection is one of the most common local factors that may contribute to the development of hypercementosis, which generally affects a single root with a bulbous pattern or nodular enlargement [4-6]. The periapical pathosis can be explained by a mild, chronic and low grade infection in the root canal system. Furthermore, with hyper-cementosis, the roughness of the root surface could promote bacterial contamination that leads to localized bone loss. It is important to make an adequate diagnosis, establish or identify etiological factors and eliminate them [4-6, 8].
Hypercementosis is completely asymptomatic and is considered as a finding in the radiographic examination. It may be associated with other types of pathologies, such as apical periodontitis as in the case of this patient, where hyper-cementosis was associated with a periapical injury due to a possible failure in previous root canal procedures [12]. In the case of highly infected root canals, bacterial substances have been detected near the dentin-cementum junction, which may have played an important role in the pathogenesis of hyper-cementosis in this patient.
In teeth with hypercementosis it is difficult to establish a relationship between the external anatomy of the apical third and the diameter of the main foramen or the number of apical foramina; these morphological characteristics could explain the difficulties in estimating the working length radiographically [13, 14]. In this case, non-surgical retreatment or apical surgery was not proposed, due to the fact that the patient was asymptomatic. Therefore, the treatment option was to perform a surgical approach as both a diagnostic procedure and to eliminate the inflammatory tissue associated with furcation radiolucency. The literature reports that the elimination of irritating agents such as tissue, cellular and bacterial remnants through a surgical process promotes healing of tissues, with all other case factors being noncontributory [9, 15].
It is still unknown whether or not multiple factors are required for the development of hypercementosis. Additionally, studies on the impact of hypercementosis on the nonsurgical treatment outcomes of root canal are still lacking. This issue is compounded by the fact that the apical limits for root canal preparation depend on different apical termination points and manner in which the presence of hypercementosis affects these decisions and attainments [13].
The use of CBCT technology has been advocated for many procedures in endodontics, although there exists considerable debate as to whether or not it should be used as a standard and routine imaging modality [16]. In a joint statement by the American Association of Endodontists and the American Academy of Oral and Maxillofacial Radiology in 2018 [17], it was emphasized that CBCT should not be used routinely for endodontic diagnosis or screening in the absence of clinical symptoms. In this case, the patient presented with a CBCT, which while helpful in assessing her problem, detailed information as to the nature of the field of vision, voxel size and exposure parameters were not available.
Presently, it is not possible to establish a definitive outcome for the treatment performed for this patient. Long-term follow-up is required to determine its effectiveness.
CONCLUSION
Apical periodontitis suggests that chronic apical infection is a predisposing factor for the development of hyper-cementosis that complicates traditional root canal procedures. In some cases, a surgical management may be necessary to determine and eliminate the etiologic factors.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Ethical approval was obtained from the committee of investigation and ethical of the School of Dentistry, Pontificia Universidad Javeriana, Bogotá-Colombia. (Ethical code # 39776130)
HUMAN AND ANIMAL RIGHTS
No animals were used in this research. All research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013. (http://ethics.iit.edu/ecodes/node/3931)
CONSENT FOR PUBLICATION
The participante provided written informed consent.
STANDARDS OF REPORTING
This study was carried out in accordance with the principles laid in CARE guideline.
AVAILABILITY OF DATA AND MATERIAL
The authors confirm that the data supporting the findings of this study are available within the article.
FUNDING
The funding is provided by the Vicerrectoría de Investigación at Pontificia Universidad Javeriana for this project. The grant code: 9162
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


